Almost one-third of MSF projects in 2016 were dedicated to providing assistance to populations caught in wars, such as in Yemen, South Sudan, Afghanistan, Iraq, Nigeria and Syria.
MSF also provided assistance to people on the move, fleeing repression, poverty or violence, and in many cases subject to new forms of violence, exploitation or danger as countries closed options for safe and legal routes.
Our teams responded to other emergencies caused by epidemics and natural disasters and provided care and improved treatment for patients with diseases such as tuberculosis (TB) and HIV.
People in conflict
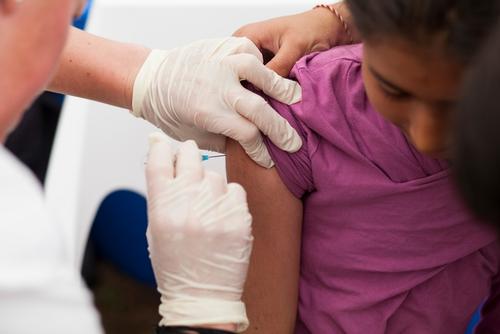
In many conflict zones, civilians and civilian infrastructure – including medical facilities – came under indiscriminate or targeted attacks. Millions of people had to flee their homes, sometimes multiple times. Our teams provided assistance to those caught in conflict and fleeing. They cared for pregnant women and newborns, treated the wounded and people with medical emergencies, managed chronic illnesses and responded to disease outbreaks, notably through vaccination campaigns. MSF also worked to meet other vital needs, such as for drinking water and essential relief items. From Lebanon to Tanzania, MSF teams mobilised to assist hundreds of thousands of people who had fled violence and conflict to other countries in search of safety.
In Nigeria, the armed conflict between Boko Haram and the Nigerian military displaced an estimated 1.8 million people in Borno state alone, with many communities cut off from the rest of the country for extended periods of time due to the conflict. In June, with only limited access due to widespread insecurity, MSF teams discovered shocking situations in villages such as Bama, where two out of 10 children under five were at risk of death due to malnutrition. Thousands of people regrouped in different villages were entirely reliant on aid.
By the end of the year, the humanitarian situation had improved in areas that were still accessible. However, the widespread insecurity and military restrictions presented a significant challenge to MSF and other humanitarian actors: the number of people in need of lifesaving assistance in inaccessible areas is unknown.
The armed conflict in Nigeria took on a regional dimension in the Lake Chad Basin, expanding across borders to Cameroon, Chad and Niger, with direct consequences for civilian populations. The crisis aggravated an already dire situation in a region suffering from poverty, food insecurity, recurring outbreaks of disease and almost non-existent health systems. MSF teams stepped up medical and humanitarian assistance in Chad, Cameroon and Niger for people fleeing Nigeria, as well as for local and displaced populations affected by the crisis.
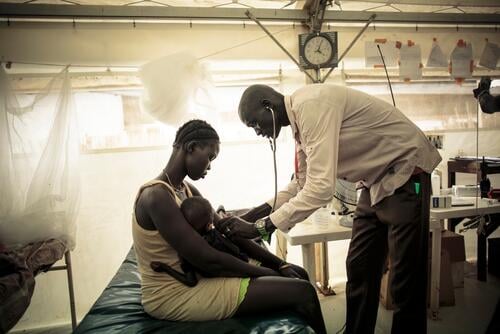
In South Sudan in July, intense fighting erupted between government and opposition forces in the capital, Juba. MSF opened clinics to provide emergency treatment for patients with gunshot wounds and injuries, as well as ongoing healthcare for conditions such as malnutrition, malaria and diarrhoea. Between August and December, we intensified our response to help South Sudanese refugees as the number of people fleeing violence increased, with hundreds of thousands arriving in Uganda, as well as in Ethiopia and Sudan.
In areas hit by violence, adapted solutions have had to be found. In South Sudan, to ensure continuity of care during instability for patients receiving HIV antiretroviral treatment, three-month emergency patient kits were prepared and distributed in the event of imminent displacement.
In Syria, MSF medical activities continued to be significantly constrained due to insecurity in opposition areas and a lack of authorisation by the Syrian government. MSF operated six medical structures in northern Syria in 2016. In inaccessible zones, such as besieged areas, our teams provided distance support to medical networks inside the country, through training, technical support and donations to medical facilities. This remains an extraordinary approach for MSF, made necessary by people’s extreme level of need and suffering and our lack of direct access.
The level of violence, and need, and lack of assistance led to sustained public communications by MSF through the testimonies of Syrian medical staff we supported, particularly in East Aleppo city and in besieged areas around Damascus.
Following the closure of the border between Syria and Jordan in June, around 75,000 Syrians were left stranded in the Berm/Rukban area. MSF teams and other aid actors were no longer able to reach the population. The border closures also prevented people from seeking assistance and protection outside Syria, a situation that is emblematic of a growing, pervasive reality across war zones, particularly in Syria.
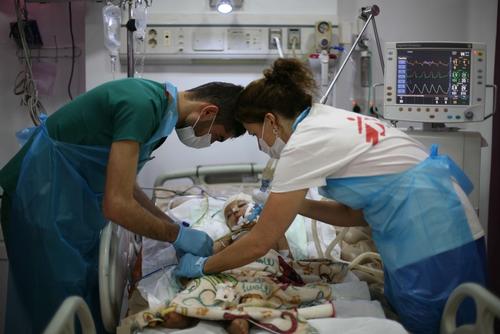
In Yemen, indiscriminate attacks against civilians and civilian infrastructure had a devastating impact on a country that was already one of the poorest in the region. To address the lack of healthcare and treat the increasing number of war victims, MSF scaled up its activities, making the response in Yemen our largest in the Middle East in 2016. MSF teams directly provided healthcare to patients in 12 hospitals and supported at least 18 other facilities.
On 15 August, an airstrike on Abs hospital in northern Yemen killed 19 people, including an MSF staff member, and wounded 24. MSF withdrew its staff from six hospitals in the north of the country following the airstrike, but continued to support the facilities. MSF resumed activities in northern Yemen in November 2016.
In May, the United Nations Security Council unanimously adopted Resolution 2286, condemning attacks on medical facilities and pledging to protect staff and patients in conflict settings. Yet airstrikes and shelling against health facilities continued, often by military coalitions acting with the direct or indirect involvement of Security Council members France, Russia, UK and USA. In 2016, 34 different health structures managed or supported by MSF were attacked in this way in Syria and Yemen.
Treacherous transit routes
The number of people crossing by sea to Italy increased from 153,000 in 2015 to over 180,000 in 2016. At least 5,000 men, women and children died while attempting the journey. MSF teams aboard three search and rescue vessels rescued 21,600 people from boats in distress in the Mediterranean. Our teams also recovered the bodies of people who drowned or were asphyxiated, crushed by the weight of hundreds of others.
With no safe and legal alternatives to reach Europe, almost all those rescued passed through Libya in search of assistance and protection. They described horrific suffering at the hands of smugglers, armed groups and individuals who exploited the desperation of those fleeing conflict, persecution or poverty.
In June, three months after the signing of the EU-Turkey deal, MSF announced it would no longer accept funds from the EU or EU Member States, in opposition to their damaging deterrence policies and continued attempts to push people and their suffering away from European shores.
In July, MSF began to run clinics in and around Tripoli, the Libyan capital, at some of the detention facilities established to lock up people on the move. Our teams witnessed catastrophic and inhumane living conditions.
In Central America, people from Honduras, Guatemala and El Salvador fleeing violence in their home countries were revictimised during their journey through Mexico to the United States. Of all MSF medical consultations in the migrant/refugee programmes in Mexico, a quarter of patients had been subjected to physical injuries and intentional trauma that occurred in transit. Patients reported that the perpetrators of violence included members of gangs and other criminal organisations, as well as members of the Mexican security forces – the very people responsible for their protection. These populations lack comprehensive access to medical care and suffer the consequences of aggressive deportation policies that disregard their need for assistance and protection.
Infectious diseases: response and innovation
The landscape of humanitarian medicine is constantly evolving, requiring MSF to keep pace with change. Adapting tools and approaches to ensure high-quality patient care is central to MSF’s work. In Niger, MSF participated in a clinical trial in the Maradi region to establish the efficacy of the new vaccine against rotavirus infection.
The infection is the leading cause of severe diarrhoea in children, which kills an estimated 1,300 globally every day. These deaths primarily occur in sub-Saharan Africa, where communities in remote areas have limited access to health services. The new vaccine is heat stable and does not require refrigeration, making it better adapted for populations most vulnerable to the disease.
Following the 2014- 2015 West Africa Ebola outbreak, MSF contributed to the development of a vaccine with potential to help prevent the spread of the Zaire strain of Ebola during future outbreaks.
A new cholera control strategy using a single-dose oral vaccine was found to be effective by MSF teams against outbreaks in Juba and was replicated in Lusaka, Zambia in April. Over 423,000 people were vaccinated against the disease, the largest cholera vaccination campaign ever undertaken during an outbreak. In the Democratic Republic of Congo (DRC), MSF vaccinated more than a million people against yellow fever. This required the daily organisation of 100 teams of 16 staff and a fleet of 65 vehicles carrying 4,000 ice packs and coolers.
When conflict disrupts health systems, infectious disease outbreaks can become more frequent and more devastating in their impact. Prevention and control strategies were part of our response in conflict settings too, such as in Nigeria, Yemen, Central African Republic, South Sudan and Syria.
Vaccination campaigns are one of the most effective ways to prevent and respond to epidemics but are only possible if vaccines are available at affordable prices. Pneumonia remains the leading cause of death in children under five, and the high price of the pneumococcal conjugate vaccine (PCV) places it out of reach for many developing countries. In Greece, for example, MSF paid US$68 per dose of PCV – 20 times more than the lowest global price – to ensure protection for refugee children.
MSF had long urged Pfizer and GlaxoSmithKline (GSK) – the only two manufacturers of the vaccine – to offer the lowest global price to humanitarian organisations. In 2016, thanks to nearly half a million supporters who participated in MSF’s A Fair Shot campaign, both companies agreed to lower the price of the vaccine for children caught in humanitarian emergencies.
MSF remains the largest non-government provider of TB treatment worldwide. In 2016, our teams treated over 2,000 patients for drug-resistant forms of the disease. MSF is contributing to clinical trials, initiated in 2016, aimed at establishing evidence on the safety and efficacy of the new TB drugs bedaquiline and delamanid. The trials aim to determine if these two drugs, used in a variety of novel combinations, are more effective or simpler than existing regimens, and if patients experience fewer side effects. If successful, these clinical trials could revolutionise treatment of drug-resistant TB, provided that the drugs are made accessible to patients in need.
MSF’s work to deliver free, lifesaving medical care where it is needed most is only possible thanks to the vital, ongoing commitment of our supporters. We extend our sincere gratitude to you all and pay tribute to the tens of thousands of MSF staff who delivered healthcare to patients in 71 countries in 2016. We also take this opportunity to remember our MSF colleagues who lost their lives while on mission. Our teams remain actively committed to finding and bringing to safety our three colleagues abducted in the DRC in 2013. Philippe, Richard and Romy: our thoughts are with you, your friends and your families.