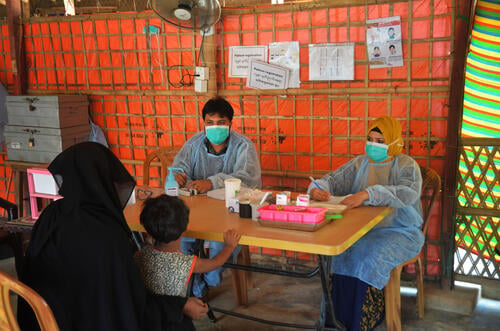
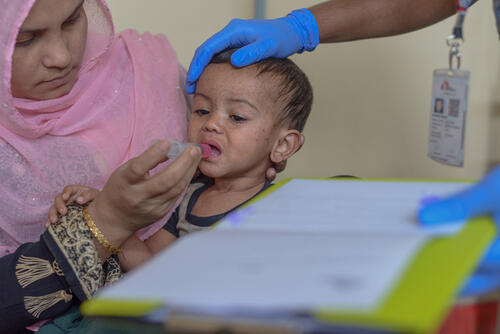
A loudspeaker from the mosque in Jamtoli comes to life at an unscheduled hour. Instead of the midday call to prayer, an imam asks his listeners to pay attention to their daily anxieties and seek help at the nearby MSF primary health centre.
“The community trusts me, I believe mental health programmes are needed for everyone’s peace of mind,” says Imam Sayeed Abdul Majeed (name changed on request).
Almost all Imam Majeed’s listeners are Rohingya refugees who fled targeted violence against them in Rakhine state, Myanmar in August 2017. Before escaping to safety in Bangladesh, many refugees directly experienced or witnessed significant violence and many lost immediate family members. In the camps, they live in cramped, overcrowded makeshift shelters, without enough food, clean water or toilets. Their lives are on hold, their futures uncertain.

“We are increasingly seeing new cases of generalised anxiety and depression,” says Pooja Iyer, MSF’s psychologist in the Jamtoli and Hakimpara health centres. While physical wounds may have healed, the memories of violence and loss of families through death or separation are still alive.
Two years on, mental health needs have evolved. Traumatic memories combined with unemployment, anxiety about the future, poor living conditions and little or no access to basic services such as formal education leave the Rohingya vulnerable to long-term psychological harm.
Gaps in mental healthcare
Nearly 450 patients seek mental health counselling in the Jamtoli and Hakimpara health facilities alone. The prevalence of chronic psychosis – a severe mental disorder that requires psychotropic treatment – is high among MSF patients. When 17-year-old Rohingya twins Abdul Hasim and Abdul Halim first came to the Jamtoli health centre, they behaved like children and were disconnected from reality. Disorganised thinking, seeing or hearing things that are not present, and behaviour like that exhibited by the twins are typical signs of psychosis.
Many MSF patients complain of nightmares and flashbacks. Aggressiveness, suicidal tendencies, delusions, and substance addiction are also common. MSF psychologists say they are symptoms of trauma and unresolved grief. Many patients have bipolar disorder, schizophrenia or other psychoses, and psychological difficulties linked to epilepsy.
At the beginning of the 2017 influx, psychosocial support was key to helping survivors cope with the trauma of suffering extreme violence. Today, psychiatric care, combined with psychosocial support, is essential to alleviating the mental health conditions prevalent in the camp. It remains an unaddressed gap. Increasing long-term comprehensive mental health services implies additional resources and personnel to evaluate the true extent of mental health issues. The health response needs trained psychiatrists who can diagnose and prescribe medicines to treat severe mental disorders.
Another gap is services for children with developmental, neurological or learning disabilities or delays.
“We have patients with cerebral palsy, attention hyperactivity deficit and autism-spectrum disorders who cannot go to a regular school or a learning centre, as they get teased and bullied,” says Iyer. “They suffer in silence.”
MSF health facilities across the Cox’s Bazar district, which covers 2,492 square kilometres, aim to support local health structures in addressing increased patient needs. While the majority of MSF’s patients are Rohingya, comprehensive mental healthcare services are also available for Bangladeshis.

Enduring social stigma
Among both communities, mental health remains poorly understood. Most patients at MSF’s health facilities exhibit visible signs of psychological stress and trauma. Many others suffer from depression, post-traumatic stress disorder, schizophrenia and psychosis, which go virtually unnoticed by their community.
Patients with visible signs of psychological distress are said to be possessed or under the influence of black magic. The Rohingya community, excluded from healthcare for decades in Myanmar, often resort to traditional healers due to either cultural affinity and beliefs, or lack of trust in healthcare providers in the camp.
We need to pay attention to the intergenerational consequence of this crisisTanya Morshed, MSF psychotherapist and clinical social worker
“Many patients are referred to mental health counsellors only when they come to seek medical treatment for physical ailments in our health facilities,” says Tanya Morshed, an MSF psychotherapist and clinical social worker. She is responsible for strengthening mental health awareness activities among the communities in Kutupalong and Balukhali camps.
“Psychiatric patients who display aggressive behaviour are often chained due to fears and misconceptions around mental illnesses. Neglect of basic needs of food and cleanliness, and isolation can result in further deterioration of their condition,” says Morshed. “Those without visible signs endure.”
The most vulnerable, according to Morshed, are those who suffered sexual violence, either in Myanmar or in the refugee camps in Cox’s Bazar. For MSF, sexual violence is an emergency that requires immediate medical attention. Stigma around it, nested in patriarchal attitudes, increases the risk of long-term psychological damage. Morshed says children born from rape are often abandoned and are shamed by their own community.
“We need to pay attention to the intergenerational consequence of this crisis,” says Morshed.
Building trust
Patients’ isolation and loneliness is another challenge for MSF’s mental health teams. Their inability to contact their families in Cox’s Bazar or Myanmar due to restrictions on movement or telecommunications can worsen existing conditions.

MSF teams tackle the stigma and isolation faced by patients by building trust and solidarity through psychoeducation activities. Community mental health educators (CMHEs) with similar religious and cultural affinities are key in building trust and awareness of mental healthcare among patients, caregivers and community leaders.
Patients and families often abandon mental health treatment, as counselling and medication can take time to take effect. CMHEs help ensure patients continue medication and follow up on psychosocial sessions. Mental health teams, composed of CMHEs, counsellors, psychologist supervisor and psychiatrists ensure each patient has a specialised treatment plan.
The loudspeaker at the Jamtoli mosque crackles again. Imam Majeed repeats his message, optimistic that people will follow his advice. Patients, caregivers, community leaders and MSF teams are together in ensuring trauma and deprivation does not come to define the lives of those seeking mental healthcare in Cox’s Bazar. But is there hope?
“Most of my young patients are scared of men in uniform, as they witnessed violence perpetrated by either the Myanmar army or police,” says Iyer. “When the children improve, they are able to recount their experiences without trembling or urinating in their clothes. Isn’t that hope?”