What’s your point of view on what is happening in Syria?
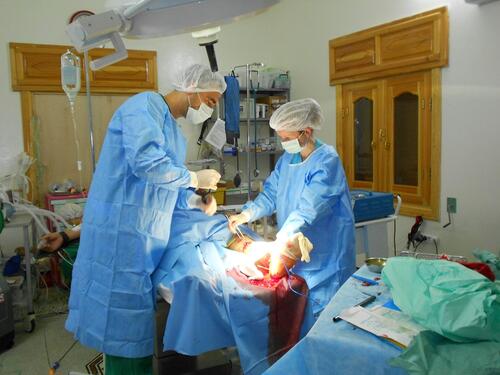
Brian Moller is an anaesthetic nurse. He has been working with Médecins Sans Frontières (MSF) for nine years and is today an emergency coordinator. This July, Brian managed the surgical hospital set up by MSF in Syria.
We’re working in a rebel enclave and thus only have a partial view on the entire situation. It’s a war though – one that doesn’t spare civilians. Some are targeted by snipers and others are victims of “collateral damage”, as they say. Whereas regular army troops were confronting demonstrators in the past, they’re now clashing with armed opposition groups, mostly in urban centres. From what we are seeing, these groups are varied, made up of people with different social backgrounds and grievances. The only thing that they all seem to have in common is their anger towards the Syrian regime.
As an NGO, isn’t it complicated to be working on one side of the conflict?
As we don’t have official authorisation to work in the country, we don’t have a choice. Our work consists of coming to the aid of those who don’t have access to healthcare. The supporters of the regime can access public hospitals, but many of the rebels and their supporters are deprived of this access and assistance. We also explain to people that the causes of this violence are less important to us than its consequences from a medical point of view. And though we are working in rebel territory, we insist upon the fact that we make no distinction between supporters and opponents of the regime in administering care. Our position is relatively well understood from an intellectual standpoint by the health professionals and Syrians we meet. It’s not as well understood from an emotional point of view. Since the beginning of the Syrian uprising, many have had people close to them get injured or killed.
How are Syrian health professionals dealing with the situation?
Their availability and willingness to help each other out is impressive, given the context. They are not experienced or prepared for such an influx of patients, or for treating these types of injuries. Our team’s experience in this regard reinforces the abilities of the local staff, who are seeing this kind of violence for the first time. We’re dealing with it, and we’re even getting good results in spite of the difficulties and ethical dilemmas that arise. For example: what are the priorities? When can one say that there’s nothing more that can be done for a patient? When does one stop aggressive therapy? There are many questions that create tensions and heated exchanges between staff confronted with the demands of rationality in an extremely emotional situation.
What are health and medical services like in the region you’re working in?
There are dispensaries, pharmacies and places where consultations are carried out, but there is no capacity for surgery and hospitalisation in this area. Further afield, hospitals that are able to operate on people refer them to us so that we can hospitalise them post intervention.
Getting medical supplies and medicines is also a problem. Blood, painkillers, anaesthetics - they’re short on everything. Along with access to water, electricity and communication networks, these problems of availability, transport and supply are particularly acute, though they pose a problem in all conflicts. On our side, we are succeeding thanks to a group of Syrian doctors and the efforts of our logisticians in maintaining a buffer stock that permits us to hold out two weeks in case of any major problems. We are also getting private donations, which attests to the solidarity of the people around here. A few days ago, some women from the village arrived with two big bags full of medical and dressing supplies and medicines purchased from the local pharmacies. Where these products came from originally is hard to verify; for example, if you don’t know where anaesthetics drugs came from, can you use them? The problem in a context of war is that you don’t always have the choice.