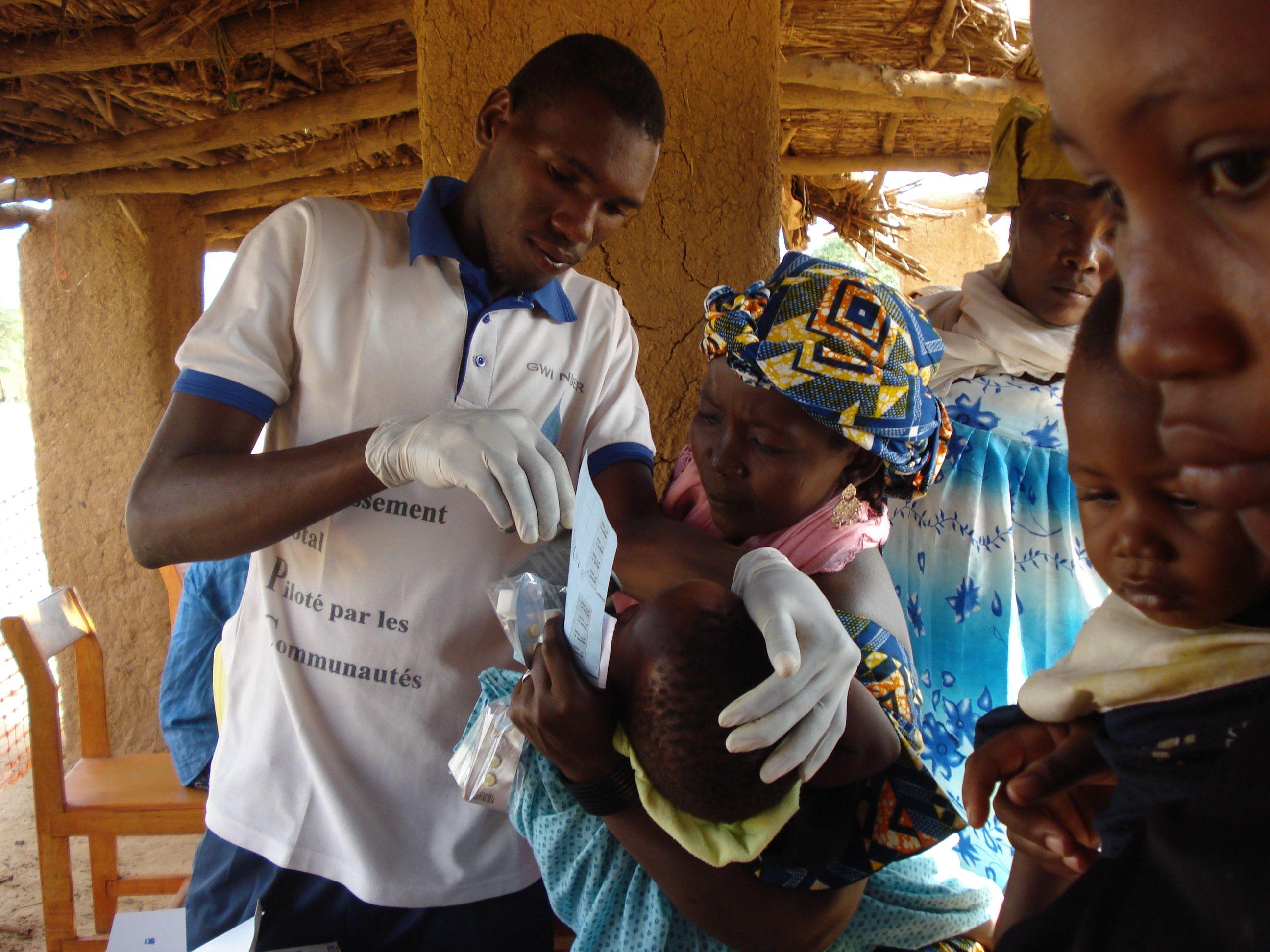
In the weeks before the rainy season begins, teams from Médecins Sans Frontières (MSF) in Niger have been working hard to distribute medicine that will prevent malaria, while preparing themselves to deal with possible food crises in some areas of the country.
Each year, the arrival of the rainy season in Niger brings with it a real risk of catching malaria from the mosquitoes which breed in stagnant water. Malaria can be fatal, so to help prevent people from contracting the disease, MSF teams have just completed an initial round of seasonal malaria chemoprevention (SMC), a new preventive method recommended by the World Health Organization (WHO) since last year.
This is the first time that SMC has been used in Niger. The treatment, introduced by MSF teams working alongside the Ministry of Health, is aimed at children aged between three months and five years, who receive three doses per month over the four months of the rainy season. So far, more than 184,000 children from more than 1,000 villages in the districts of Magaria, Guidan Sori, Moulé, Tafo, Sabon Guida, Bouza and Madaoua have received initial doses of the medicine.
The campaign to protect young children from malaria has seen more than 1,850 local community agents together with international teams visiting villages across the area, raising awareness about the campaign among local people, distributing the medicine and encouraging parents to make sure their children receive the full 12 doses.
More than 600,000 people die each year from malaria. However, recent estimates from the WHO suggest that, over the past decade, cases have dropped by 25 percent, meaning that more than a million deaths have been prevented, the vast majority of them among under-fives in sub-Saharan Africa. Improved access to rapid diagnostic tests and artemisinin-based combination therapies (ACT) have revolutionised malaria treatment in developing countries. SMC is a new approach.
In 2012, a programme initiated by MSF in Mali and Chad saw more than 200,000 healthy children receiving SMC, with very encouraging results. There was a 66% reduction of cases of simple malaria, with 70% fewer hospital admissions and 75% fewer blood transfusions due to malaria during the campaign in the Koutiala district in Mali.
Despite the encouraging results, “SMC is not a miracle cure,” warns Anja Wolz, MSF’s medical coordinator in Niger. “It allows us to reduce the mortality rate and the number of cases of malaria in countries where there is limited access to care. But the top priority is to continue to increase the provision of mosquito nets and insecticidal spray, as well as diagnosing and treating cases of malaria.”
In addition, SMC is only relevant in regions where malaria is seasonal, rather than endemic, as distributing the treatment all year round would be a near-impossible task.
A fatal combination
But SMC is expected to play an important role in preventing malaria in Niger, says Wolz. “Preventing malaria with this new treatment is vital for children under five,” she says. “Each year in Niger, at this time, children in particular face not just malaria but also food crises. And malaria combined with malnutrition is a fatal combination.”
The ‘transitional period’ of the rainy season is a time when household food stocks run low even before the next harvest has been planted. It is a critical time for the poorest households in these regions: food supplies run out just when prices peak in the markets. And the rainy season multiplies the number of mosquitoes responsible for spreading malaria.
Malnutrition and malaria are the two main illnesses that affect under-fives during this season. Without access to the micronutrient-rich food they need, many suffer from malnutrition. Undernourished children have less immunity to illnesses generally, and so are more susceptible to contracting malaria with complications. Malaria also weakens the metabolism and leads to loss of appetite in young children. The combination of malnutrition and malaria can be fatal.
In parallel with the SMC campaign, MSF teams have systematically checked some 128,000 children aged between 6 and 59 months for malnutrition, treating those who are severely malnourished; they hope that this will prevent children coming for medical care only when they are suffering from complications and it is too late for them to be saved.
The MSF teams are being kept on their toes. They are getting ready to respond to the medical demands of this critical period while at the same time putting in place measures to prevent a sharp rise in malaria and minimise the number of children who need to be admitted to hospital.
Extensive malnutrition in some regions in Niger
This year, children have suffered exceptionally high levels of malnutrition in some regions in Niger, mainly in the Maradi region. At Madarounfa, MSF has been caring for nearly twice as many malnourished children in 2013 as in the same period in 2012 (5,455 compared to 3,985).
Dr Chantal Gamba, who runs MSF’s programmes in Niger, says that many of these children are suffering from marasmus (a severe form of malnutrition without oedema) as well as dehydration or severe malaria. “Given this increase in our activities, MSF has had to change the way it works: we have organised more hospital space to accept more children and we have provided the human and material resources to assure the extra care.”
Figures from the Niger authorities show that Maradi is the only region of Niger affected by pockets of malnutrition and – in some welcome news – that overall in Niger the nutritional condition of under-fives has improved slightly in 2013. The data shows that acute malnutrition is at 13.3% nationally, with severe acute cases at 2.6%. This means that 376,000 children are suffering from malnutrition, 77,000 of them from the severest form of the disease.
MSF’s work in Niger is mainly aimed at improving healthcare for children under five and pregnant women, focusing on prevention and early treatment of malnutrition in particular. In the regions of Zinder, Maradi and Tahoua, MSF teams run outpatient feeding programmes in some 38 health centres, while patients in need of hospital care are admitted to inpatient feeding centres in Zinder, Magaria, Madarounfa, Guidan Roumdji, Madoua and Bouza hospitals. Since the spring of 2012 MSF has also been providing basic and hospital-level healthcare in Abala camp, in Tillabéri region, which houses refugees from Mali. MSF has been working in Niger since 1985.