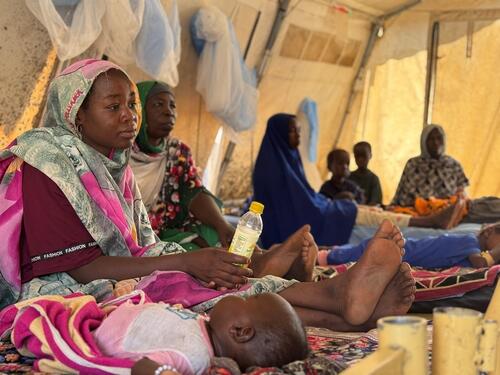
In 2018, an estimated 311,000 women died of cervical cancer. More than 85 per cent of those women lived in low- and middle-income countries. In the same year, 570,000 new cases were diagnosed.
The inequality of cervical cancer is stark. In 42 countries it kills more women than any other cancer. Contrast that with Switzerland where it ranks 19th, which makes it the least fatal. Mortality is currently highest in Malawi, where Médecins Sans Frontières (MSF) has its most comprehensive programme, with Mali and Zimbabwe two more countries not far behind. Worldwide, Australian and New Zealand women are among the least likely to be affected.Arbyn M, Weiderpass E, Bruni L, de Sanjosé S, Saraiya M, Ferlay J, Bray F. Estimates of incidence and mortality of cervical cancer in 2018: a worldwide analysis. The Lancet Global Health. 2020 Feb 1;8(2):e191-203.
Cervical cancer is preventable—and curable, if detected early.
So, why are women still dying of cervical cancer?” First, we need to understand more about how the cancer develops.
The figure is projected to increase in coming years, yet the world is largely silent about these deaths.Dr Severine Caluwaerts, MSF obstetrician
How can you get cervical cancer?
Nearly all cases of cervical cancer are attributable to persistent infection by the human papillomavirus, or HPV. HPV is sexually transmitted—in fact, it is one of the most common sexually transmitted infections and affects both men and women. There are over 100 strains of HPV, but two particularly virulent strains, types 16 and 18, cause around 70 per cent of all cases of cervical cancer.
In many women, the infection will spontaneously clear. But for others, over time, chronic infection causes abnormal changes in the cells of the cervix: pre-cancer. If left untreated, these can progress to cancer, silently—but, as explained below, not invisibly—over a period of 15 to 20 years.
However, HPV infection is especially aggressive in HIV-positive women and girls, which means they can fast track to cervical cancer in less than half that time.
Meanwhile in Malawi, due to late detection, the average age of diagnosis is 49—often too late to avoid terminal illness and the suffering that accompanies it.
These women are the cervical cancer cases that should not be, because they could have been prevented.

How do you prevent cervical cancer?
How can you prevent cervical cancer?
Prevention of cervical cancer should start as early as age nine—before girls are exposed to HPV.
This is primary prevention, in the form of vaccination against HPV, which is recommended by the World Health Organization (WHO) between the ages of 9 and 14.
Screening for pre-cancer is the second step, combined with treatment. In lower income countries “screen and treat” programmes make it possible to identify, destroy or remove pre-cancer and, if regular screening continues, detect any recurrence and manage it, or refer the patient for higher level care.
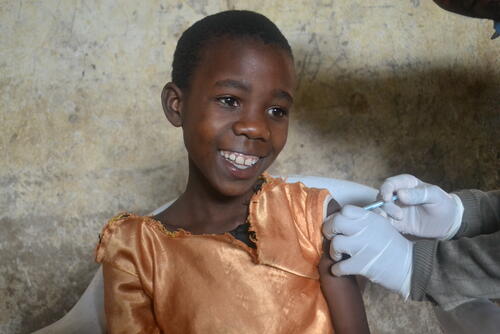
Vaccination
Since the first vaccine’s introduction in 2006, HPV vaccination programmes in early uptake countries like Australia have shown impressive success. There are now confident predictions that cervical cancer will be eliminated in high-income countries in the near future.
There are currently two pharmaceutical corporations that produce three vaccines targeting cancer-causing HPV strains. Pharmaceutical company Merck dominates sales with two of those three.
But Merck has failed to meet the demand from the countries hardest hit by cervical cancer. The vaccine remains unaffordable and unavailable for many countries, with Merck prioritising higher-paying customers such as those in European and North American markets. As a result, only 21 per cent of low-income countries have started using an HPV vaccine, compared to 79 per cent of high-income countries.Data as at October 2 2019 accessed from WHO Immunization, Vaccines and Biologicals database, available at <a href="https://www.who.int/immunization/documents/en/">https://www.who.int/immunization/documents/en/</a> As a stop-gap measure for this critical vaccine shortage, WHO has issued new guidance, including that some countries vaccinate a single-age group only, such as just 9-year-olds.
As a result, MSF is seeing countries that have committed to roll out HPV vaccination forced to leave millions of girls unprotected. MSF is also limited in any additional vaccination efforts it might provide.
Screening
In 2018, MSF screened over 20,000 women in five countries. This is where MSF has most significantly stepped in, to halt the advance of pre-cancer.
Screening remains key to cervical cancer prevention despite the effectiveness of HPV vaccination, especially as many women today grew up before introduction of the vaccine, and many young girls still don’t receive it. But if you screen, you must also be able to treat.
In low-resource settings, “screen and treat” has been designed to achieve as much as possible for the patient in the one visit in their local clinic, by one healthcare provider.
Using visual inspection with acetic acid, or VIA, nurses and midwives are trained to detect abnormalities or pre-cancer on the cervix with their naked eye, or using a camera or a smartphone (cervicography). They are then also equipped to treat what they find, within a defined extent. Using an electrical probe they can freeze (cryotherapy) or heat (thermal ablation) the lesions to destroy them. The whole consultation, with counselling throughout, can be completed in 30 minutes.
Pre-cancer that cannot be treated on the spot is referred for LEEP or loop electrical excision procedure. If cancer is suspected, Médecins Sans Frontières can also make arrangements for a biopsy.
The relatively simple infrastructure and equipment needed for screen and treat makes it a cost-effective strategy in places where sophisticated analytics are out of reach due to cost, distance, or the complex resources needed to support them. MSF has also taken screen and treat on the road, to make it accessible for even more women: installed in a bus in the Philippines, or in a pop-up tent in Zimbabwe.
To help strengthen capacity in ministries of health or local partners, MSF also focuses on mentoring nurses and introducing regular quality assurance through peer review and expert support. Meanwhile community engagement is essential: to share the story of how screen and treat prevents cancer; how waiting for symptoms is waiting too late; and how a positive screening result is usually not a cancer diagnosis, but an opportunity to stay well.
In Gutu district, Zimbabwe, screen and treat take-up has now reached 75 per cent of the catchment population.

Sister Mercy Mandizvo speaks about cervical cancer in Zimbabwe
What if cervical cancer develops?
Surgery
If screening is missed, and a cancer develops, curative options are limited in low-resource settings. Surgery is a high-level skill often missing, but chemotherapy and radiotherapy can be even rarer.
A complex and invasive cancer, cervical cancer is only able to be treated by surgery in its early stages. The operation, an extended abdominal hysterectomy, and the ensuing hospital stay can be daunting for the woman and her family in many ways.
To complete the full spectrum of prevention and treatment in its Malawi programme, MSF opened an operating theatre and inpatient ward in the capital, Blantyre, in December 2019. Meanwhile in Zimbabwe and Mali, for example, we directly support women in their referral to an identified specialised hospital that can provide this lifesaving option.

Cervical cancer patient Rumbidzai Mushayi talks about surviving cancer
What exactly is MSF doing to address the issue?
In 2019, Médecins Sans Frontières provided cervical cancer care across five main projects worldwide.
Zimbabwe
Together with the Ministry of Health and Child Care, Médecins Sans Frontières offers a range of prevention and early treatment services for cervical cancer in Gutu District, in six health facilities. In 2015, our teams began working with MoHCC to screen women for abnormalities and pre-cancerous lesions using VIAC (visual inspection with acetic acid and cervicography). The teams provide on-the-spot treatment (cryotherapy) for pre-cancerous lesions and refer women with more invasive lesions for surgery, and those with cancer for surgery.
Philippines
A 2015 assessment by Médecins Sans Frontières confirmed the need for sexual and reproductive health services in Tondo, a densely populated and impoverished area of the capital Manila in the Philippines. In 2016, we launched a partnership that continues today with local non-government organisation Likhaan to support a clinic providing screening for cervical cancer and cryotherapy alongside other sexual and reproductive health services. Since 2016 we have screened more than 9,300 women, including 6,400 who were being screened for the first time, in static and mobile clinics. Those with pre-cancerous lesions were provided immediate treatment. In 2017, we also vaccinated 22,000 girls aged between 9 and 13 against HPV in Tondo.
Eswatini
Médecins Sans Frontières began providing VIA screening and cryotherapy for women aged 25-45 in the predominantly rural Shiselweni region of Eswatini in 2016, in collaboration with the Ministry of Health. MSF provided all supplies and logistical support for screen and treat, including treatment and management of other infections detected in the consultation. MSF recruited VIA staff, supported training for nurses and piloted a mobile health and telemedicine programme for nurse-led diagnosis. Training was conducted in 30 facilities in 2019, and the project was handed over to the Ministry of Health later that year.
Mali
In Bamako, Mali’s bustling capital city, Médecins Sans Frontières runs an oncology project for women with cervical and breast cancers, set up in partnership with Mali’s Ministry of Health. In 2018 we began offering palliative care and support services in the public haemato-oncology department of Point G University Hospital and in patients’ homes. Teams also offer consultations in supportive and palliative care for patients with other types of cancer. In 2020 we also began supporting cervical cancer screening services for women in Bamako. We have also supplied equipment and implemented training to introduce thermal ablation in a number of health centres.
Malawi
Médecins Sans Frontières’ comprehensive cervical cancer project in Malawi targets all stages of primary and secondary prevention and tertiary care. Opened in 2018 and now operating across health centres in Chiradzulu district and a hospital and health centre in Blantyre, it provides HPV vaccination, VIA screening and pre-cancer treatments. As of December 2019, a dedicated operating theatre began offering surgical treatment. Case management for patient with advanced-stage cancer includes palliative care. Chemotherapy will be offered to eligible patients from later in 2020. In January 2020, in conjunction with the Ministry of Health, MSF implemented an HPV vaccination campaign for 8,500 nine-year-old girls in Chiradzulu district.
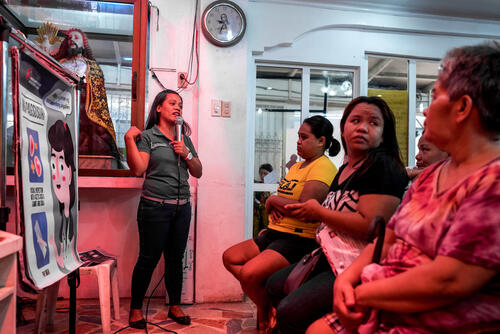
What happens if the gaps aren’t filled?
MSF continues to see women in their 40s and 50s come too late for care, diagnosed with advanced cancer beyond reprieve.
They may have been suffering, and deteriorating, in a community that knows little about the disease. They may already have spent considerable money seeking care for unexplained symptoms, or simply lost money as it became harder to work. Their cancer may be disfiguring, and distancing.
The burden of cervical cancer has created an enormous need for palliative care, a gap MSF has recognised in its efforts to reduce suffering.
In Mali’s capital, Bamako, we support a programme of hospital- and home-based palliative care in one of the only hospitals in the capital with this type of service. Some 50 per cent of the patients travel from out of town. The service covers prevention and management of symptoms, pain relief, and psychosocial and spiritual support. Women are also treated for the side effects of chemotherapy, non-cancer disorders, and wounds caused by tumours.
Twice a week, the team also travels to the homes of patients, often so destitute or unwell they simply cannot go to the hospital.
How can we end preventable deaths from cervical cancer?
Huge advances have been made in high-income countries, yet there are increasing gaps between the best quality of care and what is provided in resource-limited settings. The WHO has released its draft strategy on elimination of cervical cancer, on the table for approval at the World Health Assembly in May. Without scale up in vaccination, screening and treatment, the death toll will continue to mount. What more can be done?
There needs to be greater supply of the HPV vaccine for the girls most at risk. The vaccine needs to be available at a lower price, to ensure that it can be accessed affordably by countries. Humanitarian organisations such as MSF must also be able to access the HPV vaccine at an affordable price for the people they care for.
There is also no time to lose to be able to screen and treat more women. This needs a trained and maintained health workforce, and a reliable flow of material supplies. “Screen and treat” needs to be integrated as standard care to existing health services, including primary health care centres in rural regions and HIV programmes. Screening also needs to work harder: newer, more sensitive methods such as HPV screening need to be incorporated, to detect affected women earlier. Between 2017 and 2018 MSF doubled its screen and treat coverage and has dedicated resources to develop evidence on scalable models of care. Yet this remains a small contribution to an enormous problem.
Cancer treatment must be urgently expanded. With mortality still so high, chemotherapy, radiotherapy and surgery need to be accessible for women diagnosed early enough. Lastly, to help women and their communities navigate pre-cancer and cancer, the importance of psychological and social support systems cannot be overlooked.
It is unacceptable that a woman’s likelihood of dying from cervical cancer depends largely on where she lives.