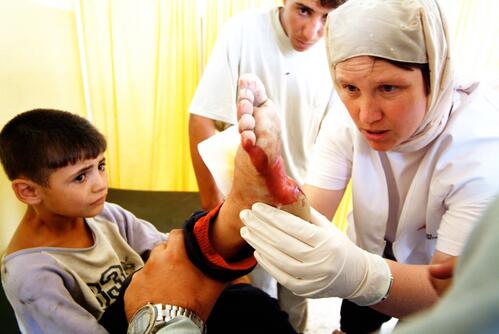
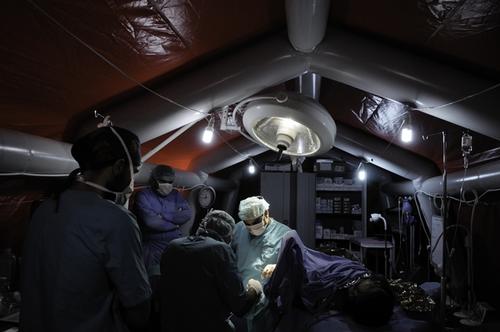
More than one third of our projects are dedicated to providing assistance to people living in areas of war and armed conflict such as Central African Republic, Iraq, Nigeria, South Sudan, Syria and Yemen, among many others.
The consequences of war
The consequences of war can be vast and catastrophic; from death and violence; to long-term lifechanging injuries and post-traumatic stress disorder; destroyed infrastructure and healthcare systems; as well as people being uprooted and forced to leave everything behind.
In war zones, our teams endeavour to assess and treat the most pressing needs; we don’t take sides but address people’s medical and humanitarian needs first and foremost.
We also speak out about the situations faced by the people we strive to help, including in war zones. We will continue to provide assistance to people in distress, regardless of their race, religion, creed or political convictions.
Since the creation of MSF in 1971, our teams have provided care in myriad wars and conflicts and violent contexts. We have addressed both the immediate and long-term medical needs from Afghanistan, the Balkans, Colombia, and the Democratic Republic of Congo, to Iraq, Rwanda, Syria, Yemen and many more.
Direct consequences of war
War and conflict have an immediate and direct impact on people’s lives. After seven years of war, Yemen illustrates the devastation wreaked by indiscriminate or targeted attacks that kill and injure people, and shatter civilian infrastructure.
Trauma injuries surge during armed conflict, calling for increased emergency care. Today, our teams focus on treating both fresh war wounds and long-lasting injuries, through emergency trauma care as well as reconstructive surgery.
In Amman, Jordan, for example, our reconstructive surgery hospital provides plastic, maxillofacial, and orthopaedic surgery, in tandem with physiotherapy for war-wounded people from across the region.
Indirect consequences of war
During war and conflict regular medical needs climb as healthcare services collapse. Pregnant women, or people with chronic diseases such as diabetes or HIV, are left particularly vulnerable. As commodities become scarce, the price of basic food and domestic items soar, while fear, insecurity, and loss generate psychological distress.
We regularly see an increase in sexual violence during conflict. Sometimes, rape is used to subdue a community. For example, a group of at least 10 women were gang-raped in February 2018 near Bossangoa, western Central African Republic by men from a local armed group who took them hostage. With ongoing conflict in the area, it took the women a month to get medical care.
In 2020, nearly 11,000 people were assisted by our teams in DRC for physical and psychological conditions related to sexual violence. Sixty three per cent reported having been raped by armed men.
In conflict settings, depending on the priorities, we may set up operating theatres, clinics, nutrition programmes, epidemic control, medical care for victims of sexual violence, and maternity wards, among other services.

Twice Victims
Forced from home
Conflict often uproots people from their homes, leaving them displaced in their own country or as refugees in another. According to the UNHCR, at the end of 2020, the total number of forcibly displaced people worldwide was 82.4 million. Our teams provide medical care to those who are displaced by conflict, often in refugee and displaced people's camps.
In the Central African Republic (CAR), millions of people have been displaced during years of bloody conflict. Our teams see the direct consequences of violence on the health of individuals and entire communities we serve. Wounded people needing care. Children unable to reach medical facilities during malaria season. The interruption of vaccination programmes and treatment for HIV and tuberculosis (TB). Women left without assistance before, during and after giving birth.
Treacherous journeys and precarious conditions at the place of destination jeopardise health and well-being. In Syria, for example, millions of people have been internally displaced due to the conflict that has been ongoing for over a decade and are living in displacement camps.
In such settings, people stuck in limbo without access to proper education, medical care, or even water and sanitation services, are dangerously exposed to various conditions and risks, including mental health issues, violence, and diseases such as cholera, measles and hepatitis.

Epidemics
Conflict and displacement can be catalysts for epidemics and disease outbreaks, due to a lack of access to water, sanitation and medical care.
Living in cramped and unsanitary conditions can be an ideal breeding ground for cholera or measles. Insecurity and collapsed health systems cut people off from receiving preventative healthcare, including vaccinations.
In CAR, for example, routine vaccination coverage plummeted after the country plunged into violence and instability in 2013. The vaccination coverage rate for measles fell from 64 per cent to 25 per cent. In response, in 2016 we organised a mass vaccination campaign with the Ministry of Health, immunising 220,000 children under five years old.
Mental health
Whether treating children who have been uprooted and witnessed horrific conflicts, or people who have survived torture and sexual violence, our teams of psychologists and psychiatrists strive to address the pressing mental health needs for people affected by war and conflict.
The terrifying sound of bombs falling above your head, or bullets puncturing your bedroom walls, or watching your family being murdered in front of you, or perhaps being tortured by armed groups. This has been the reality for a generation of people from countries like Iraq, Syria, Libya and beyond, where our teams see patients with serious mental health issues linked to such experiences – such as post-traumatic stress disorder.
In the past 10 years, mental health consultations in our projects have risen by 230 per cent worldwide and a large proportion of the needs we have addressed are consequences of people affected by war, violence and conflict.
In many areas of the world there are very few if any providers of comprehensive mental health services – this often means we have to create our own programmes.
In addition to the lack of services, come taboos, stigmas and suspicion surrounding mental health. We therefore have to work with communities to spread awareness regarding the importance of mental health. Despite the varying challenges of treating people affected by conflict, treating psychological needs in such settings remains a priority for our teams.

Mental Health in Iraq
We don’t take sides
In conflict zones, we do not take sides. It’s crucial for us to talk with all parties in a conflict to obtain access and provide assistance to affected communities. We will speak out about the suffering we observe, as well as any gross violations we may witness while providing assistance to people caught up in war and conflict.
One of the ways we can maintain our independence is to ensure that all our funding for work in conflicts comes from private donors. Globally we accept very few government grants – three per cent of our total funding – and in war zones we do not use funds from governments that have any sort of tie with the conflict.
Despite not supporting any of the warring parties, we are not always present on all sides of a conflict. This may be either because access is not granted to us by one or more of the parties, or due to insecurity, or because the main needs of people are already covered.
In Syria, for example, we are only able to work in some areas controlled by armed opposition groups. Violence and insecurity, attacks on health facilities and medical workers, and the absence of government authorisation to work in Syria have been some of the main obstacles to extending direct medical activities to all areas.
The needs of people who fall victim to war and conflict are vast and complex, and so our medical response is never the same – from treating trauma and long-lasting debilitating war wounds, to the psychological impact of war and violence, to supporting destroyed health systems and responding to epidemics and diseases as people have been uprooted and find themselves in precarious conditions.
Our teams do not always have the capacity to fill every gap, however, we always put people in need first and provide them with the best medical care possible, no matter where they are from, what they believe in, or who they support.