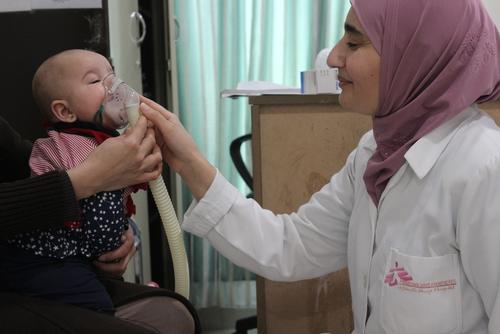
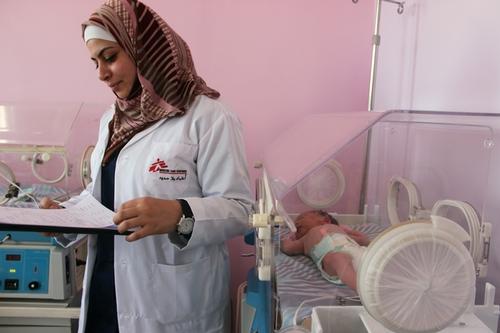
MSF mental health activities manager Heidi Mitton explains the mental healthcare needs and services in Irbid, Jordan, where MSF runs a non-communicable diseases (NCD) project for Syrian refugees and vulnerable Jordanians.
MSF teams at our non-communicable diseases (NCD) clinic in Irbid, Jordan, have worked with Syrian refugees living outside camps since December 2014. We opened this project to respond to the massive needs of the Syrian refugee living in non-camp settings.
Jordan hosts around 671,900 registered refugees, and many more who are without registration. Around 125,783 Syrians live in camps, while the rest reside in cities and villages around Jordan.
Although displaced people living in host communities do not always receive the same media attention as those in camps, they often face difficulties accessing healthcare and other basic services, and can face unique economic and social challenges as they try to integrate a new society.
Moreover, 30 per cent of our patients are vulnerable Jordanians suffering from similar conditions.
In order to improve their physical health, patients in highly stressful situations often need help managing the emotional and social effects of these stressorsHeidi Mitton, MSF mental health activities manager
Our work in the mental health team has taught us the many needs and stories these patients experience in their daily lives.
Mental healthcare was incorporated into the Irbid NCD programme in 2016, and has since benefited 630 patients, through 2,548 individual consultations and 37 group sessions.
The starting point was acknowledgment that, in order to improve their physical health, patients in highly stressful situations often need help managing the emotional and social effects of these stressors. A more holistic approach to treatment was required.
Adults affected by emergencies have a higher risk of suffering from common and severe mental health conditions such as depression, anxiety and post-traumatic stress disorder. Even in the years after arriving to safety, many of our patients continue to experience these symptoms.
Zuhair, a father of three and a Syrian refugee from Homs, once told us his wife was waiting for him to finish his sessions to take his spot, as she realised he had changed a lot after enrolling in the mental health programme. “I took about 10 to 15 sessions. I feel much better and much happier,” Zuhair said.
The symptoms could worsen if people continue to live in stressful conditions. The mental health team works closely with patients in order to address their condition and find new coping strategies for a combination of factors - from the multiple stressors related to the chronic condition, financial difficulties and family stress, to the effects of experiences of violence, including the grieving of incomprehensible losses.