The below is an outline of activities MSF undertook in the wake of Cyclone Idai and the subsequent flooding in Mozambique, Malawi and Zimbabwe in March 2019.
We wrapped up all cyclone and flooding-related activities in May 2019.
Background
A weather system that produced heavy rains flooded parts of Malawi in early March 2019, before developing into Cyclone Idai which struck Mozambique and Zimbabwe on 14-16 March, 2019.
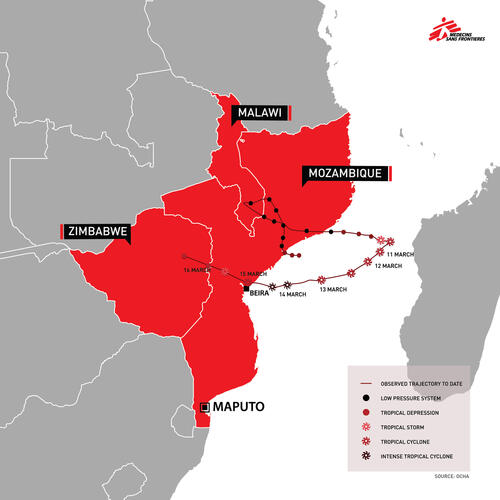
Flooding in Malawi has displaced nearly 87,000 people in campsOCHA, 26 March, with the district of Makhanga one of the worst affected areas, which remains an island, cut off from all road access.
In Mozambique, Cyclone Idai wreaked havoc in the city of Beira, home to some 500,000 people, as well as in the surrounding districts of Manica and Sofala, where it has destroyed the lives and livelihoods of hundreds of thousands more people.
In Zimbabwe, the impact from the cyclone on the eastern highlands has been massive with nearly 22,000 people displaced and several bridges and roads have been washed away. Some communities are reachable only by foot.
We have emergency response teams on the ground in all three countries. We are undertaking medical activities, including treating cases of cholera and acute watery diarrhoea. We are also responding to humanitarian needs, such as providing non-medical items including buckets and soap, and ensuring safe water and sanitation.
Teams in all the affected countries have mobilised to provide medical and non-medical assistance. Our warehouses in Brussels and Dubai have sent tons of supplies to the affected areas, particularly Mozambique.

Emergency cargo sent to Mozambique
Mozambique
Mozambique, and particularly the city of Beira, in the centre of the country, has been the hardest hit by Cyclone Idai, which struck late on 14 March.
Situation
High winds and high waters have killed 602 people, injured more than 1,600According to the Government of Mozambique as at 8 April and damaged or destroyed thousands of buildings - homes, schools, health centres and hospitals - across the area. Many families are left homeless and thousands of people are still without reliable access to clean water or electricity.
The government declared a cholera outbreak in Beira on 27 March, and later in Tica, Buzi and Dondo. Our teams are also seeing cases of acute watery diarrhoea elsewhere. We are working in collaboration with the Ministry of Health to treat people who are already ill, while setting up clean water supplies and informing the community about how to protect themselves in order to stop more people from becoming sick.
Teams have been treating people with the immediate needs in the wake of the cyclone, including injuries, infections and cases of diarrhoea and cholera, normal functioning of the health system must also be supported with mothers still needing to deliver babies safely, and people still needing vital medication for illnesses such as HIV.
More than a month after the cyclone struck, teams are continuing to monitor the health situation, particularly for malaria - with mosquitoes prevalent amongst the stagnant water - and for malnutrition, as the cyclone struck just before the harvest, diminishing people's food stocks.
According to the government of Mozambique as of 22 April
715,000
715,
239,682
239,682
72,793
72,793
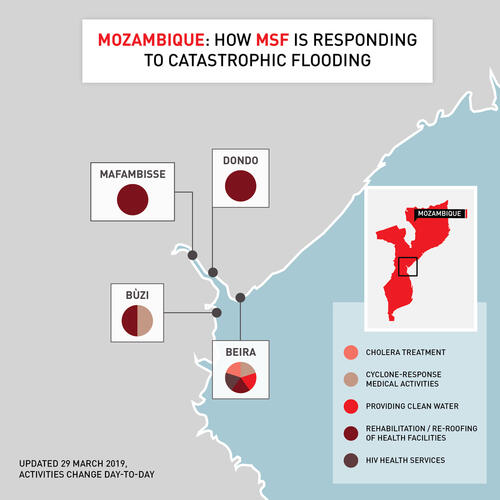
Beira and surrounds
- Ninety percent of the area around Beira has been damaged, with roads, electricity and communications having been cut off.
- Buildings have been submerged and severely damaged; many people are staying with family or friends or in transit centres because their homes are uninhabitable.
- Healthcare infrastructure has been damaged, including the hospital.
- While clean-up efforts by communities are underway, clearing the streets of debris and uprooted trees, extensive repair work to buildings and infrastructure is much needed.
- The cyclone substantially damaged the city’s water supply system, resulting in many people having drunk from contaminated wells or stagnant water.
- The Government declared an outbreak of cholera in the city on 27 March.
Tica
- Houses, farmland and structures have been destroyed and some are still flooded.
- The health centre was badly damaged.
- More than 55,000 people, out of 300,000 inhabitants in the district, are homeless.
- Access to clean water is severely limited, with just one clean water well available for thousands of people.
- A cholera outbreak was declared in the district, Nhamadanta (of which Tica is the main town).
Dondo
- The town and surrounding area sustained damage from the cyclone and flooding, including to local health infrastructures.
- A cholera outbreak has been declared by the Ministry of Health.
Buzi, Dombe, Macharote, Matua and Mafambisse
- The areas surrounding these towns sustained damage from the cyclone and subsequent flooding, including to local health infrastructures.
- Some areas lack access to clean water.

MSF flood emergency response 101
Response
We currently have nearly 900 staff on the ground in the flood-affected areas, the vast majority of whom are Mozambican.
Staff on the ground in Mozambique as at 26 April 2019:
755
755
140
14
120
12
Much of our work is in support of the local Ministry of Health, who have prioritised access to clean water - although thousands in outlying areas still need improved access - the treatment of cholera in establishing treatment centres and units, and the prevention of cholera and acute watery diarrhoea through vaccination campaigns.
Fears of a mass cholera outbreak in Beira have not materialised, with the number of cases now drastically diminishing. We remain vigilant about new cholera hotspots in other areas and are running cholera-treatment centres or units in three towns or villages, although these are shortly expected to be closed or handed over given the comparatively few cases.
Cholera situation and response as of 22 April:
6,596
6,596
803,125
803,125
98 %
98%
Beira
MSF was working in Beira before the cyclone to provide antiretroviral medicines (ARVs) for people living with HIV and to provide treatment for patients with advanced HIV. Following the cyclone these activities were disrupted, but have now been completely restarted. In Beira, 16 percent of people are HIV positive.
MSF teams are undertaking medical and non-medical activities in Beira and in areas on the outskirts of the city. Medical activities include treating cholera in cholera treatment centres (CTC) and cholera treatment units (CTU):
- Running one 40-bed CTC in Macurungo.
- Running an ambulance and referral system to ensure that suspect patients are taken to the closest CTC with available beds.
- Running oral rehydration salt points in the community so those who are not too sick with cholera can avoid adding to the workload of the treatment centres.
- Running water and sanitation and health promotion activities in the poorest areas of Beira to talk about the risks of cholera and help the community protect themselves.
- Wastewater management and desludging of latrines both in the CTCs and in the community.
- Cleaning, disinfecting and repairing wells that were damaged or contaminated by the cyclone.
- Installing water treatment plant at Chingussura to provide clean water for the health centre, CTC and local community.
- Supporting the local water authority to repair the water network.
- Distributing chlorine and soap to over 10,000 households, plus distributing kits to help people repair damaged homes.
- Distributing water and sanitation kits in remote villages.
- Providing mental health support to the community and to the Mozambican staff who went through the trauma of the cyclone.
- Training MoH psychologists on first-aid mental health support in several health centres, as well as referral from the mobile clinics
- Providing health consultations through mobile clinics in hard to reach areas (mainly impoverished neighbourhoods) and in transit camps.
Buzi
- Rehabilitating the health centre to make it fit for use again.
- Working on the supply of clean water in the community.
- Undertaking health promotion in the community to explain the psychological symptoms that people might be experiencing after the trauma of the cyclone and flooding.
- Running a four-bed cholera treatment unit.
- Providing peri-natal (just before and just after birth) care in the community as well as supporting the local midwives at the hospital.
- Mobile clinic running in remote communities of Grudja, Bandua and Inharongue as well as Guara Guara.
Dondo
- Treating cholera patients in two CTUs (a 16-bed unit in Dondo and 10-bed unit in Mafambessi) and four oral rehydration points.
- Providing ambulance referrals to the CTU.
- Conducting mobile clinics in remote areas to ensure access to primary health care with a focus on malaria and diarrhoea.
Rehabilitation of the damaged roof in three health centres to ensure functionality. - Distribution of 6,800 hygiene, cooking, shelter kits to families living in Chibuabuabua, Tundane, Savane.
Dombe
- Setting up a water treatment station in Dombe to provide up to 2,000 litres of water per hour for the Matarara settlement camp.
Tica and Nhamatanda district
- Repairing the health centre in Tica which has been damaged by Cyclone Idai to have it fully operational again.
- Undertaking epidemiological surveillance and testing where needed for malaria, acute watery diarrhoea, mental health and malnutrition.
- Provide medical support to the health centre in Nhampoca, including setting up a three-bed in-patient department.
- Testing and treating for malaria and undertaking nutritional screenings.
- Providing mental health consultations.
- Running mobile clinics in remote areas, and assisting with the distribution of over 10,000 mosquito nets.
- Supporting the health centre in Metuchira and setting up a cholera treatment unit.
- Running mobile clinics in remote areas in the north of Metuchira.

Local MSF staff in Beira explain current situation
Zimbabwe
Cyclone Idai hit Chimanimani, a small district of approximately 30,000 people in Manicaland province, late Friday 15 March, after passing through Mozambique.
Situation
- The damage in Chimanimani district is massive, with many roads completely wiped away for several kilometres or blocked by rock falls, and the only way to reach some communities is now by foot.
- Many have been left without homes or livelihoods.
- Access to safe drinking water is an issue with many pipes washed away.

22,000
22,
330
33
181
181
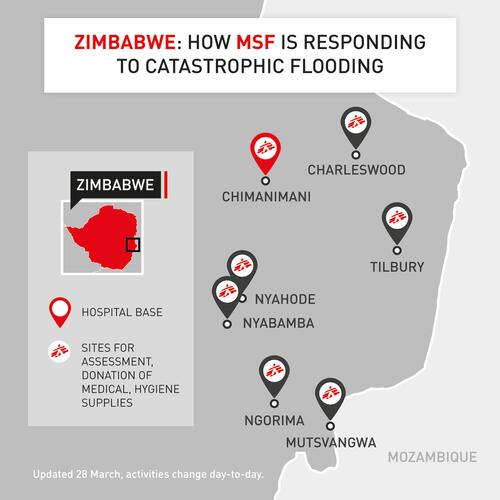
Response
We have sent an emergency response team to the mountainous areas of Manicaland province, including the districts of Chimanimani and Chipinge.
Chimanimani and surrounds
After an MSF team was finally able to access the district and provide a response in the hardest-hit areas, more than a month after the cylcone, MSF teams are scaling down their work and preparing to leave by the end of April. Recent interventions include:
- Providing technical and logistical support during an oral cholera vaccination campaign which reached 128,251 people in Chimanimani.
- Assisting with psychosocial support to affected communities through psychological first aid, training of trainers on basic counselling skills and identification of trauma, anxiety, depression and grief, and mentoring and training for nurses and village health workers in selected clinics in Chimanimani.
- Providing group and individual mental health consultations in clinics and seven settlements for internally displaced people.
- Providing water, sanitation and hygiene support in Chimanimani hospitals and IDP camps, as well as conducting assessment in those areas and in three out of the 23 wards of the district.
- Providing health promotion activities on good water, sanitation and hygiene practices to prevent water borne diseases.
Longer term, the consequences of blocked access should be considered: electricity was disrupted affecting routine vaccination services; impending stockouts of medical supplies and drugs; treatment interruptions for HIV, TB and chronic disease patients; and a lack of detergents and chlorine.
Chipinge
- Providing technical and logistical support during an oral cholera vaccination campaign which reached 334,761 people in Chipinge
- Providing aqua-tabs to ensure people have access to clean water.
- Providing essential medicines and medication for diseases including diabetes, hypertension, and asthma.
- Assisting with psychosocial support to affected communities.
Malawi
Extremely heavy rains in lower Shire River districts of Chikwawa and Nsanje, in Malawi’s far south, has been compounded by further rains from Cyclone Idai. The Makhanga and Nsanje districts were the worst affected, with 14 of Malawi’s 28 districts experiencing severe flooding.
Situation
- Flooding affected the majority of Nsanje district, in southern Malawi; rains have now largely stopped and access to the flooded areas is improving.
- Some areas remain under water or cut off with limited phone communication.
- Around 16,000 households are affected, according to the national disaster report; a huge number of houses have collapsed.
- Many thousands of people are in displacement camps and makeshifts sites such as schools and churches. Big reconstruction efforts will be required in coming weeks.
- There's been huge destruction of agricultural crops and animals; an estimated 50 percent of the area’s crops might have been lost.
- Electricity has returned to hard-hit Makhanga district, on the eastern bank of the Shire river, which essentially remains an island, cut off from all road access.

87,000
87,
677
677
56
56
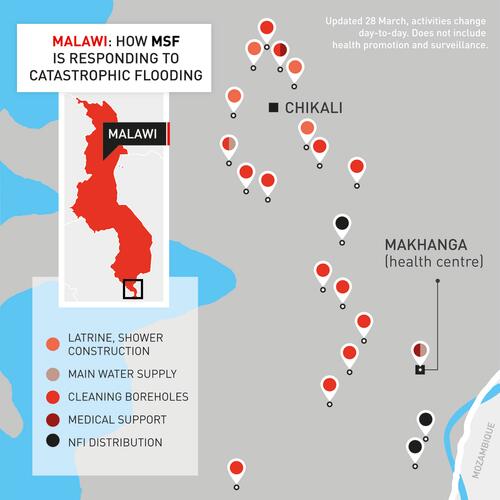
Response
We had a team of 18 people working with local authorities, communities and the health ministry to cover the needs of people with health, sanitation and non-food-item supplies. MSF has finished or handed over all activities in Malawi, and wrapped up our emergency response in mid-April.
Overall
- Outreach teams visited communities to clean and repair boreholes plus test the water quality to ensure access to clean water.
- Teams built basic latrines, showers, shelters and distributed non-food items and hygiene kits, educating communities on hygiene and safe water practices.
Makhanga
- A team of 18 people is supported the health ministry, moving by boat, to cover the needs of an estimated 18,000 people with health, sanitation and non-food-item supplies.
- In Makhanga health centre, we ensured primary health, HIV services and basic disease surveillance, and undertook approximately 150 consultations per day.
- Worked with the Malawian District Health Office, on an outreach clinic to ensure access to primary health care services and to drugs for patients with chronic diseases, including HIV and tuberculosis, who lost their medications in the floods.
- Reached more than 2,000 households with hygiene kits, which includes buckets, cups, and soap.
- Constructed a basic, four-bed cholera treatment unit and conduct training, to be prepared just in case the need arises.



