Since the civil war of 2013, CAR has been marked by cycles of intensive violence. Fighting between the government and non-state armed groups, spurred by an election process, escalated in early 2021.
MSF sees the direct consequences of violence on the health of individuals and entire communities. There is a severe lack of access to healthcare; trained health workers are scarce, health services are poorly resourced and often targeted by the conflict; and patients need to travel hundreds of kilometres on dangerous roads to reach medical structures.
In CAR, we focus on treating victims and survivors of sexual violence; provide sexual and reproductive healthcare, including maternal healthcare; and provide treatment to people living with HIV.
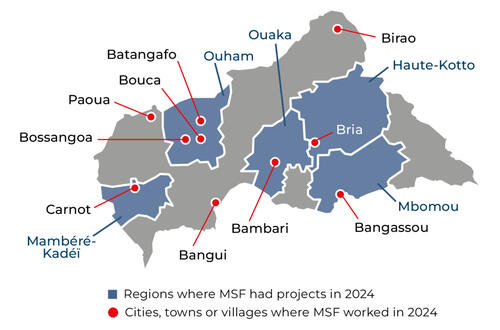
Our activities in 2024 in Central African Republic
Data and information from the International Activity Report 2024.
2,379
2,379
€68.1 M
68.1M
1997
1997

543,600
543,6
324,800
324,8
10,300
10,3

4,820
4,82

Two MSF staff members released in Central African Republic

Two MSF staff members detained in Central African Republic



Invisible Wounds: MSF findings on sexual violence in CAR between 2018 and 2022

Sexual violence in Central African Republic is a “public health emergency”

Abortion: Women more at risk of death in fragile and conflict-affected settings

Attacks against staff and patients in Batangafo threaten continuation of healthcare




