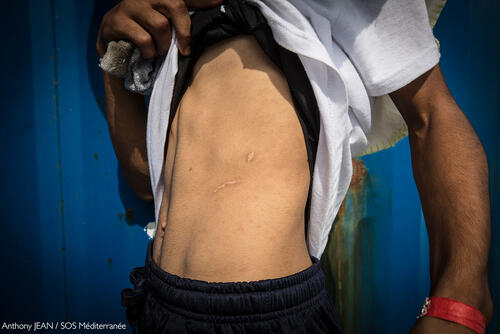
War, violence, natural disasters, disease outbreaks, rising inflation and spiralling prices; these factors all contributed to an overall increase in people’s needs, to which nearly 68,000 Médecins Sans Frontières (MSF) staff responded in more than 75 countries around the world in 2022.
Violence in Haiti
The highly volatile political, economic and security situation in Haiti deteriorated even further in 2022, leaving the country on the verge of collapse. Yet it yielded little international attention or assistance. Extreme levels of violence in the capital, Port-au-Prince, meant that some communities became trapped without access to food, water or medical care. We have achieved acceptance by the armed gangs who rule entire neighbourhoods, but they frequently target people on the streets and kidnap medical staff with virtual impunity.
MSF’s trauma hospital in Tabarre, and two stabilisation centres in Turgeau and Carrefour – all neighbourhoods in the capital – were often overwhelmed by the numbers of patients with violence-related injuries, particularly during an upsurge in fighting in May.
Our Drouillard hospital in the Cité Soleil neighbourhood is regularly at the crossroads of the armed groups’ territorial struggle, and the often intense violence forced our medical activities there to be suspended several times during the year. Haiti is currently one of the most challenging countries for MSF, in terms of security risk for our staff and supplies.
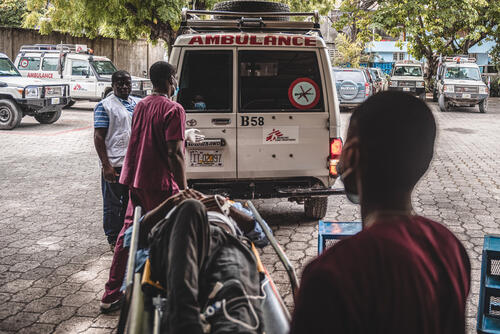
Escalation of war in Ukraine
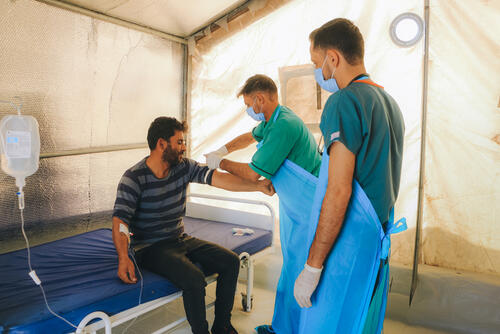
MSF has been active in eastern Ukraine, supporting people caught up in the war since it started in 2014. However, on 24 February 2022, our teams were taken by surprise by the dramatic escalation in conflict following large-scale attacks by Russian forces across the country. We rapidly increased our response, providing staff and materials, as well as training to Ukrainian surgeons and healthcare workers to help them cope with large influxes of wounded patients.
We assisted people who decided to stay home, those who moved elsewhere within the country, and the immense number who chose to seek refuge in neighbouring countries such as Poland, Moldova, Belarus and Russia, providing them with medical and mental healthcare.
The escalation of the war posed several challenges for us. We needed to rapidly scale up activities to respond to a wide range of needs – not only treating war-related physical and mental trauma but also pre-existing conditions such as non-communicable diseases – and adapt to the changing situation and fast-moving frontlines. We had to balance our ambition to deliver care where it was most needed with the necessity of guaranteeing the safety of our staff, including our many Ukrainian staff who had been displaced.
To address these challenges, we devised new ways to get as close to people as possible; for example, using a specially designed medical trains to transport patients away from danger zones; running mobile clinics in shelters for the displaced and in metro stations, where people took cover as bombs fell indiscriminately above ground; and opening phone hotlines for consultations for non-communicable diseases.

COVID-19’s lasting impact
At the beginning of 2022, as the pandemic entered its third year, MSF teams were still responding to COVID-19 in many places. We continued offering treatment in countries such as Iraq and Eswatini, and administering vaccinations in Lebanon, South Africa and Uganda.
Meanwhile, MSF’s Access Campaign highlighted the need for an intellectual property waiver that would facilitate greater and more rapid production of vaccines for this and future pandemics. While our response to COVID-19 decreased as the year wore on, our teams worked to address the toll the pandemic has taken on people and healthcare systems, such as a lack of routine vaccinations, which has led to outbreaks of vaccine-preventable diseases in many countries.
Cholera resurges
We saw an extraordinary resurgence of cholera in 2022; 30 countries recorded cases or outbreaks. MSF responded to this highly contagious disease in at least 10 countries, including Nigeria, Syria, Cameroon, Niger, Lebanon, Democratic Republic of Congo and Kenya. Different factors including natural disasters, climate change, water scarcity and humanitarian crises, such as conflict, contributed to the worldwide rise in cases.
In Haiti, after three years with no cases, there was a major outbreak from late September. By the end of the year, there had been over 15,000 cases, the vast majority of which were treated in our facilities. Our teams also supported outbreak vaccination efforts.
In view of the global shortage of cholera vaccines, the International Coordinating Group – of which MSF is a member – took the unprecedented decision to temporarily recommend a one-dose, rather than the usual two-dose, vaccination strategy to help protect more people from contracting the disease.
The climate crisis leaves its mark
Once again, in 2022, MSF assisted people affected by extreme weather events, such as floods in South Sudan and South Africa; drought in Somalia; and cyclones in Madagascar and the Philippines.
In January, MSF teams provided treatment to children with malnutrition on the outskirts of N’Djamena, Chad, in what was for some the driest and shortest rainy season they could remember. However, several months later in August, in the same area, unusually heavy seasonal rains caused rivers to burst their banks, leading to flooding, which displaced thousands of people.
In June, Pakistan was swept by severe floods, with one-third of the country underwater; some areas were still flooded more than three months later. The devastation displaced over 30 million people and left thousands dead and injured. In response, MSF teams provided medical, nutrition and water and sanitation support on a massive scale in Sindh and Balochistan provinces.
Towards the end of the year, we started working in Kiribati to improve maternal healthcare, particularly the diagnosis and treatment of diabetes, a disease that is prevalent in this Pacific Island nation, where rising sea levels have eroded and salinised land used to cultivate crops.
Rise in malnutrition cases
Treating high numbers of children with malnutrition was another focus of our activities during the year. As with cholera, the causes of malnutrition are complex and multifactorial; drought, bad harvests, collapsed health and economic systems, conflict, rising food prices. Some or a combination of these factors contributed to the alarming levels of malnutrition we saw in Nigeria, Ethiopia, Kenya, Afghanistan, Chad and Yemen during the year.
In Baidoa, Somalia, where the prolonged drought has been compounded by long-standing conflict and an inadequate humanitarian response, our teams were at times seeing 500 acutely malnourished children a week.

Migration pushbacks
The UN’s refugee agency, UNHCR, estimated that as many as 100 million people were forcibly displaced around the world in 2022https://www.unhcr.org/global-trends. Some were caught in a stalemate at the borders between Belarus and Latvia, Lithuania and Poland, where they were met with constant, often violent, pushbacks.
From the beginning of the year, we struggled to assist people in these areas due to hostile policies restricting our access. The escalation of the war in Ukraine in late February, however, revealed a double standard in European migration policies; for millions of Ukrainians – fleeing conflict, like many of the people stranded at the Belarusian border – entry to EU countries as refugees was swiftly facilitated.
Refugees and migrants arriving at Mexico’s northern border also continued to be pushed back by the US under Title 42, a decades-old policy that has been widely used only since March 2020, to regulate border crossings under the premise of increased COVID-19 precautions. Meanwhile, thousands of migrants heading for the Mediterranean coast in northern Africa – or retreating from the dangers in Libya – were expelled from Algeria to Niger and abandoned on the border in the middle of the desert.
Pushbacks continued at sea as well; in September, Malta forced a ship to take people rescued from its search and rescue zone in the Central Mediterranean Sea to Egypt, in clear violation of maritime and international law.
In the five years since over 750,000 Rohingya fled Rakhine state, in Myanmar, following indescribable violence, life for the persecuted minority has not improved. Those arriving by boat to seek safety in Malaysia have been forcibly returned to sea or have been arrested, imprisoned, and charged. In Bangladesh, Rohingya live in cramped and unsanitary conditions, and their right to move around the camp of 1 million people and work has been severely restricted, adding to people’s distress.

Successes in TB, but challenges remain
At the end of the year, the New England Journal of Medicine published results from our TB-PRACTECAL clinical trial, which tested the efficacy and safety of a six-month, all-oral treatment regimen for drug-resistant tuberculosis (DR-TB).
The regimen cured 90 per cent of patients, a significant improvement on previous standard treatments, which typically took two years to complete, with only around half of patients cured. It has now been included in the World Health Organization’s updated TB treatment guidelines.
Scale-up of shorter, all-oral regimens will be critical to getting people on treatment and cured. But this can only happen if the drugs used in these regimens are affordable. Prices for bedaquiline and delamanid, which are being used in our PRACTECAL and/or endTB and endTB-Q trials, remain too high for wide-scale use in many high-burden countries, and must come down.
Like PRACTECAL, the endTB and endTB-Q trials are also looking at shorter, safer, more effective regimens, including in patients who are minors. This is doubly important following WHO’s new recommended algorithm to diagnose TB in children.
The impact of anti-NGO rhetoric on MSF activities
Across some parts of the world, our teams continued to see the effects of counterterrorism and anti-NGO rhetoric. Four colleagues from our team in Southwest region, Cameroon, were arrested and charged with complicity with secessionists after they transported a patient with a gunshot wound in an ambulance to hospital in Mamfe.
They spent between 10 months and just over a year in prison, before being acquitted in court at the end of December. Due to the lack of guarantees for our safety, we were forced to first suspend, and then close, our project in Mamfe, which further reduced the availability of healthcare in an area with immense needs.
Access to healthcare remained an issue in Tigray, and other parts of Ethiopia, in the year following the June 2021 murders of our colleagues María, Yohannes and Tedros. Since then, we have tried relentlessly to understand the full circumstances behind what happened to our colleagues and obtain an acknowledgment of responsibility for the events leading to their murders. Despite the heavy investment made in bilateral engagement with the authorities, the lack of progress in obtaining substantial answers led MSF Spain to pull out of the country.
In Afghanistan, the Islamic Emirate of Afghanistan (also known as the Taliban) has continued to strip away freedoms for women in the year since retaking power in August 2021. In December, edicts were issued restricting girls’ and women’s access to education, and banning female NGO workers, with an informal exemption for those working in healthcare. While we can retain women on our teams – for now – we are deeply worried about the longer term, as female medical students cannot complete their education to become the doctors, nurses and specialists that the country’s health system desperately needs.
Our teams have witnessed the criminalisation of the delivery of aid in some places, including in Mali and Niger. This has made it extremely difficult to reach people caught up in conflict in the Sahel border region of Niger, Mali and Burkina Faso.
Our work has its risks, with staff working under the threat of attack, abduction, or detention. Despite the challenges in this part of the Sahel, and elsewhere we worked during 2022, our teams managed to deliver lifesaving care to millions of people. But this work would not have been possible without the support of our nearly 7 million donors, for whom we are grateful.
*MSF Directors of Operations - Dr Ahmed Abd-elrahman, Dr Marc Biot, Akke Boere, Dr Sal Ha Issoufou, Kenneth Lavelle, Isabelle Mouniaman, Teresa Sancristoval.