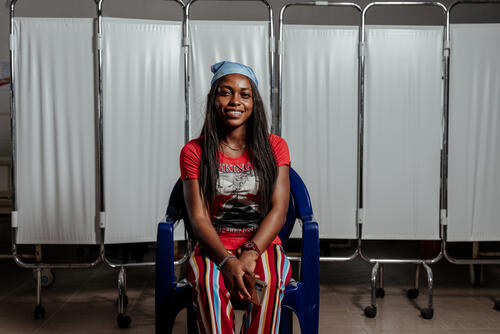
“Everything felt strange,” says 14-year-old Nneoma Okonogha, who was treated for Lassa fever – a virus transmitted to humans through contact with food or household items that have been contaminated by rodents. “I thought I was really in a nightmare.”
Once a person is ill with Lassa fever, they can pass it on to others should they come into contact with the infected person's body fluids. Nneoma, along with her sister, Ukamaka and their mother, Priscilla, caught the viral haemorrhagic fever at the same time. All three of them were treated at the Alex Ekweme University Teaching Hospital in Abakiliki (AE-FUTHA), Ebonyi State, Nigeria.
“It was so severe that when the children were shouting in pain, I couldn’t help them because I was also down with pain,” says Priscilla, who also works at the hospital as a civil servant.

Lassa fever - Nigeria
In Nigeria, Lassa fever is endemic – cases are found and reported almost every year. During a severe outbreak in 2018, more than 600 people were confirmed to be infected, and 171 people died.
In March 2018, Médecins Sans Frontières (MSF) started supporting the Lassa treatment centre at AE-FUTHA. Since then, our teams have been working closely with the Ministry of Health (MoH) to treat patients suffering from Lassa fever.
The treatment has proven pertinent for the community, with over 15 patients treated for Lassa fever at the Abakaliki project in the first month of 2022 alone. Across Nigeria, there have been a total of 115 confirmed cases and 26 deaths throughout 30 local government areas in 11 states of the country.
“I contracted Lassa fever in February 2021. When I tested positive, I was shocked,” says Anastasia, a Lassa survivor from Abakaliki. “It came like malaria, and I bought anti-malaria drugs from a pharmacy. When I took it for three days, I was still sick. In fact, my situation was worse.”
Anastasia had Lassa fever, but thankfully she was able to access the anti-viral treatment she needed to recover. However, her first assumption that she had malaria is a common one.
Lassa fever symptoms are very similar to malaria, making it difficult to diagnose. Many medical staff don’t have specific training on the detection and treatment of Lassa. As a result, patients often only receive an accurate diagnosis once they are at a severe stage of the disease, which is more challenging to treat.
Lassa fever is a serious disease. But when the medical community and the communities are fully engaged and empowered with accurate information [...] we can get people timely access to care and they can recover more quickly.Luigi Sportelli, MSF project medical referent
Since we started working to treat Lassa fever in Ebonyi state, our aim has been to tackle the root causes of Lassa fever and its large impact on infected people. A key trial of rapid diagnostic tests (RDT) for Lassa fever is currently underway at AE-FUTHA. If an RDT proves effective, it could help drastically reduce the waiting time for laboratory test results.
“We want to see if an RDT could be a substitute in treating or diagnosing Lassa fever,” says Dr Okereke Michael Uche, MSF medical doctor. “Timing is important; a patient moves from a mild condition to severe. And when it becomes severe, it is more difficult to manage.”
Stigma can be a heavy burden on Lassa fever patients. Some people have lost their jobs, been chased out of their own community, or even lost relationships because they were associated with Lassa fever, either as a patient or a caregiver.

We work to educate communities through a team of health promotors. The team organises community meetings, health talks and awareness campaigns in villages and rural areas across seven local government areas in Ebonyi state.
“The purpose of all this is to foster behavioural change,” says Benjamin Uzoma, MSF health promotion supervisor. “We talk to people one at a time to ensure that everybody gets the message and understands the causes and cures for Lassa.”
“Lassa fever is a serious disease,” says Luigi Sportelli, MSF project medical referent. “But when the medical community and the communities are fully engaged and empowered with accurate information, then not only is the stigma reduced – but we can get people timely access to care and they can recover more quickly.”
To ensure continued progress in the fight against Lassa fever, our teams keep a continuous provision of drugs, lab supplies, and personal protective equipment (PPE). We also train AE-FUTHA staff on clinical management and Infection Prevention Control (IPC) for Lassa fever. And to alleviate the psychological impact of the viral disease on infected or suspected patients and their families, mental health support is also provided.