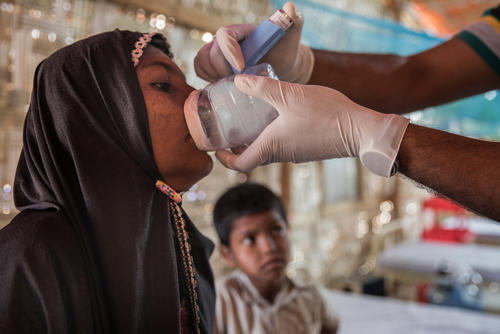
With the last major outbreak happening decades ago, most MSF staff had only ever seen diphtheria in textbooks. MSF medical team leader Carla Pla describes the challenges of treating the disease amongst the refugee settlements of southeastern Bangladesh.
“When diphtheria broke out in December in Bangladesh’s Cox’s Bazar district, the MSF team in Balukhali was completely overwhelmed. The district is sheltering almost 700,000 Rohingya refugees who have arrived over the last six months fleeing violence in Myanmar. It’s also where thousands of others who were there from previous crises are living in tents in huge, overcrowded makeshift settlements. This provides ideal conditions for the airborne disease to spread.
Some kilometres away from MSF’s clinic in Balukhali, we had started to build a brand new hospital in Moynarghona. Given the urgency of the situation, we decided to put the construction on hold and focus on setting up a diphtheria treatment centre in the hospital grounds. Initially housed in a series of tents, the treatment centre was later moved into several of the completed wards.
Patients with suspected diphtheria were soon being referred to us from across the area’s other health facilities. Imagine the scale of it: tens of thousands of refugees living in the nearby makeshift settlements, with many of the suspected cases being referred to us.
Learning on the go
In those early weeks, it was difficult to manage. Patients were arriving all at once, sometimes in minibuses, and at the same time our staff were not very experienced. We had never seen anything like this before – or only in textbooks – as the last outbreak of diphtheria happened decades ago [recently there has been also an outbreak in Yemen]. We had to learn around the clock how to treat patients for diphtheria.
The first thing, and I believe the most challenging one, is to ensure that patients are isolated to prevent the disease from spreading. The rules applied to everyone, including staff, which means they have to spend long periods wearing masks and protective equipment.
Diagnosis and treatment
When people with suspected diphtheria are brought in, most have a cough, fever and sore throat. Our staff do a clinical examination. Usually you see a thick membrane covering the throat, with white patches on the tonsils and a very swollen neck. Some patients experience bronchial spasms. The membrane can block the throat and constrict breathing. Diphtheria can also raise the heartbeat and cause neurological disorders that can lead to paralysis.
Once a diagnosis is confirmed, the most delicate part of the treatment is the administration of the diphtheria anti-toxin. The medication is given intravenously and can produce adverse reactions leading to complications, and even death, if not well managed. One-to-one patient-clinician care is necessary, particularly at the start, because you have to detect side effects quickly to be able to stop them.
Usually the patient is discharged within 48 hours of being admitted. But it doesn’t end there. Another key component is vaccinating and giving prophylaxis to all the people that the patient has been in contact with, to protect them against diphtheria and halt the spread of the disease.
Contact tracing
In the treatment centre, MSF staff identify all the patient’s contacts – those relatives or neighbours who have been in close contact with them in the past seven days. It can be very challenging to identify everyone. The next day, a contact tracing team goes to visit them and provide the vaccinations. Meanwhile, the team needs to check regularly on the discharged patient: to make sure they are taking the medication and not suffering side effects. After a month, the patient comes back to the centre for a final visit, when the medical staff confirm that there are no complications.
Diphtheria is a preventable disease, and the vaccine is part of the basic package of childhood vaccinations. Nevertheless, we have seen many children here affected with it, due to the refugees’ apparently very low immunisation status.
Death… and life
Some patients have died of diphtheria, which is very painful for everyone involved. We had a case of a child who came to us very late. The team worked very hard and were hopeful that he would improve. But then he died. I thought: ‘Why did he come so late? Why was he not vaccinated?’ You realise that this is how life is, and what we need is to make things change.
On a different day, another small child was brought in. She was tired, had no appetite due to the pain in her throat, and was very scared. She came from one of the makeshift settlements to a place where everyone was wearing a mask and speaking a language she didn’t understand. We played her a movie, we started her on treatment, and little by little she started to laugh. The next day I saw her as she was discharged. I remember thinking: ‘Well done everyone!’ This is the best part of our job.”
MSF has treated more than 4,280 people for diphtheria in the Cox’s Bazar district as of 31 January, most of them aged between five and 14 years. During the peak of the outbreak, MSF ran three dedicated health facilities. With cases decreasing over recent weeks, two of the facilities changed back to pediatrics, emergency room services ,and mother and child healthcare, while one diphtheria treatment centre remains open.