Why did game-changing tools not work to their full effect?
In August 2018, the authorities in the Democratic Republic of Congo (DRC) declared an Ebola outbreak, which turned out to be the largest the country had ever known. The epidemic spread through communities in North Kivu and Ituri provinces that were already severely affected by decades of armed conflict.
This time, it seemed that we were better prepared to respond than in previous Ebola outbreaks; we had new ‘game-changers’ – tools that could potentially bring the outbreak to a quick end. These tools, which could perhaps determine the length and extent of the outbreak, included two vaccines and two therapeutic drugs. From the start, we had one vaccine with proven efficacy. During the outbreak, Médecins Sans Frontières (MSF) participated in a clinical trial that determined two new therapeutic drugs were effective to treat the disease, and we tested a second new vaccine to reduce transmission. Despite the proven efficacy of these new tools, two of every three people with Ebola died and the virus continued to spread for more than 18 months.
With the promising resources at hand, we should have been able to reduce the number of deaths and number of new cases. But this did not happen. People slipped through the net and were not cared for by those responding to the Ebola outbreak. At some points in the epidemic, more than half of Ebola-related deaths were occurring within the community, with people never reaching Ebola treatment centres (ETCs). Those who did, arrived too late, when treatments were less likely to prevent a fatal outcome.
Why didn’t these game-changers have a greater impact?
The care proposed by the Ebola response did not always meet patients’ needs, including those who were not sick with Ebola. Having not gained the trust of the community, the response was perceived by people as hostile. Often, people were offered care in isolation, far away from their families and communities. Considering people perceived the mortality rate for Ebola patients in the ETCs to be high, for many, the proposed healthcare was not reassuring enough and did not offer much.
In North Kivu and Ituri provinces, Ebola is often not the top health priority. People in these areas face other life-threatening diseases such as measles, malaria and malnutrition, as well as a strained health system impacted by the ongoing armed conflict. The overall response was centred on the Ebola outbreak rather than patient and community health needs. It absorbed a lot of the fragile health system’s already limited resources, leaving many seriously sick people without critical care. The failure to focus on local-level coordination and provide an individualised response for patients in each disease hotspot meant that MSF and other organisations tackling the disease were unable to obtain the trust and acceptance of the communities.
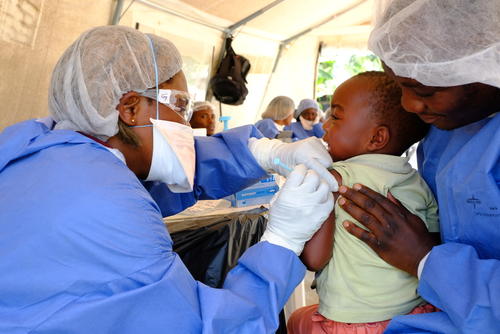
An important way of reducing the number of people infected with Ebola is preventing ongoing transmission through vaccination. The strategy implemented by the response in DRC was to vaccinate people who had been in close contact with confirmed Ebola patients, and people in contact with those contacts. Despite the effective vaccine, identifying contacts proved difficult in practice, with fewer people qualifying for vaccination, thereby limiting the effectiveness of the targeted vaccination strategy. The restricted supply of the vaccine also impacted the strategy’s implementation and its unregistered status made vaccination time-consuming. Overall, the vaccination strategy applied did not prevent the further spread of the virus quickly enough. Initially, MSF focused on vaccinating frontline workers. As the outbreak continued, we pushed for an adapted strategy that would reach more people and we participated in the testing of a second vaccine.
How do we address these issues in the future?
To get the best of any new ‘game-changers’ in an outbreak response, community ownership and social mobilisation are vital. For this to be achieved, patients and communities must clearly see the benefits of the response.
We have progressively moved away from Ebola-centric approaches to focus on the overall needs of communities. This includes decentralising Ebola triage to existing MSF healthcare facilities so that both Ebola and non-Ebola care is addressed and is closer to communities, conducting more outreach activities so that patients can seek our assistance before it is too late.
We also need to make sure treatment is adapted to specific patient needs, rather than treating everyone the same way. For some patients, it may be possible to provide home-based care; others could be treated in smaller health units closer to where they live. Some people at risk of infection may benefit from the prompt use of post-exposure prophylaxis treatment, while others may need to go to a health centre on a regular basis.
In terms of prevention during an outbreak, we should also facilitate the development and testing of more vaccines and diverse vaccination strategies, adapted to context and addressing the expectations of communities. They should be easy to use in the context of an outbreak, with fast-tracked licensing if needed, while the vaccination strategy should facilitate access for those that need it. To better respond to future Ebola outbreaks, the medical response strategies should not be viewed alone. Patient-centred approaches and community ownership are the real game-changers.