“When COVID-19 reached Iraq in March 2020, it was quickly clear that it would be a huge challenge to the health system,” says Dr Daniel Uche, Médecins Sans Frontières (MSF) emergency medical team leader in Baghdad. “Numbers started increasing rapidly and healthcare workers were soon overwhelmed.”
Our teams had already been working extensively in Iraq, where the healthcare system was struggling to meet the needs of Iraqis after decades of war and instability. So when the pandemic hit we had to react quickly in order to support those in need of care. Nearly two years after the beginning of the pandemic, Al-Shifaa Hospital at Baghdad Medical City is the latest in a line of hospitals that we have collaborated with.
Baghdad has been the city hardest hit by COVID-19, and so it is here that we have focused our efforts. We provided essential training on infection prevention and control measures, and on triage management, as well as mental health support to help COVID-19 patients and caretakers cope with the impact of the disease.
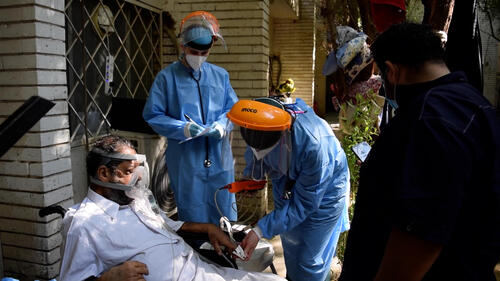
With admissions in the intensive care units increasing at a fast pace, hospitals were overwhelmed by the number of severe cases. Our teams extended support to include directly caring for patients in the intensive care unit of Al-Kindi Hospital.
From September 2020 until October 2021, we worked there in close collaboration with the hospital’s management and healthcare providers to provide lifesaving care, physiotherapy, and mental healthcare to severely and critically ill COVID-19 patients.
We started with a ward of 24 beds that was later expanded to 36 and then to 52 beds, as the numbers kept increasing with each wave. In total, our teams cared for 934 critically ill COVID-19 patients at Al-Kindi Hospital and reduced the average mortality for severe cases by 40 per cent.
During the peaks, we often saw some patients who were in dire need of intensive care but unable to access it, because intensive care beds were full everywhere.Dr Daniel Uche, MSF emergency medical team leader
“During the peaks, we often saw some patients in dire need of intensive care, but unable to access it, because intensive care beds were full everywhere,” says Dr Uche. “Healthcare providers had to put in extra work to care for the large influxes of sick people and they were exhausted.”
To increase bed capacity, healthcare authorities were sometimes left with no option but to switch other healthcare facilities into COVID-19 treatment centres.
“As a result of that, regular healthcare services had to be disrupted in many facilities across the city, which in turn impacted other patients with other health conditions,” says Dr Uche.
The country has experienced three waves of the disease, each bigger than the last. But the challenges have remained constant.
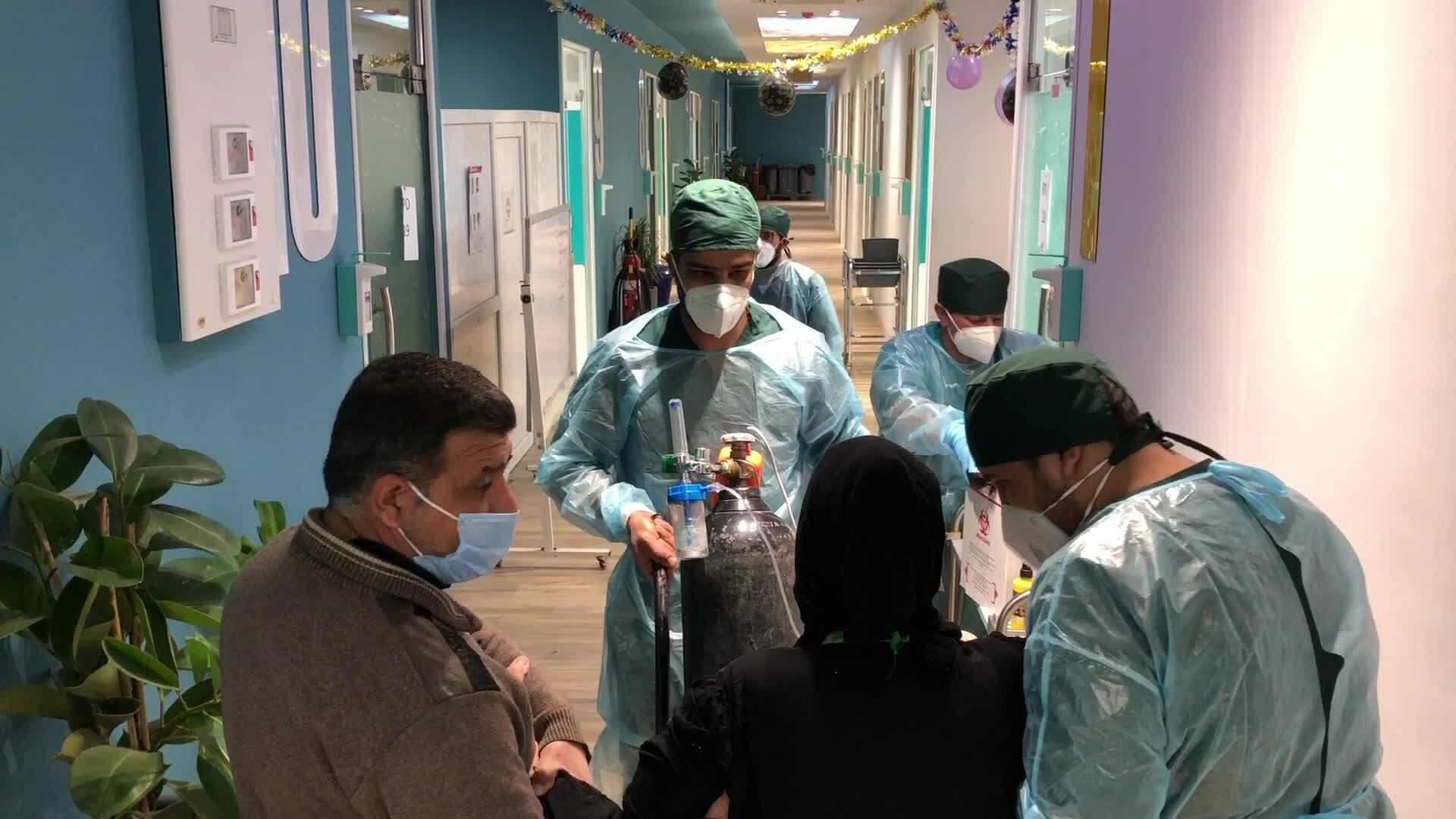
COVID-19 in Baghdad
“One of the big problems we often faced was that most patients admitted to the intensive care unit came to us at a very late stage and already in critical condition,” says Dr Uche. “They tried everything they could at home and only came when they couldn’t avoid it anymore. So, we were treating the complications of late arrivals on top of the COVID-19 infection itself.”
The numbers of COVID-19 infections in Iraq have started to increase recently, and with just around 15 per cent of people fully vaccinated and poor compliance with infection prevention measures, in addition to the recent arrival of the rapidly spreading Omicron variant of the virus, Iraq is not safe from the effects of another wave.
The country also has high numbers of people with chronic diseases that are considered risk factors for a severe COVID-19 illness, such as hypertension, diabetes, and lung disease. All these factors mean that the preparedness of the health system is key to responding effectively to any increase of hospitalisation rates and that’s where we have been supporting Baghdad Medical City’s Al-Shifaa Hospital.
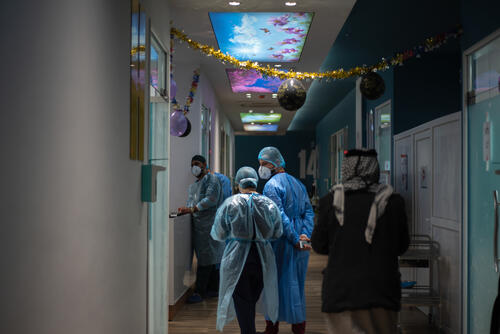
Preparing for a new wave
When the last wave of COVID-19 was declared over in Iraq, our COVID-19 team moved activities to the Baghdad Medical City to continue the support and preparedness for any future increase in infections.
“At Medical City, we are currently simultaneously caring for severe or critical COVID-19 patients in the intensive care unit and raising the levels of preparedness of healthcare workers by providing training and on the job coaching,” says Dr Uche. “We hope that we don’t see a surge in the number of cases, but at the same time we are doing our best to be ready if that happens.
Elsewhere in Iraq, our teams also run a six-bed patient isolation and treatment unit for mild to moderate COVID-19 patients at the Sinuni General Hospital in Sinjar. We support the Tel Afar General Hospital with essential infection prevention and control training, and preparedness to care for severe and critical COVID-19 patients if numbers start increasing.
MSF has also supported healthcare facilities in responding to the pandemic in Ninewa, Erbil, Kirkuk, and Duhok governorates, mainly through providing essential training and supplies to strengthen infection prevention and control measures in hospitals. Between March and December 2020, we temporarily transformed our 62-bed surgical hospital in East Mosul to become an isolation and treatment centre for suspected and mild to moderate COVID-19 patients. Between November 2020 and April 2021, we ran a COVID-19 intensive care unit at Al-Salam Hospital in East Mosul.






