Cholera is a water-borne, acute gastrointestinal infection caused by the Vibrio cholerae bacterium. It is transmitted by contaminated water or food, or direct contact with contaminated surfaces. In non-endemic areas, large outbreaks can occur suddenly, and the infection can spread rapidly. Most people will not get sick or will suffer only a mild infection, but the illness can be very severe, causing profuse watery diarrhoea and vomiting that can lead to severe dehydration and death within a few hours after the start of symptoms. Treatment consists of a rehydration solution – administered orally or intravenously – which replaces lost fluids and salts. Cholera is most common in densely populated settings where sanitation is poor and water supplies are not safe.
As soon as an outbreak is suspected, patients are treated in centres where infection control precautions are taken to avoid further transmission of the disease. Strict hygiene practices must be implemented, and large quantities of safe water must be available. An oral vaccine is available as both a preventive measure and to respond during outbreaks.
MSF treated 47,000 people for cholera in 2019.
Ebola is a virus that is transmitted through contact with the bodily fluids of an infected person, including someone who is deceased, or through surfaces contaminated with these fluids. Ebola first appeared in 1976, and although its origins are unknown, bats are considered the likely host. MSF has intervened in almost all reported Ebola outbreaks in recent years, but until 2014 these were usually geographically contained and involved more remote locations. Ebola has a mortality rate of between 25 and 90 per cent and starts with flu-like symptoms, followed by vomiting and diarrhoea, symptoms that are common to many illnesses. As the disease progresses, people in some cases experience haemorrhaging, and death. Despite being so deadly, it is a fragile virus that can be easily killed with sunshine, heat, bleach, chlorine, and even soap and water. Two investigational vaccines are available to help protect health workers and the contacts of infected people. Anti-viral drugs have also been used in outbreaks to treat people on compassionate use and investigational bases. Otherwise, patient care is centred on rehydration and treating the symptoms such as fever and nausea.
Preventing transmission is essential: patients are cared for in Ebola treatment centres where strict infection control procedures are reinforced. Identifying people the patient was in contact with when they were ill becomes a priority to protect them and prevent further transmission, as do safe burials. Community health promotion is also important to inform the community about the risk of exposure and how to try and keep themselves safe, and what to do if they develop symptoms of the disease.
MSF treated 910 people for haemorrhagic fevers, including Ebola, in 2019.
Health promotion activities aim to improve health and encourage the effective use of health services. Health promotion is a two-way process: understanding the culture and practices of a community is as important as providing information.
During outbreaks, MSF provides people with information on how the disease is transmitted and how to prevent it, what signs to look for, and what to do if someone becomes ill. If MSF is responding to an outbreak of cholera, for example, teams work to explain the importance of good hygiene practices because the disease is transmitted through contaminated water or food, or direct contact with contaminated surfaces.
Hepatitis C is a liver disease caused by the blood-borne hepatitis C virus (HCV). It is most commonly transmitted through unsafe injection practices, reuse or inadequate sterilisation of medical equipment, and the transfusion of unscreened blood and blood products.
The virus can cause both acute and chronic infection, ranging in severity from a mild illness lasting a few weeks to serious, lifelong illness. Infected people often do not show symptoms for many years, although those with acute infection may experience fever, fatigue, decreased appetite, nausea, vomiting, abdominal pain, dark urine, joint pain and jaundice.
It is estimated that 71 million people are chronically infected with hepatitis C. The disease kills an estimated 400,000 people each year, the vast majority of whom live in low- and middle-income countries where there is little or no access to diagnosis and treatment. While hepatitis C is found worldwide, central and east Asia, Egypt, China, and Pakistan are the regions and countries most affected.
In the last few years, new drugs called direct-acting antivirals (DAAs) have been developed that allow for treatment to be given orally, with few side effects, over a course of three months. These new drugs are very effective – with different combinations curing well over 95 per cent of patients – but can be very expensive in high- and middle-income countries. Prices for a three-month course of treatment in wealthy countries started at well above US$100,000, and treatment remains unaffordable for many, particularly in middle-income countries. Through the use of generic DAAs, MSF has been able to secure a price of just $75 per treatment in most projects.
MSF started 10,000 people on hepatitis C treatment in 11 countries in 2019.
The human immunodeficiency virus (HIV) is transmitted through blood and body fluids and gradually breaks down the immune system – usually over a three- to 15-year period, most commonly 10 years – leading to acquired immunodeficiency syndrome, or AIDS. As immunodeficiency progresses, people begin to suffer from opportunistic infections. The most common opportunistic infection that often leads to death is tuberculosis.
Simple blood tests can confirm HIV status, but many people live for years without symptoms and may not know they have been infected. Combinations of drugs known as antiretrovirals (ARVs) help combat the virus and enable people to live longer, healthier lives without their immune systems deteriorating rapidly. ARVs also significantly reduce the likelihood of the virus being transmitted.
As well as treatment, MSF’s comprehensive HIV/AIDS programmes generally include health promotion and awareness activities, condom distribution, HIV testing, counselling, and prevention of mother-to-child transmission (PMTCT) services. PMTCT involves the administration of ARV treatment to the mother during and after pregnancy, labour and breastfeeding, and to the infant just after birth.
In 2019, 144,800 people were on first-line or second-line ARV treatment under direct MSF care or in MSF-supported programmes.
Largely unknown in high-income countries, kala azar – Hindi for ‘black fever’ – is a tropical, parasitic disease transmitted through bites from certain types of sandfly. Of the estimated 50,000 – 90,000 annual cases, 90 per cent occur in Brazil, Ethiopia, India, Kenya, Somalia, South Sudan and Sudan, where the disease is endemic. Kala azar is characterised by fever, weight loss, enlargement of the liver and spleen, anaemia, and immune-system deficiencies. Without treatment, kala azar is almost always fatal.
Today, liposomal amphotericin B is becoming the primary treatment drug in Asia, either alone or as part of a combination therapy. While safer and shorter than previously used medication, it requires intravenous administration, which remains an obstacle to its use in local clinics. An oral drug, miltefosine, is often added to optimise treatment regimens in some patients. In Africa, the best available treatment is still a combination of pentavalent antimonials and paromomycin, which is toxic and requires a number of painful injections. Research into other treatment combinations is underway.
Co-infection of kala azar and HIV is a major challenge, as the diseases influence each other in a vicious spiral as they attack and weaken the immune system.
MSF treated 1,970 patients for kala azar in 2019.
Malaria is transmitted by infected mosquitoes. Symptoms include fever, pain in the joints, shivering, headache, repeated vomiting, convulsions and coma. Severe malaria, nearly always caused by the Plasmodium falciparum parasite, causes organ damage and leads to death if left untreated. MSF field research has helped prove that artemisinin-based combination therapy (ACT) is currently the most effective treatment for malaria caused by Plasmodium falciparum. MSF also piloted the use of injectable artesunate for the treatment of severe malaria in many countries.
Long-lasting insecticide-treated bed nets are one important means of controlling malaria. In endemic areas, MSF prioritises the distribution of bed nets to pregnant women and children under the age of five, who are most vulnerable and have the highest frequency of severe malaria. Staff advise people on how to use the nets.
Since 2012, MSF is also strongly involved in prevention strategies, such as ‘seasonal malaria chemoprevention’ (SMC), based on the use of anti-malarial drugs, implemented in the Sahel, in which children under five take oral antimalarial treatment monthly over a period of three to four months during the peak malaria season.
MSF treated 2,638,200 malaria cases in 2019.
Two of the most immediate causes of malnutrition are a reduced intake of food and/or essential nutrients and repeated episodes of illness which go untreated. Children under five, adolescents, pregnant or breastfeeding women, the elderly, and the chronically ill (e.g. with HIV, TB, diabetes) are the most vulnerable to malnutrition.
Acute malnutrition in children is usually categorised in two ways: it can be calculated from a ratio using weight and height or weight and age; or by measuring the mid-upper arm circumference (MUAC). Different measurements are used for different age groups. According to these measurements, malnourished children are diagnosed with moderate or severe acute malnutrition. Their clinical status and appetite is then assessed to determine whether they should be treated in hospital or receive outpatient care.
In outpatient clinics, MSF uses ready-to-use therapeutic food (RUTF) along with supportive medical treatment. Ideally, local foods should be used to treat malnutrition, but with RUTF’s long shelf-life which requires no preparation, these nutritional products can be used in all kinds of settings and allow malnourished patients to be treated at home, unless they are suffering severe medical complications. Malnourished children with medical complications are treated in hospital with therapeutic milks designed to stabilise their metabolism, and medication to treat their other illnesses. In situations where malnutrition is likely to become severe, MSF takes a preventive approach with our nutritional activities to cover at-risk individuals and prevent their condition from deteriorating further.
MSF admitted 76,400 malnourished children to inpatient feeding programmes and registered 109,300 admissions to outpatient feeding programmes in 2019.
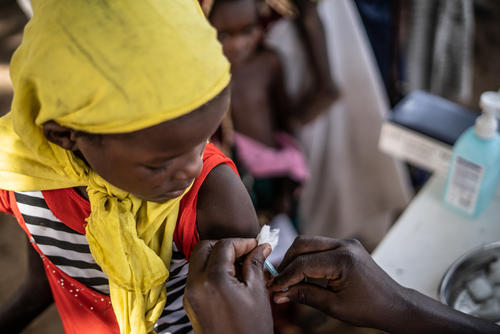
Measles is a highly contagious viral disease. Symptoms appear on average 10 days after exposure to the virus and include a high fever, rash, runny nose, cough and conjunctivitis. There is no specific treatment against measles; all patients receive vitamin A to prevent eye complications, antibiotics to prevent respiratory tract infections, and nutritional support. Other case-based care can include treating symptoms for stomatitis (a yeast infection in the mouth) and dehydration.
In high-income countries, most people infected with measles recover within two to three weeks, and mortality rates are low. In low- and middle-income countries, however, the mortality rate can be up to 10 per cent, rising to 20 per cent in outbreaks with limited access to care. Death is mostly due to severe respiratory infections, such as pneumonia; diarrhoea and stomatitis that can lead to malnutrition; and, more rarely, neurological complications such as encephalitis (inflammation of the brain).
A safe and cost-effective vaccine against measles exists, and large-scale vaccination campaigns have significantly decreased the number of cases and deaths. However, large numbers of children are left susceptible to the disease, especially in countries with weak health systems, where outbreaks are frequent and where there is limited access to health services.
MSF carried out 1,320,100 vaccinations against measles in response to outbreaks in 2019.
Meningococcal meningitis is a bacterial infection of the thin membranes surrounding the brain and spinal cord. Symptoms may occur one to four days after infection. It can cause sudden and intense headaches, fever, nausea, vomiting, sensitivity to light and stiffness of the neck. The infection can progress rapidly, and death can follow within hours of the onset of symptoms. However, even with treatment, up to 10 per cent of people infected can die; in the absence of treatment this may rise to 50 per cent. Among survivors, 10 to 20 per cent are left with lifelong conditions such as deafness, intellectual disability and epilepsy.
Six strains of the bacterium Neisseria meningitidis (A, B, C, W135, X and Y) are known to cause meningitis. People can be carriers without showing symptoms and transmit the bacteria when they cough or sneeze. Cases are diagnosed through the examination of a sample of spinal fluid and treated with specific antibiotics.
Meningitis occurs throughout the world, but the majority of infections and deaths are in Africa, particularly across the ‘meningitis belt’, an east–west geographical strip from Ethiopia to Senegal. Prior to the introduction of a meningitis A conjugate vaccine in 2010, epidemics were mostly caused by meningococcus A. The first large-scale meningococcal C epidemic was recorded in Niger and Nigeria in 2015. Conjugate vaccines against multiple meningococcus strains (ACWY) are in extreme shortage, are very expensive and are therefore impossible to use for wide-scale preventive campaigns. However, a new meningococcus conjugate vaccine against the ACWYX strains is currently being developed and expected to be available at an affordable price in 2021 or 2022.
In total, MSF vaccinated 197,700 people against meningitis in response to outbreaks in 2019.
Mental healthcare refers to any type of activity that aims to protect or promote mental wellbeing of communities; to prevent the development of mental health conditions; and to treat or alleviate psychological suffering of people experiencing mental health problems and disorders, while improving their ability to continue performing life’s daily activities.
These goals are achieved by supporting people in using their strengths, developing their individual and collective adaptation strategies, reconnecting to their support networks, and managing their emotions, through individual, group, family and community interventions. These interventions are counselling, psychological support, medication, and other psychosocial activities.
People caught up in natural and man-made disasters, epidemics, war and conflict have an increased risk of experiencing distress and mental disorders. For this reason, mental healthcare is an essential part of MSF interventions.
MSF staff provided 400,200 individual mental health consultations and 104,200 consultations in group sessions in 2019.
MSF’s primary focus is on providing medical care, but in an emergency, teams often organise the distribution of relief items that are essential for survival. Such items include clothing, blankets, bedding, shelter, cleaning materials, cooking utensils and fuel. In many emergencies, relief items are distributed as kits. Cooking kits contain a stove, pots, plates, cups, cutlery and a jerrycan so that people can prepare meals, while a washing kit includes soap, shampoo, toothbrushes, toothpaste and laundry soap.
Where people are without shelter, and materials are not locally available, MSF distributes emergency supplies – rope and plastic sheeting or tents – with the aim of ensuring a shelter. In cold climates more substantial tents are provided, or teams try to find more permanent structures.
MSF distributed relief kits to 346,900 families in 2019.
Emergency obstetrics and newborn care are an important part of MSF’s work. Medical staff assist births, performing caesarean sections when necessary and feasible, and mothers and newborns receive appropriate care during and after delivery.
Many of MSF’s programmes offer more extensive maternal healthcare. Several ante- and postnatal visits are recommended and include, where needed, prevention of mother-to-child transmission of HIV. Contraceptive services are offered, and safe abortion care is available. The need for medical care for terminations of pregnancy is obvious: in 2019, MSF treated over 25,800 women and girls with abortion-related concerns and complications, many of which resulted from unsafe attempts to terminate pregnancy; we also provided safe abortion care to over 21,500 women and girls who requested it.
Skilled birth attendance and immediate postnatal care can prevent obstetric fistulas, a stigmatising medical condition resulting in chronic incontinence. MSF provides surgical care for fistula repair in some of the most remote areas.
Since 2012, MSF has piloted cervical cancer screening and treatment. Human papillomavirus infection is the main cause of cervical cancer and particularly affects HIV-positive women.
MSF assisted 302,600 births, including 27,300 caesarean sections in 2019.
Sexual violence occurs in all societies and in all contexts at any time. Destabilisation often results in increased levels of violence, including sexual violence. Sexual violence is particularly complex and stigmatising, has long-lasting consequences, and can result in important physical and psychological health risks.
MSF medical care for victims of sexual violence covers preventive treatment against sexually transmitted infections, including HIV, syphilis and gonorrhoea, and vaccinations for tetanus and hepatitis B. Treatment of physical injuries, psychological support and the prevention and management of unwanted pregnancy are also part of systematic care. MSF provides a medical certificate to all victims of violence.
Medical care is central to MSF’s response to sexual violence, but stigma and fear may prevent many victims from coming forward. A proactive approach is necessary to raise awareness about the medical consequences of sexual violence and the availability of care. Where MSF sees large numbers of victims – especially in areas of conflict – advocacy aims to raise awareness among local authorities, as well as the armed forces when they are involved in the assaults.
MSF provided medical care to 28,800 victims of sexual violence in 2019.
Generally known as sleeping sickness, human African trypanosomiasis is a parasitic infection transmitted by tsetse flies that occurs in sub-Saharan Africa. In its latter stage, it attacks the central nervous system, causing severe neurological disorders and death if left untreated. More than 98 per cent of reported cases are caused by the parasite Trypanosoma brucei gambiense, which is found in western and central Africa. The reported number of new cases fell by 96 per cent between 1999 and 2018 (from around 28,000 to 977).
During the first stage, the disease is relatively easy to treat but difficult to diagnose, as symptoms such as fever and weakness are non-specific. The second stage begins when the parasite invades the central nervous system and the infected person begins to show neurological or psychiatric symptoms, such as poor coordination, confusion, convulsions and sleep disturbance. Accurate diagnosis of the illness requires three different laboratory tests, including a sample of spinal fluid.
A new drug, fexinidazole – the first all-oral treatment that works for both stages of the disease – has been developed by Drugs for Neglected Diseases initiative (DNDi) and received approval in late 2018. While it is being made gradually available, nifurtimox-eflornithine combination therapy or NECT, is a safe, highly effective but cumbersome treatment developed by MSF, DNDi and Epicentre in 2009.
MSF treated 48 people for sleeping sickness in 2019.
One-third of the world’s population is currently infected with the tuberculosis (TB) bacillus, but they have a latent form of the disease and so have no symptoms and cannot transmit it. In some people, the latent TB infection progresses to acute TB, often due to a weak immune system. Every year, over 10 million people develop active TB and 1.6 million die from it.
TB is spread through the air when infected people cough or sneeze. Not everyone infected with TB becomes ill, but 10 per cent will develop active TB at some point in their lives. The disease most often affects the lungs. Symptoms include a persistent cough, fever, weight loss, chest pain and breathlessness in the lead-up to death. Among people living with HIV, TB incidence is much higher, and is the leading cause of death.
Diagnosis of pulmonary TB depends on a sputum sample, which can be difficult to obtain from children. A molecular test that can give results in two hours and can detect a certain level of drug resistance is now being used, but it is costly and still requires a sputum sample, as well as a reliable power supply.
A course of treatment for uncomplicated TB takes a minimum of six months. When patients are resistant to the two most powerful first-line antibiotics (isoniazid and rifampicin), they are considered to have multidrug-resistant TB (MDR-TB). MDR-TB is not impossible to treat, but the drug regimen is arduous, can take up to two years and cause serious side effects. Extensively drug-resistant tuberculosis (XDR-TB) is identified when patients show resistance to the second-line drugs administered for MDR-TB. The treatment options for XDR-TB are very limited. Three of the newest drugs – bedaquiline, delamanid and pretomanid – can improve treatment outcomes for patients with drug-resistant versions of the disease, but their availability is currently limited.
MSF started 18,800 patients on treatment for TB in 2019, including 2,000 for MDR-TB.
Immunisation is one of the most cost-effective medical interventions in public health; according to the World Health Organization, vaccination with a series of vaccines recommended by WHO and MSF prevents 2 – 3 million deaths each year. Currently, these vaccines are BCG (against tuberculosis), poliomyelitis, DTP (diphtheria, tetanus, pertussis), hepatitis B, Haemophilius influenzae type b (Hib), conjugate pneumococcal, rotavirus, measles rubella, yellow fever, and human papillomavirus – although not all vaccines are recommended everywhere.
In countries where vaccination coverage is generally low, MSF strives to offer routine vaccinations for children under five as part of our basic healthcare programme. Vaccination also forms a key part of MSF’s response to outbreaks of vaccine-preventable diseases such as measles, cholera, yellow fever, and meningitis. In humanitarian emergencies, frequently involving population displacements or the rapid deterioration of living conditions and health, MSF conducts large-scale preventive campaigns to reduce the burden of vaccine-preventable diseases as well as to reduce the risk of outbreaks, such as measles or cholera.
MSF carried out 2,271,900 routine vaccinations in 2019.
Safe water and good sanitation are essential to medical activities. MSF teams make sure there is a clean water supply and a waste management system in all the health facilities where it works.
In emergencies, MSF assists in the provision of safe water and adequate sanitation. Drinking water and waste disposal are among the first priorities. Where a safe water source cannot be found close by, water in containers is trucked in. Staff conduct information campaigns to promote the use of sanitation facilities and ensure good hygiene practices.