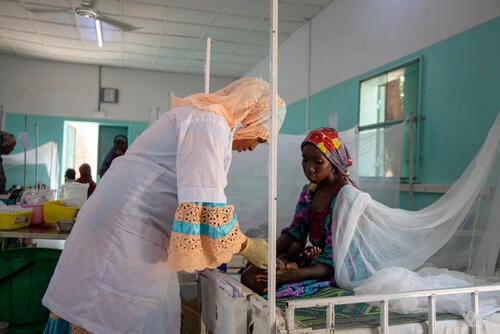
The global fight against the three main infectious killer diseases – HIV/AIDS, tuberculosis (TB) and malaria – has ground to a halt. In recent years, teams from Médecins Sans Frontières (MSF) around the world have seen worrying signs of a reversal in progress against all three diseases, compounded by the COVID-19 pandemic and economic difficulties. If donor countries are to help beat these deadly diseases, they will need to demonstrate their commitment with increased pledges at the upcoming Global Fund to Fight AIDS, Tuberculosis and Malaria (Global Fund) replenishment round.
The US$18 billion asked for by the Global Fund is the bare minimum of what is needed. In fact, this amount would leave a wider, unfunded financial gap than previously, rather than providing the means to get the fight back on track. Anything less than $18 billion will create serious problems for millions of people living with and dying from these three diseases.
MSF teams witness the very real consequences of the funding shortfall for our patients. This briefing paper presents examples from seven countries: Central African Republic, Democratic Republic of Congo, Guinea, Mozambique, Myanmar, South Sudan and Uganda. (For a snapshot of the situation for each country, see page 6.)
The seriousness of the situation today should come as no surprise. In 2019, MSF published a report warning that the HIV/TB response had come to a standstill, largely because the world was too optimistic about how much of the financing for programmes to combat the diseases could be shouldered by low- and middle-income countries.
A new assessment by MSF teams in 2022 shows how the COVID-19 pandemic and concurrent economic and social crises have exacerbated existing problems for HIV, TB and malaria. The consequences for people living with all three diseases are dramatic.
Fight against TB, HIV and malaria going backwards
Illness and deaths from TB clearly show the reversal of gains made in previous years. As many people are dying from TB now as they did in 2017, with 1.3 million deaths per year. An estimated 10 million people become infected with the disease each year. Fewer people with drug-resistant forms of the disease are receiving treatment now compared to 2019-2020, with a 19% drop for multidrug-resistant TB, a 37% drop for extensively drug-resistant TB, and a 16% drop for people coinfected with HIV and TB.
Instead of meeting the 2020 objective to reduce the number of new TB infections worldwide by 20 per cent compared to 2015 figures, several countries – including Guinea, South Sudan and Mozambique – have actually seen increases in the number of infections. The 2020 objective to reduce global TB deaths has also not been reached.
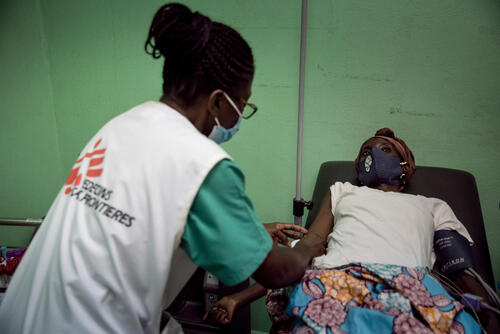
It is a similar situation with HIV: the numbers of people getting tested for the disease have fallen by 22%, while prevention services have dropped by 11% from 2019 - 2020. Some 9.5 million people living with HIV are still not on treatment, while almost one-third of those who seek to start treatment already show signs of advanced HIV disease, putting them at high risk of imminent death. During the COVID-19 pandemic, large numbers of people living with HIV interrupted their treatment; now they urgently need to restart if they are to avoid the slide towards AIDS and an early death.
The number of people falling ill with malaria has regressed back to 2015 levels (at 59 per 1,000 people at risk). The number of people dying from malaria is up 12 per cent from 2019 numbers, with 627,000 deaths.
MSF teams seeing the reality of cuts on the ground
One obvious consequence seen by our teams is the loss of all those gains made over previous years. We are worse off on several fronts compared to a few years ago. The lost ground must first be recovered before renewed progress can be made.
As countries face insufficient funding for their medical programmes, they have to cut effective interventions from their plans. HIV programmes for pregnant women and their unborn babies are typically one of the first victims of such cuts, as are programmes targeting vulnerable groups such as men who have sex with men, sex workers and drug users.
Another effect of the funding shortfall is a substandard quality of care, which is counterproductive and potentially very dangerous for people with HIV, TB or malaria. Essential elements are left out of the standard package of care, such as tests for the level of virus in the blood, medicines to treat people with opportunistic infections and complications linked to AIDS, and adapted paediatric TB care.
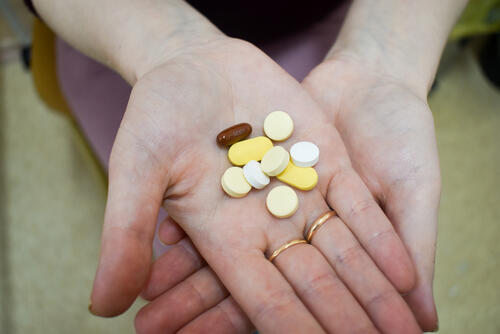
Less support for patients and community programmes
There is also less support for community health programmes, although they have proven to be highly effective. When money is tight, implementing innovative approaches and offering the most recent treatments are delayed, despite the fact that these are sorely needed and have proved their value in the past.
Ultimately, it is the patients who bear the brunt of the funding gaps. People can be forced towards harmful coping mechanisms, such as borrowing money at very high interest rates, pawning their assets or deprioritising other necessary household expenditures. This in turn increases their vulnerability and pushes them further into poverty.
Countries must close the (massive) gap
An estimated $130 billion is needed for HIV, TB and malaria for the period 2024-26. With the Global Fund supplying 14% of that budget – assuming that $18 billion is raised – and other external funding supplying another 19%, domestic funding should account for 45%. This leaves a huge gap of 22%.
But at present, it looks very unlikely that enough domestic funding will be mobilised to cover 45% of the $130 billion. With over-optimistic expectations for domestic funding, we can expect an actual gap that is much bigger than the predicted 22%.
The key question is if the September Global Fund replenishment conference will succeed in mobilising the necessary funding, and if countries will step up their pledges by at least 30 per cent on previous pledges. Some firm commitments have already been made by the US and Japan, but other countries are keeping us in suspense as to if, when and how much they will pledge.
A shortfall of European donors, in particular, would have a doubly negative effect, as it would proportionally cut into the US pledge, which is limited to a maximum of one-third of the total amount.
It is important to remember that the $18 billion asked for by the Global Fund replenishment is an absolute minimum and will need to be complemented by other international funding. At country level, priority will have to be given to fill existing and future gaps.
Many international donors have withdrawn from bilateral funding of HIV, TB and malaria programmes; to complement countries’ contributions to the Global Fund, donors should re-engage or risk seeing all the progress undone.