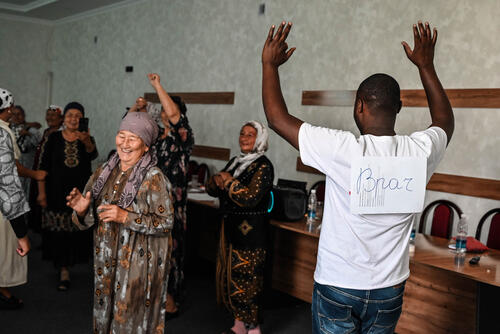For people who have lived through violence or natural disasters, survival goes beyond ensuring physical wellbeing. Even after their physical injuries have been treated, hidden psychological wounds can remain. To help heal the patient’s psychological wounds, MSF professionals are there to listen, support and provide mental healthcare, so the traumatic experiences do not come to define their lives.
According to the World Health Organization, around the world one in four people will suffer some kind of mental health disorder, yet about 60 per cent of sufferers do not seek help. This percentage is likely to increase dramatically when factors such as persecution, the need to flee armed conflict and natural disasters, and a lack of access vital healthcare are added. This is why we place a great deal of importance on providing mental healthcare during humanitarian emergencies.
In 1998, MSF formally recognised the importance of providing mental healthcare as part of our emergency work. More than 25 years later and, in 2023, our staff provided over 493,900 individual mental health consultations. The psychosocial support we provide through these consultations and groups focuses on helping people to develop coping strategies after they have lived through traumatic experiences. The immediate goal is to reduce their symptoms and help them be able to lead a normal life.
"I'm not a criminal"
For people caught in their wake, humanitarian crises can cause intense mental suffering. Many of the people assisted by us have been separated from their families or witnessed the deaths of loved ones. Others have spent much of their time on the run, searching for shelter and safety. Being forced from home is a particular problem for people who are already suffering from psychological disorders, as they lose access to treatment and routine care, which can cause them to develop more severe conditions.
The Malakal Protection of Civilian site, in South Sudan, was designed to provide protection to the local population affected by violence. Yet, difficult living conditions, a loss of hope, feelings of imprisonment and limited opportunities for work have affected the mental health of those living inside the camp. In 2016, we saw increasing numbers of suicides and attempted suicides, even among children.
On the Greek island of Lesbos, in Moria camp ─ which fires destroyed in September 2020 ─ the policy of indefinitely detaining asylum seekers had a severe impact on the mental health of the 13,000 people held there. The uncertain situation affected all those detained there, particularly children. During a group mental health activity for children (between 6 and 18 years) in 2018, an MSF team observed that nearly 25 per cent of children had self-harmed, attempted suicide or had thought about committing suicide. Many children were suffering from panic attacks and constant nightmares.
She always walks with a knife and says she will harm herself. I've already found a knife twice under her pillow. When I leave her alone, she always keeps her head down and cries.Fatima*, a refugee living in Moria camp, Greece, tells how the conditions have affected her 14 year-old daughter
Many people, in many countries around the world, are experiencing stress and/or anxiety during the current coronavirus COVID-19 pandemic. MSF teams are providing mental healthcare to people affected by the pandemic, and have offered tips on how to manage stress.
Challenges for providing mental healthcare
People face many barriers preventing them from accessing mental healthcare. One is that many do not understand what it is, how it might help them or that they might even need it. Psychologist Deborah Duarte recalls the challenge of accessing refugees arriving at the Daadab camp in Kenya. "These people did not know the impact their experiences had had on their physical and mental health. They only noticed their conditions when they could go no further without help", she says.
Other obstacles to providing psychological support in our projects are language and cultural barriers, the short amount of contact time between professionals and patients, and the social stigma that often accompanies mental ill-health.
Different approaches
Each situation requires a different approach from MSF’s teams of counsellors, psychologists and psychiatrists. In some cases, counsellors are trained to help people talk about their experiences, process their feelings, and learn to deal with them. In other cases, psychologists conduct individual therapy sessions, often with a specific focus.
Amir* is being treated by MSF in the city of Sulaymaniyah, in southern Iraq. He left his home in Salaheddin when the self-proclaimed Islamic State group besieged his town and cut off food supplies. He began to suffer from anxiety and insomnia. "I think too much, I get anxious and I cannot sleep. I stay awake all night, sitting in a corner until the morning. As a result, I get sick. In the past, I had pain in my stomach and chest. I visited doctors and they did not help me. But when I started to be treated by the MSF psychologist, it was very helpful to me. He encouraged me to make sure I get out of my tent every day and socialise with other people, to play sports, and to avoid being alone at home."

Another aspect to mental healthcare is psycho-education, where communities are taught about the importance of mental healthcare and to be aware of the signs and symptoms that they should look out for. Psycho-education, as well as counselling, can be done in groups, which may have predetermined themes connected to the situation.
Our teams use creative approaches to help raise awareness about the importance of psychological care. In Mweso, a town in eastern Democratic Republic of Congo (DRC) with many internally-displaced people living alongside a host community, our mental health counsellors became performers. They connect with audiences of up to 200 people through music, dance and dramatic scenes. Their performances inform people that MSF is in the community and is there to listen and to help them.
I think too much, I get anxious and I cannot sleep. I stay awake all night, sitting in a corner until the morning. As a result, I get sick.Amir*, a patient now being treated by MSF in Sulaymaniyah, southern Iraq
In all cases, it is essential to understand the structures that exist in the communities where patients live, and the emotional support these can offer. When our mental health teams begin work in a new community, one of their first steps is to seek out local leaders, who can guide the team on the strategies that will best match people’s needs. Communities often need to rebuild themselves as a whole to help strengthen the identities of the people within them.
In many cases, members of the MSF mental health teams will actually be from the communities being assisted, which can be very useful. They are aware of the social taboos around mental health in their communities, as well as the traumatic events which people have been or are being subjected to.
"As counsellors, we help our patients by listening to them, but we can also connect with them through the experiences we share,” explains Stanley, an MSF counsellor in DRC. “When someone comes to us suffering because he has lost his house, I say, 'Oh, you lost your home. I understand that you are deeply affected by this. I was also like that.' Our sessions are foremost conducted to help our patients, but reflecting on our shared experiences allows us, as counsellors, to be comforted as well."

The local context and its specific details will determine the best way for us to support the community in question. Psychosocial support teams are there to help individuals and communities access the tools they already have inside to rebuild themselves.
For this work to be done, there is yet another important mental health concern: that of the MSF professionals. Often far away from home, under the pressure of emergency work, and required to process the traumatic stories of the people they meet, they often also need a listening space where they can share their anguish and any other issues.
Returning home after working in an MSF project is often the time when psychological support becomes most necessary. This is when our staff need to rediscover who they are and return to their lives having had experiences that may have left psychological marks. Many struggle with the knowledge that for many of their patients, returning home is not an option and that there is still a long way to go. However, it is an essential process that they find meaning for the experiences they had and re-adapt to a normal routine. Only after that, if they want, will they be ready for a new project, where they can care for the visible and invisible wounds of their patients.
*Names changed to protect patients' privacy