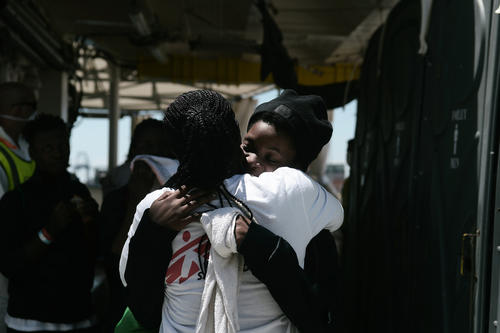In 2018 Médecins Sans Frontières (MSF) teams provided medical and humanitarian assistance to people facing extreme hardship in over 70 countries. From treating war-wounded ever closer to frontlines in Yemen, to responding to epidemic outbreaks such as cholera in Niger, or providing assistance to people fleeing violence in the Central African Republic, emergency response continued to be a core part of our work.
As 2018 drew to a close, the Democratic Republic of Congo (DRC) was in the midst of its second Ebola outbreak of the year, and its biggest ever. MSF was part of the response, led by the Ministry of Health.
Although rapid and well-resourced, with teams having access to a promising new vaccine and several new drugs with the potential to better protect and treat people, the response, and those managing it, failed to adapt to people’s priorities, and to gain the trust of the community.
This lack of trust in the health services meant people delayed or avoided seeking treatment. By the end of the year, the epidemic in North Kivu and Ituri provinces had claimed more than 360 lives and in some areas was still not under control.
Seeking care in war zones
Early in the year, Syrian civilians and medical staff were caught in the violence in Idlib, in the northwest, and in East Ghouta, near the capital Damascus. In East Ghouta, the barrage was relentless in February and March, with waves of dead and injured arriving at MSF-supported hospitals and health posts.
As the siege blocked incoming aid, medical staff had few medical supplies to work with. By the end of the offensive, 19 of the 20 hospitals and clinics we supported were destroyed or abandoned, leaving civilians with few options to seek medical help.
The war in Yemen, which has left the country and its healthcare system in ruins, entered its fourth year. The Saudi- and Emirati -led coalition continued to target civilian areas with airstrikes and bombings, including our new cholera treatment centre in Abs. The war is taking a heavy toll on people, who often must negotiate constantly changing frontlines to find care for their war-wounds or their general medical needs.
Yemen was the country where our teams treated the highest number of war-wounded in 2018, over 16,000 people. After a major offensive was launched in Hodeidah in June, doctors in our Aden hospital treated Hodeidah residents who had been driven for six hours, the majority of them in a critical condition.
Conflict intensified on several frontlines at the end of the year, leading to an influx of people with war-related injuries. We also treated more than 150 people wounded by mines planted by Houthi-led Ansar Allah troops around Mocha. Constant attacks on our staff and patients at facilities in Ad Dhale forced us to withdraw from the town in November.

The consequences of deterrence and detainment migration policies
The number of MSF projects working with displaced people has more than doubled since 2012. Record numbers of people have left their homes in search of safety, but many only encounter more violence, abuse and exploitation along the way.
In trying to escape extreme levels of violence at home, people from the Northern Triangle of Central America – Guatemala, Honduras and El Salvador – are exposed to shocking brutality on their routes north through Mexico to the United States. This takes its toll, and we treat the mental, as well as the physical, injuries of people who are kidnapped, raped, tortured and exploited.
In the Mediterranean, those attempting to make the dangerous crossing from Libya are frequently intercepted by the Libyan coastguard. Funded by European governments, the coastguard is implementing the EU’s policy of push-back and deterrence. People who are picked up by the coastguard are returned to awful conditions in detention centres, where our access to them is severely restricted.
Across the world in 2018, countries reinforced borders in a bid to keep out migrants and refugees. Governments attempted to cover up the human cost of their harmful policies by demonising, threatening and ultimately blocking some of our efforts to bear witness and provide assistance.
We were forced to end our search and rescue operations in the Central Mediterranean in early December after increasingly obstructive actions by European governments, particularly Italy, which shut its ports to migrant rescue boats, despite an estimated 2,297 people having drowned while attempting to flee Libya during the year.
In October, the Nauruan government expelled our team with just 24 hours’ notice, with no more explanation than that ‘our services were no longer required’. Until then, we had been providing desperately needed mental healthcare to local people and asylum seekers held on Nauru as part of Australia’s offshore detention policy.
Treating visible and invisible wounds
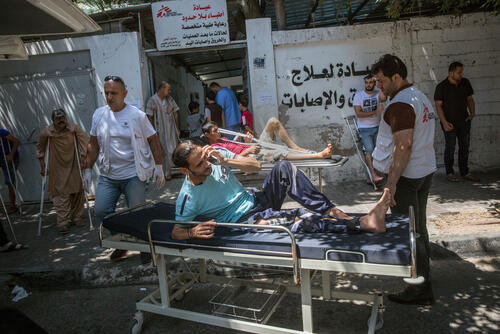
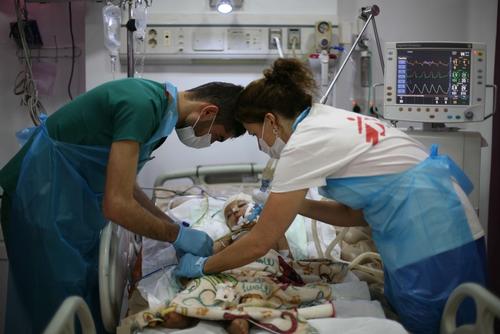
From March, the Israeli army responded with brute force to the ‘March of Return’ protests in Gaza, firing on people and leaving thousands with horrific gunshot injuries, mostly to the legs.
Our surgical teams were overwhelmed by the number of patients with severe and complex wounds; in 2018, teams in Palestine performed over 3,000 major surgical interventions, compared with 400 in 2017. Patients and medical staff now face the challenge of long-term rehabilitation and multiple surgical procedures, while trying to avoid the high risk of infection, in an enclave with limited resources due to the 11-year blockade.
In the Central African Republic, a cycle of revenge and retaliatory violence escalated, particularly in Bangui and Bambari in April and May, and in Batangafo in November. Our teams provided surgical care to war-wounded patients and were twice forced to activate mass casualty plans in Bangui. However, fighting prevented us from reaching many of the injured people who had fled into the bush.
We also addressed people’s invisible wounds, running mental health services in 54 countries. In 2018, MSF released a number of reports that highlighted the grave mental health situation of refugees and displaced people in particular, including alarming rates of mental illness and thoughts of suicide among people stuck on Lesbos in Greece and on Nauru, and in camps in South Sudan. We ran group and individual counselling sessions for refugees in these countries, as well as in Mexico, Bangladesh and Liberia.

Displaced people out of the spotlight
In Ethiopia, ethnic violence, high insecurity, and a lack of support in their places of origin forced at least 1.4 million people to become internally displaced in multiple, simultaneous and massive displacement crises. Most people left their houses with close to nothing and needed food, shelter, water and psychosocial support.
Our teams worked in camps in the country’s south and west, where overcrowding and poor sanitation facilitated the spread of conditions such as diarrhoea and skin infections.
The forced relocation of displaced people and the barriers to the impartial delivery of aid were constant dilemmas faced by humanitarian organisations. Ethiopia is also now host to the second-largest refugee population in Africa, mainly Eritreans, Somalis and South Sudanese.
In northeast Nigeria, nearly two million people have been displaced across Borno and Yobe states by the ongoing conflict. Rann town in Borno came under attack on 1 March – for the second time in just over a year – forcing us to temporarily suspend activities. We worked in 17 locations across the two states in 2018, where hundreds of thousands of people remain heavily dependent on aid for their survival, with hundreds of thousands more in areas inaccessible to humanitarian organisations.
Medical achievements improve patient care
In November, MSF’s partner organisation Drugs for Neglected Diseases initiative (DNDi) received approval for fexinidazole, a sleeping sickness drug that is safer, easier to administer and more effective than previous treatments. MSF projects trialled fexinidazole, which is the first new chemical entity to be developed by DNDi.
Ninety-seven per cent of unsafe abortions and related deaths occur in Africa, Latin America and southern and western Asia, and over the last two years, a significant effort has been made to increase access to safe abortion care in MSF projects in these regions. In 2018, around 70 projects in 25 countries reported providing safe termination of pregnancy to over 11,000 women and girls who requested it.
Our continuous drive to improve the quality of diagnostics led us to expand our investment in point-of-care ultrasound. We also developed eCARE, an algorithm to support paediatric diagnostic capacity, which substantially increases health workers' compliance with guidelines and decreases the use of unnecessary antibiotics.
MSF’s Access Campaign continues to advocate better access to key sofosbuvir-based drug combinations, used to treat hepatitis C. This enabled our teams to scale up and simplify treatment in a number of countries in 2018, including Cambodia, where we also introduced a simplified diagnostic process that has significantly reduced the time between screening and the start of treatment.
Our work is not without its risks. Our teams provide care under the threat of detention, abduction and attack; our thoughts remain with Romy, Richard and Philippe, our colleagues abducted in DRC in July 2013, who remain missing.
MSF Directors of Operations:
Dr Marc Biot
Dr Isabelle Defourny
Marcel Langenbach
Kenneth Lavelle
Bertrand Perrochet
Teresa Sancristoval