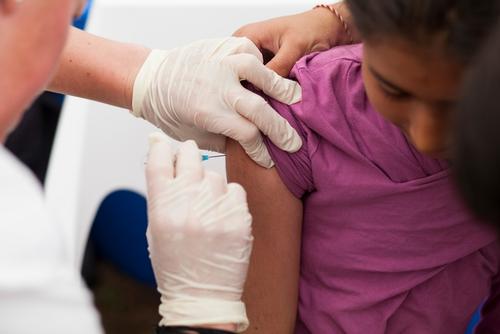
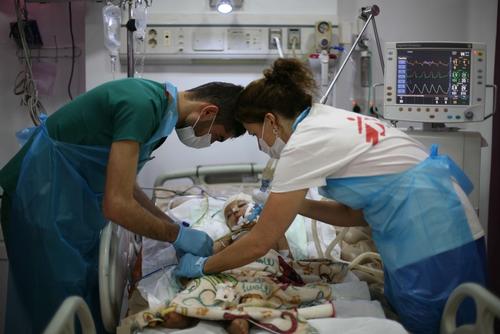
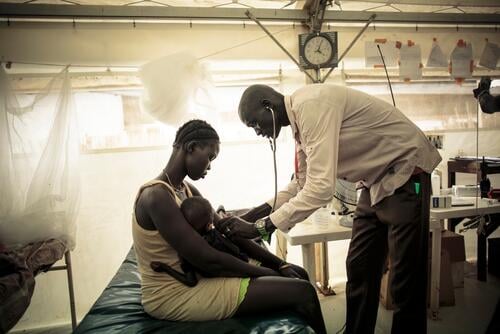
Anastasia
(30) from Minsk was diagnosed with multidrug-resistant tuberculosis in November 2015.
“To learn that you are sick – it’s a shock. You don’t feel anything, it doesn’t hurt. But then you are scared: what will they say at work? I quit my job, spent three months in hospital. I felt bad because of the medicines: I was nauseous, my stomach hardly worked, I had no strength to get up, I was dizzy, I had pain in my joints. You have to take your drugs daily under medical supervision, because no sane person can bring himself to swallow the stuff that produces such severe side effects. And it’s every day, not just for a week, a month or even a year, but for 18-20 months ... MSF were there for me. Many thanks for their invaluable support. How many times have I seen the joy in the eyes of patients coming from the counsellor's office!”
Belarus
Farah*
26, mother and shopkeeper
I gave birth at the Gbaya Dombia maternity hospital on the afternoon of 30 October 2016.
The birth went very well, and afterwards I was transferred to a recovery room. I was there with my friends and family when I heard gunfire, and then I heard banging at the gate of the hospital. It was then that the wounded started to arrive. There were a lot of people and they were everywhere. There were wounded in all the beds except mine.
In this neighbourhood [PK5] insecurity is constant. We regularly hear gunshots and every two or three days there’s a fight. People argue and then pull out a weapon. Weapons are everywhere. Even honest, hardworking people carry weapons to protect themselves.
* Name has been changed
Central African Republic
Elysée
18, from Ngola, South Kivu, DRC
We often have to flee clashes between the armed groups and the regular army. That’s why we can’t tend our fields. When we’re able to return, either the crops have spoiled or they’ve destroyed or burnt them all. Life is difficult in Ngola and it’s tough to find food in the forest. My three children and I received some food only once from an NGO and now my children have been treated at the Makala health centre for free. I thought I was going to lose one of them to malaria. The distribution of soap, blankets, fabric (for the women to carry children, swaddle babies and use as clothing), mosquito nets and farming tools will help us, as we have nothing ─ we have lost it all. We need everything.
Ngola, in Lulingu, is quite isolated. Only MSF was able to distribute the non-food items. They used 30 motorcycles in an operation that took more than a week.
Democratic Republic of Congo

Conor Kenny
Doctor
They escape only to be confronted with a new challenge here at Idomeni. The camp in the north of Greece on the border with the Former Yugoslav Republic of Macedonia has formed around an international freight train station for goods and a cattle slaughterhouse. Accommodating over 10,000 refugees and migrants, these people live in constant fear. Fear of the unknown. Fear of receiving the worst news from home - will the next bomb in Syria kill somebody they love? The genuine fear of being sent back.
The distress and frustration here is palpable. For Hamza, we had to prescribe relaxants. An extreme response - used as a last resort. But in this case, he was causing himself serious physical harm and with many women and young children inside, we had no other option. We kept him in the clinic for observation and spent time listening to his story before referring him to one of our psychologists.
I hope he will do well. But to be honest, I don’t know what will happen to him as time goes on. Nobody knows what will happen to him, or indeed anyone stuck Idomeni. It seems they are trapped in no-man’s land. As one patient told me, “We are dying here, just like we were in Syria, but slower”.
Greece

Salematou Camara
61, Ebola survivor in Guinea
“When I returned home after leaving the Ebola treatment centre, only my sons and daughters approached me; all the other people were too scared to. Now the situation is much better but I’m still affected by cataracts and because all eye surgery on Ebola survivors is forbidden, I cannot be operated upon.”
Guinea

Doctor Mohammad El-Momani
Emergency room doctor at MSF Ramtha surgical project, Jordan
In June 2015, I joined MSF in Ramtha district as an emergency room doctor and a supervising doctor for the inpatient department responsible for receiving emergency cases from Syria. All those cases were critical war injuries caused by missiles, explosive barrels, mines or bullets.
Since the decision to close the northern borders of Jordan, we no longer hear the sirens of the ambulances carrying the wounded and injured from the Syrian war to our emergency room. This unfortunate situation means that the injured Syrians will have to remain on the Syrian side of the borders, losing their only chance of survival and the right to receive medical care as well as physical, psychological rehabilitation.
One of the patients I received in the emergency department who touched the medical team on duty and me on a personal level was a woman who said she was hit by a rocket-propelled grenade. She was eight months pregnant at the time and, as a result of the grenade, her two legs were amputated. What caught my attention and shocked me the most was the strength and control this lady had: she understood and accepted her bitter reality and was able to endure and tolerate her situation.
Jordan
Fanta Meleram
30, fled northern Nigeria when her village was attacked and found refuge in Diffa region.
“I took my son to the health centre today because he is malnourished. I have just visited so that he can receive his treatment, a therapeutic food. This health centre is wonderful because when we come with our children or when we are ill ourselves, we are looked after for free. When Boko Haram attacked, we left Malanfatori in a rush and in a total panic. Some of our children succeeded in fleeing with us, but others were left behind and some women lost their husbands during the escape. They pursued us until we succeeded in crossing the Komadougou river to come to Niger. We arrived empty-handed and our husbands are not working. It is difficult to find food and it is very difficult to live in these conditions. Sometimes the state gives us help, and that is a relief.”
Niger
Ruslan Ozdoyev
32-year-old
In June 2014, 32-year-old Ruslan Ozdoyev became MSF’s first XDR-TB patient in Chechnya to start a new treatment regimen containing bedaquiline. Within two months of treatment, he tested negative for TB. On 15 July 2016, Ruslan was declared cured.
“I was admitted to the hospital with the most complicated diagnosis of TB. I weighed 75kg before the disease. After I fell ill, my weight dropped to 40kg. I was taking drugs, but there was no improvement. In July 2014, they started me on a new treatment. In the beginning it was very tough. I was nauseous and vomited, but began to get better after some time. My weight went up to 70kg. I want to thank everyone who took care of me. Now this is the treatment that really works.”
Russian Federation
![Sinethemba- MSF Treatment For TB in South Africa. Sinethemba in the streets outside the home she shares with her grandmother and four other family members, Zone C29, Khayelitsha, Western Cape.
Sinethemba, 16 years, lives with her grandmother, Vuyisiwa Madubela, and four other family members in a two-bedroomed home in Zone C29, Khayelitsha, Western Cape, South Africa.
Her grandmother’s determination and love, combined with receiving a six-month trial of one the newest DR-TB drugs on the market likely saved her life this year.
Current regimen: delamanid, linezolid, pyrazinamide, ethambutol, clofazimine, high dose levofloxacin, terizidone.
Grandmother Vuyisiwa Madubela:
“Sinethemba’s mother died when she was 6 months old, she was taken [raised] by my elder daughter who also died last December.
She’s from PE (Port Elizabeth) and when I arrived there for the funeral I saw Sinethemba was very sick – thin, weak, shaking, very pale, sleeping, very high temperature . She was very quiet. I hadn’t seen her for a long time, nearly three years.
On the day of the funeral, the senior sister in the area called me – “Can you take her? This child is sick… “
I thought I was going to lose her. It was painful as I’ve lost three children. I used say ‘if I lose one child, I’ll die; I was thinking: I’ve lost her mum, and she’s going to die too.’
During her first month with us in Khayelitsha, it was terrible - she wouldn’t eat. We’d all just watch her. Everyone was sad. When I wanted to cry, I had to go outside.
On 12 December 2015, she had X-rays, and they took sputum. They called and said I had to come immediately, she had MDR-TB and they were putting her in Brooklyn Chest Hospital.
That day, I lost hope. I thought she was going to die. If she stayed in PE, she would have died.
By end December 2015 she started MDR treatment with kanamycin injections, as well as the other drugs – they said she could go deaf because of the side effects of the injection. She had to go to the clinic Monday to Friday, every day.
It was painful and some days she asked not to go. In February 2016, her sputum showed that she was resistant to the injection, so they applied for new drugs to change her treatment.
In February 2016, MSF came and explained that they could apply for a new drug for Sinethemba called delamanid if I gave my permission for her to take part, because the drug is not usually available for TB patients in South Africa. We met with a counsellor, and got a lot of information.
The first few days she had nausea, wanting to vomit. I sat her down and I said: “You have to accept this; you must talk to your tablets. You must give them an order: ‘I am in charge.’”
Not even a month later, she started speaking, even dancing. She’s going to church, she’s singing in the church choir. Everyone could see there was an improvement and they wanted to know what happened. She’s going for an electrocardiogram (ECG) every month and it’s normal.
Last year was very hard for the whole family, but from February when she started delamanid, she didn’t take a long time to get better.
The only problem is now she eats everything. We have to dish up twice! She’s gained weight.
When she went for her last x-ray they told me they don’t see any signs of TB in her chest.
Sinethemba hasn’t been to school this year, I was told that she wouldn’t cope, that the treatment would make her drowsy, sleepy. We’ve been told she can go next year.
Everyone could see there was improvement. Everyone wanted to know.
What would I like to tell the manufacturer of delamanid?
I would ask the manufacturer of delamanid to give it to every patient who really needs it. I see lots of TB patients at the TB clinic. If people got this drug, they could really control DR-TB. TB is a giant but not a killer. TB can be cured.”](https://img.msf.org/AssetLink/f31lbo56u8u05c8imar6urfc86637n67.jpg)
Sinethemba Kuse
17, from Khayelitsha, was one of the first multidrug-resistant TB patients initiated on delamanid in South Africa.
“Just imagine being told that you have MDR-TB just before Christmas. The same day the doctor gave me tablets and I also got an injection. The injections were painful. I was scared of the needle because I had to be injected every day. Sometimes I would bleed and I even got lumps. I swallowed a lot of tablets, so I would vomit or be dizzy. Later, we were told about a new medication that is available in Khayelitsha that not a lot of people are lucky enough to have. Dr Jenny [Hughes] of MSF explained more about this new drug called delamanid. In February 2015, I started taking it. All I can say is that there is hope. I trusted it with my life and it worked. My gran and everybody started noticing the difference – even my gran’s church friends saw the change.”
South Africa
Maggi Myeni,
50, an HIV patient from Tibane in Shiselweni.
I collect my drugs from JCI clinic. It takes me around five hours to travel to and from my clinic and I spend SZL 60 for the trip. In May 2016, a small group of neighbours on HIV treatment and I formed a community antiretroviral treatment group (CAG). Each month, the group chooses one member who goes to the clinic to collect the medication for the others.
I find being in the group very helpful and I am able to save the little money that I have. Today, it was my turn to come to the clinic to fetch the medication. When I was done with all my HIV-related consultations and collecting the medication, I decided to do the test to check if I have cancer (VIA screening).
The nurse told me that there were whitish patches in my cervix. He said this means I have sores in my cervix and therefore a high chance of getting cervical cancer. He treated the sores and told me to come back to the clinic if I bleed. I am relieved now that I have done the test and have received the necessary treatment on time.
Swaziland
MSF Doctor
Testimony of a medical practitioner who acts as a hospital director, human resource manager, surgeon and senior doctor in an MSF-supported hospital near Damascus.
“August was the worst we’ve seen [here] medically. Hundreds of injured are coming in. Sometimes we have to go two or three days without sleeping. This month is incomparable to before. It is the worst I’ve seen. We are trying our best. We are trying to save lives and that’s what is keeping us going. We cannot do anything about the siege, it is what it is, and we are just struggling to survive. Of course, I have to hang on to hope. There is always hope.
There is much fear and depression in our community. You see it everywhere. Whenever there is a shelling or the sound of a plane, everyone desperately rushes home or to a shelter. The sound of a plane in the sky is terrifying. It is hard to explain how the situation is on the ground. You have to see it with your own eyes to understand, and even then it is unbelievable. We have seen huge numbers of injured over the past month; in these circumstances anyone who isn’t injured or dead can count themselves lucky.
Medically, we’ve had to become used to the situation, so we do things like rationing of medicine. Rationing has become an important part of our work. We have no choice, so we try to make do with what we have. There are too many patients, too many stories. But one patient shows the madness of this crisis – a child – who I will never forget until I die: he had injuries all over his face, his arms, his legs, and yet he was laughing! Just laughing and laughing. Children usually are afraid of our injections and needles, but he was not. He just laughed, laughed at everything.”
Syria

Ramadhani Lubunga
26, Burundian refugee
“I’ve been living in Nyarugusu for six months but have actually spent most of my life as a refugee: I grew up in another camp in Tanzania after my parents and I were forced to flee our country. I still find the conditions here difficult, though – it’s a struggle to get enough food and water and living in a tent wears you down. I’ve just been diagnosed with malaria and I can’t stop shivering and shaking. I have a headache and nausea and feel very cold. I’m also worried about my wife. She is four months pregnant but has been having stomach pains and is now in the camp hospital. I’m scared about what might happen to our unborn baby. Refugees never have a good life, but it’s better than living in fear at home. I can’t and won’t go back home. I will stay in this camp until I die.”
Tanzania

Taisiya Gregorivna,
82, has lived in Pavlopil, a village just a few kilometres from the contact line in eastern Ukraine, for the last 46 years.
Since 2014, Taisiya’s house has been shelled twice, forcing her to move to a safer place for a while. After receiving the support of her family to rebuild her house, she is now back home. Over the past months, Taisiya has received medical care from MSF for a heart condition she suffers from, as well as mental health support to cope with what she has been through.
“I can’t recall exactly when my house was first damaged by shelling, but I remember being very scared. Two shells hit the road, just in front of the main entrance, with shrapnel damaging the walls and some windows. The second time was during winter. I was alone in the house, and it was a very dark night outside. The roof was shelled twice. It was destroyed together with some of the rooms. All the windows also broke apart. I called my daughter who lives in Mariupol and left for the city the day after. I am so grateful for my family: my four children, six grandchildren and eight great-grandchildren. They are a great support. They take such good care of me; they are the ones who helped me to get my home back. Look around – others didn’t get so lucky.”
Ukraine
Amrita Ronnachit
Doctor
"Treating TB has some parallels with treating cancer. The treatment can be long and arduous, with toxic medications, which have terrible side effects. Pretty much the same as chemotherapy. And sometimes, it fails and the TB comes back. When it happens, it’s hard not to wonder if there was more that we could have done.
Today I visited a patient whose treatment has failed, and his results show that the TB is coming back. He is a young 19-year-old boy who has studied to become a mechanic. He was almost at the end of his treatment, just one month to go, when he started to have some symptoms again. At first he told himself that it was just the flu – he often gets it. But last week I saw his test results – it’s not the flu. And further testing has showed that his TB, which was the multi-drug resistant form, is becoming more resistant, what we colloquially refer to as ‘pre-XDR’. XDR, or extensively drug-resistant TB, is one of the most resistant forms of TB, and is very, very hard to treat successfully.
I tell him that the regimen we have been giving him is not working, and we will need to switch to another combination of drugs. It also means we will have to start his treatment all over again, a full 20–24 month course. The months of treatment that he has had so far won’t count, and he will have to restart his daily injections again.
“Twenty months of treatment? Fifteen to 16 tablets a day, right? No, I would rather die.”
Through the surgical mask I can hear his strangled breathing. He is trying not to cry but eventually he can’t hold back the tears."
Uzbekistan
Cecilia
58, lives in the Libertador municipality of Caracas. She witnessed her son’s murder at the hands of a criminal gang. She has been undergoing psychological treatment for four months.
”I feel better thanks to you, you are the only one who listens to me, understands me and does not judge me, makes me see the light when I see everything dark. When I'm on the street I remember what we talked about here [in the sessions] and then I feel better.”
Venezuela
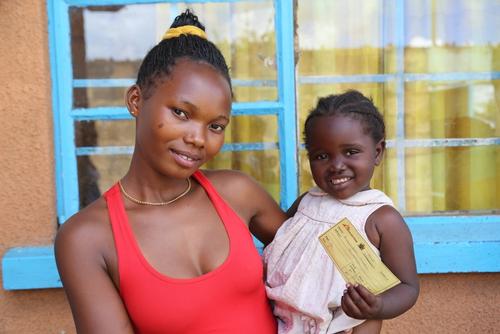
Mathilda
came to be vaccinated with her daughter, Edna, who had just turned three.
“In our neighbourhood, we have no clean water. People leave their rubbish in the streets and nobody does anything. I came as soon as I heard about the vaccination. The vaccine will help protect us against cholera. It can save lives. I encourage other mothers and community members to come and get vaccinated ... it's important that we are all protected.”
Zambia
Jabulani Simango*
21 years old, from Epworth
"When I was eleven years old, I fell seriously ill and I was taken to hospital in a wheelbarrow. I was started on ARVs but I didn’t understand why I was taking them. My parents died when I was young and my other family members didn’t have much information about HIV and AIDS … I was advised to join support groups for young people living with HIV. I then realised that I was not alone. There were many people my age who were HIV positive and from that moment onwards, I started to adhere to my treatment. MSF used to visit me at home to check if I was taking my medication consistently and in a proper way. After a while, my condition began to improve. When I showed signs of recovering, my family members began to accept me and my status. They began to realise that being HIV positive is not the end of one’s life."
* Name has been changed
Zimbabwe