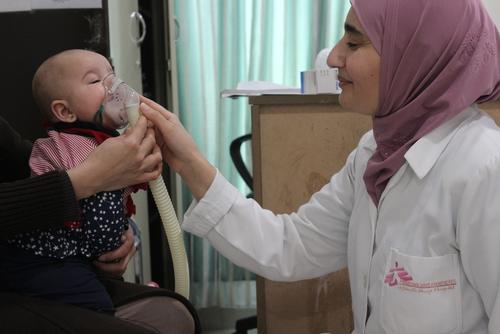
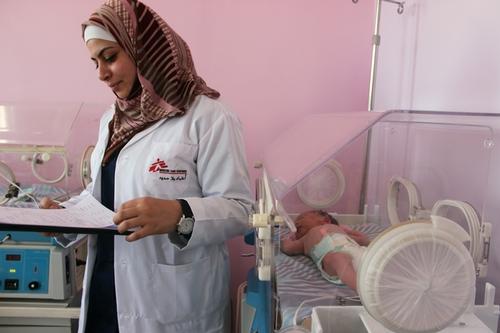
Amal Bani Khalaf, a Jordanian psychologist who has worked with MSF since 2014, gives an account of her work in MSF’s non-communicable diseases (NCD) project in Irbid, Jordan.
As her body drops into the chair in front of me – worn out, so slight – her quiet mask falls to reveal a deep sadness. How many tears she must have shed, I think to myself.
Slim, brunette, dressed in black (as the women of Daraa, a governorate in the south of Syria, usually are), she is in her early 40s but looks much older. After a long sigh, she says to me, “I have heard from my doctor here that you provide psychological support in individual sessions, in confidentiality...”
“Yes,” I answer, and give her a detailed explanation of the psychological support MSF provides, alongside other medical services, at our non-communicable diseases (NCD) clinic in Irbid.
This woman is one of many Syrian refugees we see dealing with mental health difficulties in addition to chronic disease. A life of displacement is painful, and even more so for those who have lost children to war.
We try to provide specialised support to patients of all ages and in all kinds of situationAmal Bani Khalaf, MSF psychologist
The mental health component of our NCD programme in Irbid includes individual and group counselling sessions aimed at providing psychosocial support at the highest level, in a private and confidential space.
In these sessions, we develop treatment plans together with the patient, and deal with symptoms of anxiety, depression, post-traumatic stress disorder or gender-based violence, and any other difficult situations they are facing.
We recently finished our first course of group counselling sessions for patients with symptoms of depression. By the seventh session, I had to prepare the group for ‘graduation’. The next session would be their last.
I still remember how they appeared on the first day: crying, pale, with no energy left in their bodies, eyes full of tears, hearts full of grief. Many had experienced enormous loss in Syria, survived violence, and continued to support their families in Irbid while struggling with poverty, loneliness, and painful memories.
In these final sessions, I noticed a change. I could see great hope in their eyes. All positive, or at least able to express negative feelings and deal with them in a positive way. One participant sang a song of love and enthusiasm, another smiled at stories of beautiful family mornings. One suggested planning a lunchtime gathering in a nearby garden after the group had closed, and another asked my manager, in English at break time, about the best cities in Canada for refugees, in terms of cost of living.
Over the course of these sessions, the group became a family that came together, in spite of other family commitments and transport difficulties, every Wednesday for over a month and a half, listening to each other’s stories, supporting one another, and sharing their concerns.
As a counsellor, my role was to offer supportive, appropriate activities that enabled each of the participants to express their feelings in a warm and safe atmosphere, to educate at times, and to suggest some simple homework to reinforce the work we did together and support their progress. When we closed the group, it was clear that they would remain a family.
With these sessions, we try to provide specialised support to patients of all ages and in all kinds of situation. We help them wipe away their tears and plant hope for a better future.
This is how we, the mental health team at MSF’s clinic in Irbid, are working to save lives, and improve the lives of our patients.