934,400
934,4
313,500
313,5
55,400
55,4

47,700
47,7
25,100
25,1
14,300
14,3

1,000
1,
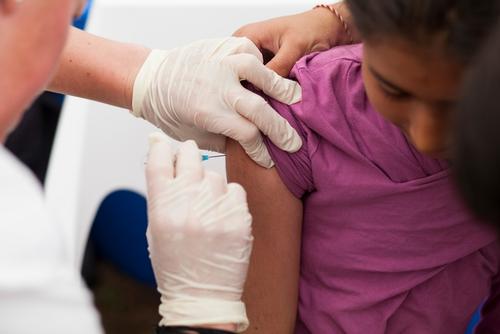
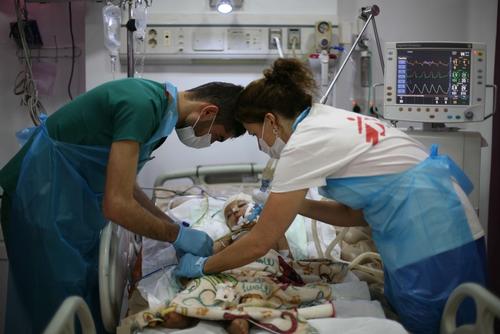
Hundreds of thousands have been unable to access basic necessities such as food, water and primary and secondary healthcare for months at a time, and live in fear for their lives.
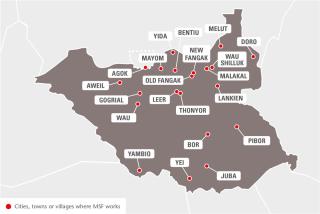
In 2016, MSF continued to respond to the urgent medical needs of people affected by violence and maintained its essential healthcare programmes across South Sudan, despite the growing challenges we face reaching those in greatest need. As insecurity and violence spread across the country, providing humanitarian assistance has become increasingly complex and, in some places, increasingly dangerous.

Juba
After fighting broke out in the capital, Juba, in July, MSF set up a surgical facility and ran mobile clinics across the city. In the first month, one outreach team treated 9,242 people for violence-related injuries and health problems caused by the deteriorating living conditions.
MSF staff also helped the Ministry of Health to set up and run a cholera treatment centre in Juba teaching hospital.
Greater Upper Nile Region
Pibor
The MSF clinic in Pibor provides inpatient and outpatient care, including maternity and emergency services. Looting in February temporarily halted activities, but the clinic was fully operational again by April. The team started to offer surgery towards the end of the year.
Doro
MSF staff continue to offer medical care to the 50,000 Sudanese refugees in Doro camp, as well as the local community in Maban county. Mobile clinics deployed during a spike in malaria tested 9,970 people for the disease.
Lankien
The MSF hospital in Lankien is the only functioning medical facility in the area. Although malnutrition rates were lower than expected this year, the team still admitted 1,068 patients to the therapeutic feeding programme. Malaria is the main illness treated at the Lankien hospital and the primary healthcare centre in Yuai. In 2016, teams at the hospital in Lankien also provided treatment to 1,530 patients for kala azar (visceral leishmaniasis), a potentially fatal disease spread by sandflies. A total of 116,944 outpatient consultations were carried out in 2016 at Lankien hospital and the Yuai healthcare centre.
Bor
MSF continued to train staff and rehabilitate buildings at Bor state hospital. From April, the team supported surgery and worked to improve the pharmacy, sterilisation and waste management.
Fangak
In 2016, MSF refocused its presence to provide access to healthcare in the war-torn Fangak area, progressively handing over its outpatient activities in Old Fangak, and starting activities in New Fangak, where only a few other humanitarian organisations are present. In Old Fangak, MSF supported a 40-bed hospital, where 66,000 outpatient consultations were provided and 1,800 patients were admitted.
Bentiu protection of civilians (PoC) site and town
Insecurity led many more civilians to seek refuge at the PoC site in Bentiu. MSF remains concerned about the consequences of the sub-standard conditions on the health of the 120,000 people living there. MSF runs the only hospital on the site, a 160-bed facility with an emergency room, operating theatre and maternity unit. Treatment is also available for sexual and gender-based violence, HIV, tuberculosis (TB), cholera, malaria and kala azar. In addition, teams run health promotion, monitoring and outreach activities across the site and in Bentiu town. In 2016, MSF conducted 40,380 primary healthcare consultations and admitted 4,325 patients.
Leer and Mayendit counties
In early 2016, MSF set up emergency services in Leer and Mayendit counties as intense fighting displaced thousands of people, mostly into nearby swamps. The area remains a conflict zone, and the humanitarian needs are immense. Mobile teams provide basic healthcare, focusing on malaria, respiratory tract infections, diarrhoeal diseases, nutritional support, vaccinations, and treatment for victims of sexual violence. In July, medical activities were temporarily disrupted when the MSF compound in Leer town was looted.
In Yida, MSF offers a broad range of inpatient and outpatient services, including vaccinations, and HIV and TB treatment, to refugees from South Kordofan, Sudan.
In Mayom county, MSF runs a clinic with the Ministry of Health offering basic emergency healthcare, as well as treatment for HIV and TB.
In February, the MSF-run hospital in Malakal PoC site was attacked, and over 25 people were killed, including two staff members. MSF published a report on the events and launched an international advocacy campaign calling on the United Nations Mission in South Sudan to provide credible security to civilians under its care and improve the conditions in the PoC. In June, a new 60-bed hospital was completed on the site to replace the existing structure, and MSF also opened a medical centre in Malakal town with an outpatient and inpatient departments and a delivery room to cater for the growing population.
On the opposite bank of the White Nile, Wau Shilluk hospital continues to provide primary and secondary healthcare for displaced people who have settled in the area.

Equatoria Region
Yei
Following an increase in violence in Equatoria region, MSF set up a clinic to provide healthcare and mental health support, as well as vaccinations. From November, mobile teams were deployed, and treated 1,368 patients in the first week.
In November, a project set up in response to fighting around Mundri had to be suspended after an armed robbery.
Despite sporadic clashes in the Yambio area, MSF continued its HIV ‘test and treat’ programme, which focuses on providing antiretroviral treatment to patients as soon as they are diagnosed.
Bahr El Ghazal region
Aweil hospital, the only secondary healthcare facility in the area, serves 1.5 million people. In 2016, the team provided maternal and child healthcare and responded to a sharp increase in malaria cases.
Further South, in Wau, MSF carried out around 42,000 consultations when violent clashes displaced over 60,000 people in June.
Agok, Abyei Special Administrative Area
Agok hospital provides specialist and emergency care to over 140,000 people in remote Abyei. In 2016, teams carried out around 50,000 consultations and 1,600 surgical interventions. In addition, MSF’s malaria programme treated over 40,000 patients in isolated villages.
Project closures
At the end of 2016, the team started to wind down operations in the medical facility in Melut as other organisations had stepped in to provide healthcare. In Gogrial, where MSF started working in 2009, most medical activities were handed over to the Ministry of Health in May.