Children are particularly vulnerable to tuberculosis (TB). Unfortunately, diagnosing paediatric TB is complicated, and the exhausting treatment regimen children must undergo might be accompanied by bullying or feelings of loneliness. Adapted diagnostic methods and a comprehensive approach to treatment are needed to defeat the disease that is weakening children’s bodies.
Paediatric TB treatment and diagnosis are part of an innovative project in Tajikistan run by Médecins Sans Frontières (MSF) and the Tajik Ministry of Health and Social Protection.
TB is often un- or misdiagnosed in kids
“Children have different symptoms of tuberculosis than adults,” says Dr Zufliya Dusmatova, MSF medical doctor in Tajikistan. “The symptoms in children often resemble other diseases and therefore paediatricians might treat children for viruses or diseases, like a cold or bronchitis.”
“Children are usually not able to express what exactly hurts them and what problems are they suffering from,” says Dr Dusmatova. “It happens that a child has enlarged lymph nodes, loses weight and appetite but their parents don’t notice it.”

If tuberculosis is not diagnosed in time, it may progress rapidly and, in the worst cases, can result in death. Another issue is that TB often resides in other parts of the body than the lungs (such as in the intrathoracic lymph nodes) and therefore is undetectable by x-ray. A CT scan, that could discover such type of tuberculosis, is too expensive and isn’t used very often.
MSF, in cooperation with the Tajikistan Ministry of Health and Social Protection, are trying to overcome these barriers. Since 2011, we have run a programme focused on paediatric TB. We started with contact tracing in families and diagnosing children that were in contact with someone who contracted TB.
“In most cases, the children became infected by another family member,” says Dr Dusmatova. “When the children are small, they spend a lot of time with their parents or grandparents, who might have tuberculosis and infect the child.”
Tracing the path of an infectious disease
Contact tracing is an effective method to find ‘hidden’ cases. Whether owing to a lack of symptoms, health seeking behaviours, health education or because of stigma, latent TB, and particularly paediatric TB cases, may go undetected in the community.
Surayo is the mother of six-year-old Bibisoleha and eight-year-old Zainidin. Both kids have tuberculosis, but thanks to contact tracing, the kids were diagnosed and have now started treatment.
“I knew that my father was sick and because I was aware that the disease is transmissible, I left my children at my husband’s house,” says Surayo. “I was afraid they might get infected. After three months, I brought my children to my parents’ house, where I live.”
“Then MSF came and did X-rays and other tests,” continues Surayo. “When they told me that my children had the disease, I couldn’t believe that they were sick.”
Helping kids to help get correctly diagnosed
Our team also opened a specialised room for sputum induction. Sputum is a thick mucus that adults cough up when their lungs are diseased or damaged. Analysing sputum culture is considered the best way to diagnose TB.
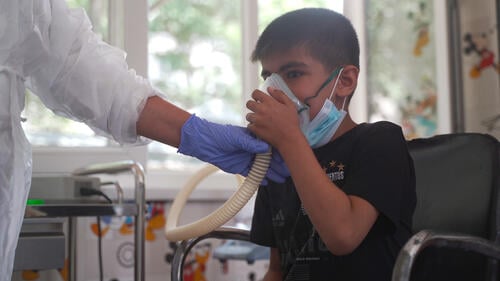
However, children have great difficulty in producing it themselves. Sputum induction uses a nebulizer machine through which the child inhales concentrated sa¬line solution, that leads to coughing and sputum production.
“We do the sputum induction for diagnosis and during the treatment to determine whether the child is infectious and has to stay in the hospital or is no longer infectious and can be treated at home,” explains Zamira Rakhmonova, an MSF nurse working at the Paediatric TB hospital in Dushanbe. “Once their sputum is clear and other test results such X-rays are good, they can go home and continue their treatment there.”
Families helping children to stay on treatment
“We moved most of the treatment to homes and families,” says Dr Dusmatova. “We call it family direct observation therapy, the F-DOT.”
“We visit families and explain to mothers or other caregivers what medicine their child needs, when they must take it and how to store it,” says Dr Dusmatova. “Before F-DOT, we had to convince the parents that their child must stay in the hospital, even if they were not infectious.”
“It was difficult because the hospital might be far away, and parents don’t always have money to go on a visit,” continues Dr Dusmatova. “Hospital is a hospital; no one wants to stay there for three or four months.”
As a part of this unique F-DOT programme, MSF teams provide usually monthly medical check-ups, but also medication, food and psychological support, that helps kids and their families to endure the treatment.

Fighting stigma surrounding TB
“It’s very confusing for children to understand what is occurring in their bodies,” says Tanya Morshed, MSF mental health activity manager in Tajikistan. “‘Why did they get it? What will happen to them?’ There is a lot of fear as well as stigma.”
“One of the medications may make a patient’s skin change colour and they may be bullied or harassed by some of their peers about it,” says Morshed. “If they are teenagers, especially female teenagers, it can affect their chances of getting married, because other families may say, ‘No, there is something wrong with this family. We don’t want them to bring tuberculosis to ours.’ So, all these issues can affect their future and can cause sadness, anxiety, stress, and isolation.”
Denial by others unfortunately occurs very often in Tajikistan.
“Some of my dearest friends accepted that I have tuberculosis, but others didn’t,” says Mahina, a 21-year-old who has multidrug-resistant TB. “They understood that I have bacteria, that might be transmitted, and they stopped talking to me. It hurt a little that they were my friends only when I was healthy.”
We started to use new regimens for children with MDR-TB containing new and repurposed drugs... Compared to the medicines we used before, it is a huge difference.Dr Zufliya Dusmatova, MSF medical doctor in Tajikistan
Fighting the stigma, misinformation and fears is another goal of the MSF project in Tajikistan. And through education of families, society is slowly changing.
“At the beginning, when our neighbours learned that my kids had tuberculosis, they didn’t let their children play with mine. They told their kids not to come here,” says Surayo. “But now, they understand that my kids are not infectious, and they play together. My kids themselves tell others that they are taking drugs.”
Changing paediatric TB treatment for the better
Children with tuberculosis need to take multiple pills every day. Fortunately, there has been huge development, especially in treatment of complicated forms of TB such as multidrug-resistant TB (MDR-TB).
In 2017, MSF developed a Guidance for the Diagnosis and Treatment of Tuberculosis in Children of the Republic of Tajikistan that recommends shorter treatment regimens with newer drugs delamanid and bedaquiline.
The guidelines, developed by MSF, were adopted by the Tajik Ministry of Health, and the country became one of only two countries so far in the Eastern Europe and Central Asia region to include World Health Organization (WHO) recommendations in their national guidelines.
“We started to use new regimens for children with MDR-TB containing new and repurposed drugs, such as bedaquiline, delamanid or clofazimine, and we were observing how effective they were,” says Dr Dusmatova. “All of them had good results and no major side effects.”
“Compared to the medicines we used before, it is a huge difference,” says Dr Dusmatova. “Before, the children had to get injections that were painful and had serious side effects, such as loss of hearing.”
“Other medicines caused nausea, vomiting or diarrhoea,” continues Dr Dusmatova. “Newly recommended drugs by the World Health Organization don’t have these side effects or only to a very small extent.”
“My work at MSF helped to change my opinion on paediatric tuberculosis – on the treatment and patient care. Now I know that it is important to do the contact tracing and treat children at home,” says Dr Dusmatova. “Since MSF started to work here, I see an incredible amount of progress. It is a unique project in this region because we started to treat and diagnose specifically children.”









