Niger is a vast, arid state on the edge of the Sahara. It is rated by the UN as one of the world's least developed nations, with one of the highest rates of population growth.
Niger shares a border region in the Central Sahel with Burkina Faso and Mali. Here, state and non-state armed groups operate in a context of poverty, climatic variability, and increasing competition over dwindling resources.
The southeast of Niger forms part of the Lake Chad Basin, where violence that began in Nigeria in 2009 has spread.
Niger is also a major transit country for migrants, asylum seekers and refugees expelled from Algeria, returning from Libya or travelling north to Europe. It hosts the majority of Malian, Nigerian and Burkinabe refugees.
Already vulnerable to drought and food shortages, especially during the 'hunger gap' between harvests, usually between May and September, people in Niger continue to suffer the consequences of crime and violent clashes between armed opposition groups and military forces in the region.

Abandoned in Niger
Violence in Mali and Burkina Faso has spread across the borders into the Tillabéri and Tahoua areas of Niger, where more than 155,500 people are internally displaced. Armed groups regularly clash with the national military, and intercommunal tensions and criminality are increasing.
In the southwestern region of Tillabéri, reported attacks against security forces, traditional leaders, schools, people working in education, and health centres are escalating.
In southeast Niger, the security situation in the Diffa region remains tense, with attacks by armed groups targeting both civilians and military positions.
For the past 20 years, we have been working in Niger mainly to address recurrent epidemics (cholera, meningitis, measles and malaria) and regular acute malnutrition emergencies. We also provide healthcare to victims of violence in displacement and conflict settings (Diffa, Tillaberi) and assistance to people travelling along migration routes in Agadez. In 2020, we helped with the country’s COVID-19 response.

Assisting migrants in Agadez
In Agadez, in the north of the country, we support local communities and migrants along the main migratory routes. In Assamaka, we provide medical and humanitarian assistance to people who have been expelled from Algeria.
At health facilities in Arlit, Séguédine, Anaye and Tabelot, our teams provide general health services and infant and maternal care, and run mobile clinics at transit sites. In these areas, networks of community relays provide epidemiological surveillance and inform people on health and protection issues.
Responding to the needs of displaced people in Tillabéri
MSF first began work in Tillabéri in November 2018 following increased violence in Liptako-Gourma –
an area that borders Niger, Burkina Faso and Mali.
This situation has resulted a significant rise in internally displaced people in the region and has affected people's access to basic social services. The health system in the region is failing with many health centres not functioning properly and lacking qualified personnel, many of whom have deserted due to the crisis.
In this context, our teams provides regular medical and humanitarian assistance. We support numerous health centres and provide basic and specialised healthcare in two camps for host communities and displaced people in Banibangou, Ayerou, and Torodi districts.
When the security situation allows, our teams also organise mobile and emergency activities to provide medical and mental health consultations, and distribute essential household items, including mosquito nets and buckets, to newly displaced people.
Malnourished children are identified and tested before being referred to nutrition centres. Our teams have also conducted immunisations and health promotion activities in the region.
Activities in Diffa region
Our teams support the regional maternal and child health centre in Diffa and the district hospital in Nguigmi by providing paediatric, neonatal, nutrition, maternity and obstetric emergency services. We also run mobile clinics and community activities in rural areas and carry out emergency interventions to help people affected by violence. We run a mental health and psychosocial support programme for children and adolescents in Diffa to address the psychological and social repercussions of traumatic events they have experienced.
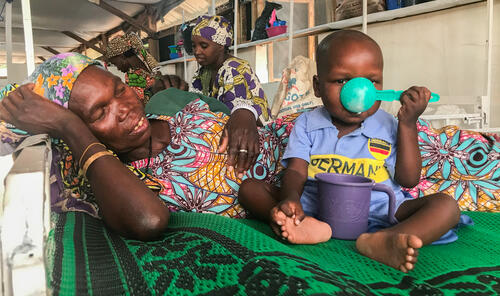
Seasonal emergency: malnutrition and malaria
Every year, the combination of food insecurity and the rainy season triggers a spike in rates of malnutrition and malaria in southern Niger – particularly from June to November.
Each year, around one million children are affected by acute malnutrition, and around 50,000 of them die.
From June to September, our teams double their response capacity in Madarounfa (Maradi region) and Magaria (Zinder region) to respond to the combined malaria and malnutrition annual peak affecting children under the age of five. Since 2005, MSF has worked with the Ministry of Public Health to offer children the best possible treatments for malaria and malnutrition.
Our teams are also responding to the increased malaria and malnutrition cases in the capital, Niamey. In 2020 and 2021, we deployed emergency teams in the Regional Hospital Centre to treat paediatric cases up to 14 years old. Between August and October 2021, our teams admitted more than 2,600 patients – around 1,550 were below five years old. We are also supporting three other health centres in Niamey, providing free admissions and care to children under 14 years old.
In Tahoua, our teams began interventions in the health district of Madaoua in November 2021, with a three-week mass screening campaign for malaria for children aged two months to 15 years. This was coupled with nutritional screening of children aged between six and 59 months.
A total of 181,122 children were screened with the rapid malaria tests and 106,122 children were treated for the disease.



