In Haiti, we provide care to victims of trauma, survivors of sexual and gender-based violence, as well as sexual and reproductive care. With natural disasters regularly occurring in the country, emergency response also remains a central aspect of our work in the country.
Since the assassination of the Haitian President in 2021, the people of the capital Port-au-Prince have been struggling to survive as armed gangs, police, and civilian self-defence brigades fight in the streets of the city. The already volatile situation has been deteriorating even further after an announcement on 28 February 2024 that elections would be postponed until as late as August 2025. More than 15,000 people were displaced in Port-au-Prince within just one week in early March.
We are scaling up our medical activities to care for the mounting number of people injured in the escalating violence and political unrest that has engulfed the city.
Our teams currently run two trauma hospitals in Tabarre and Carrefour, two emergency centres in Drouillard and Turgeau, and one centre for survivors of sexual violence in the Port-au-Prince metropolitan area. Mobile clinics have been temporarily suspended due to the volatile situation.
What we do in Haiti


Armed clashes continue to affect communities in Haiti’s capital, Port-au-Prince. While maintaining functioning medical structures during these clashes is a challenge, with kidnappings and armed robberies rampant across Port-au-Prince, we have continued to provide trauma care. Our teams treat people with gunshot and stab wounds, severe burns, and victims of road accidents in several medical facilities across the capital.


The prevalence of sexual and gender-based violence (SGBV) is a continuing concern in Haiti. We support multiple health facilities in providing care dedicated to victims of SGBV that includes medical, psychological, and social care. The introduction of a free telephone helpline has increased accessto care, offering victims remote psychological support and referrals to health centres.


Sexual and reproductive care remains an essential area of activity for our teams in Haiti. We are providing women with proper prenatal and neonatal care to continue our work on reducing the maternal and infant mortality rate. We also provide recreational and educational activities to promote family planning and sexually transmitted disease prevention and management.

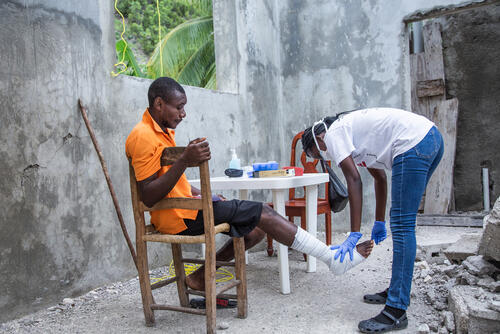
With enduring armed clashes and frequent natural disasters, our teams conduct emergency operations in Haiti. Water and sanitation support is provided to communities affected by the violence in Port-au-Prince. After an earthquake in August 2021, we provided emergency care to victims that included surgery, water and sanitation support and mobile clinics to rural areas.
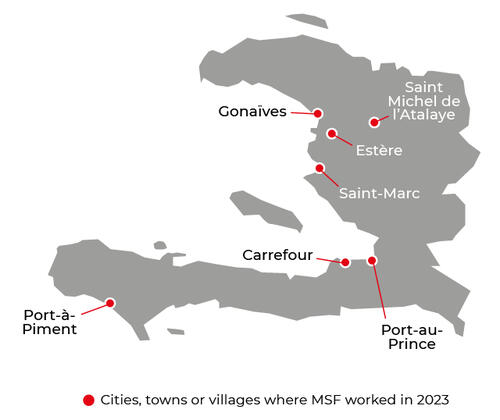
Our activities in 2023 in Haiti
Data and information from the International Activity Report 2023.
1,968
1,968
€49.6 M
49.6M
1991
1991

37,600
37,6
4,200
4,2
5,780
5,78

1,420
1,42

Haiti: MSF withdraws from two medical facilities in Port-au-Prince as widespread violence intensifies

MSF vehicles shot during hospital evacuation amid escalating violence in Port-au-Prince

In Haiti, escalating violence increases displacement and basic needs

Providing support to victims and survivors of sexual violence in Port-au-Prince

MSF partially resumes medical activities in Port-au-Prince

Violence and threats by police force MSF to suspend activities in Port-au-Prince metropolitan area

MSF outraged by police attack on ambulance and execution of patients in Haiti

Rapid and safe access to medical care must be guaranteed in Port-au-Prince







