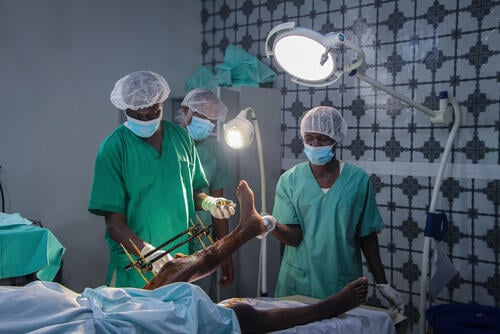
We run some of our largest programmes in the Democratic Republic of Congo (DRC). In 2019, we worked in 21 of out of the country's 26 provinces and responded to one of the biggest outbreaks of measles in decades. We also worked with people displaced by conflict, and those with health problems such as HIV/AIDS.
People have little access to healthcare, and disease outbreaks are frequent due to poor surveillance and infrastructure. Violence has led to crises in the Kivus, Tanganyika and Kasai regions, and has forced millions to flee. Three of our staff, abducted in North Kivu in 2013, are still missing.
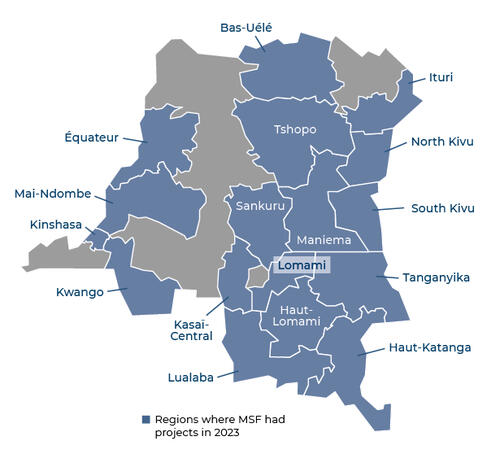
Our main areas of activity in DRC


Armed conflict has triggered massive movements of people and their needs are immense. We provide emergency responses in the areas affected, notably currently in North and South Kivu, Kasai, Ituri and Tanganyika among others. We treat the wounded, cover basic health needs and adapt our services accordingly.

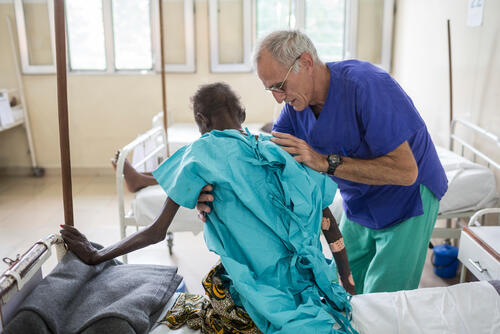
We support the national HIV/AIDS programme, which is implemented by the country's health authorities. Our teams work on improving access to screening and treatment, reinforcing treatment adherence, and patient retention. Awareness-raising through community-based activities is an important part of our projects.

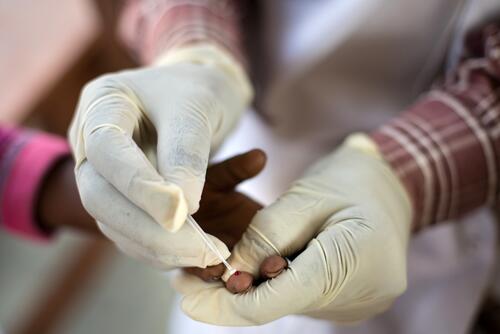
According to official statistics in DRC, malaria causes four times more deaths per year than conflict, meningitis, cholera, measles and respiratory diseases combined. Children are the most severely affected. Most of our projects include malaria care. We also carry out emergency interventions to contain outbreaks.

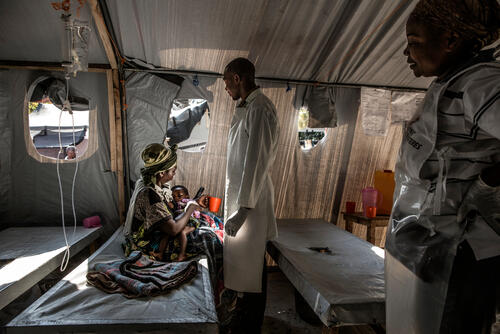
DRC is prone to outbreaks of infectious diseases, such as measles, yellow fever and cholera. We run mobile teams, which can be quickly deployed in emergencies. Among our responses to outbreaks of communicable diseases are vaccination campaigns, case management (including surgeries), health promotion and water and sanitation activities. Ebola outbreaks are also recurrent in DRC, and we support local authorities in the response.
Read more on recent Ebola outbreaks in DRC

Many of our projects have an important component of women's health. Sexual violence is also a major issue in DRC, affecting men and boys as well as women and girls. We provide medical and psychological support, organise family planning activities, antenatal and postnatal consultations, and treat patients for sexually transmitted diseases.


In 2017, we observed an increase in admissions for malnutrition in all our medical structures. This is due to violence-triggered displacement, a bad agricultural season, and less funding. We are treating malnutrition in North Kivu, South Kivu and Kasai provinces.
Our activities in 2023 in DRC
Data and information from the International Activity Report 2023.
2,890
2,89
€139.3 M
139.3M
1977
1977

2,578,300
2,578,3
1,495,400
1,495,4
779,800
779,8

29,000
29,
14,100
14,1
1,410
1,41

Violence against civilians must end in DRC as second MSF staff killed in Masisi

MSF condemns deadly shooting at Kyeshero hospital, Goma

Civilians and MSF teams trapped by violence in Walikale, DRC

New wave of violence in Ituri, DRC, further risks civilian lives

MSF adjusts emergency response around Goma amid mass departures from displacement camps

People are trapped in a climate of insecurity amidst clashes in parts of South Kivu

DRC: Statement following the passing of our colleague

Democratic Republic of Congo: MSF staff member critically injured in Masisi town after shots hit MSF base

DRC: Injured seek treatment from MSF-supported hospitals in Bukavu amid fighting
Reports & Analysis

Fexinidazole: A doctor's dream
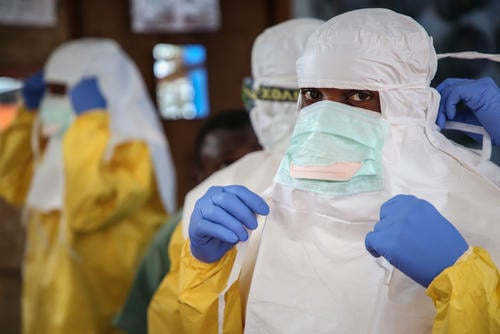
Ebola in the DRC: between operational trial and error and scientific uncertainty
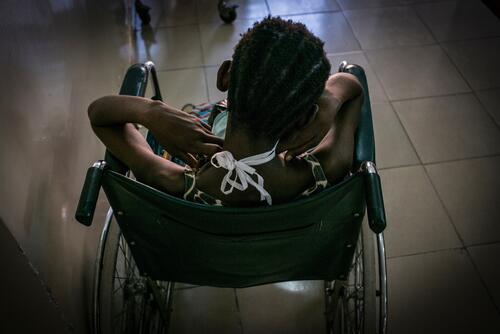
Left behind by the HIV response - Kinshasa

Violence and its humanitarian impact: the case of Kivu