14,500
14,5
240
24
33
33
Mozambique is one of the countries with the highest rates of HIV and TB worldwide.<a href="https://www.who.int/tb/publications/global_report/gtbr2018_annex2.pdf?ua=1">WHO Global Tuberculosis Report 2018</a>
In 2018, Médecins Sans Frontières teams in Maputo and Beira focused on improving the detection and rapid treatment of opportunistic infections among people with advanced HIV, by implementing a specialised package of care and support for people facing the challenge of staying on lifelong treatment or those developing drug resistance.
In Maputo, an MSF feasibility study into the use of liposomal doxorubicin to treat Kaposi’s sarcoma, the most frequent cancer affecting people with advanced HIV, showed better outcomes than other available treatments. We treated over 240 patients with this newer drug in 2018 and started advocating to push down the price and get the national treatment guidelines updated.
We started 160 patients on treatment for drug-resistant TB (DR-TB) in six health centres in Maputo in 2018; 70 per cent of those patients received less toxic, injection-free treatments. Preliminary positive results from an MSF feasibility study into DR-TB short regimens enabled the Ministry of Health to adopt them as national policy in June.
We partnered with a local organisation to open a drop-in centre for people who use drugs in Maputo. The centre, which offers testing and treatment for HIV, TB and hepatitis C, and comprehensive harm reduction services, including a needles and syringes distribution programme, received around 100 visitors a day.
We also launched a pilot project to prevent mother-to-child transmission of hepatitis B in one of the biggest hospitals in Maputo.
In Beira, as part of our project for key populations, teams offered sexual and reproductive healthcare, including HIV testing and treatment, to vulnerable and stigmatised groups such as sex workers and men who have sex with men. Around 300 people were enrolled in a pre-exposure prophylaxis study to prevent them from contracting HIV.
We also ran sexual and reproductive health services for girls and women at a local health centre, where we offer safe abortion care to reduce high mortality rates and suffering seen among women and girls without access to such services.
In 2018, we handed over our HIV project in Tete to the Ministry of Health. For 16 years, our teams in Tete had been working on innovative approaches to scale up HIV care, including community antiretroviral (ARV) treatment groups and a community initiative to monitor and address supply issues around HIV and TB drugs.
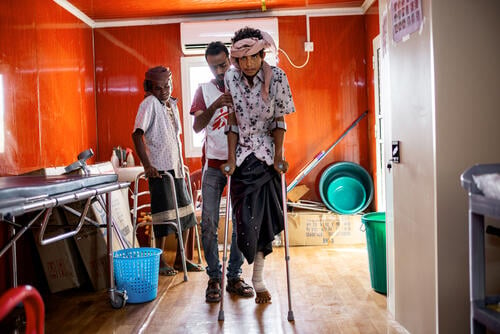
Filipe's story
“I lost my dad early. My mom is very old and has not been able to support me. I didn’t have money to buy food, I didn’t have money to pay for my education. When I moved to Beira, I started working as a sex worker. If I did not sell sex, I wouldn’t have anything to eat. After a while, I fell sick with gonorrhea, no clients wanted to see me anymore. That was when I came in touch with MSF’s community educator, who helped refer me to the hospital. I wouldn’t have gone otherwise, I didn’t even have the money to get there. Eventually, I applied to become an MSF peer educator myself. It has changed my life for the better – now I have stopped selling sex and instead get to help people that are in the same situation that I was in.”