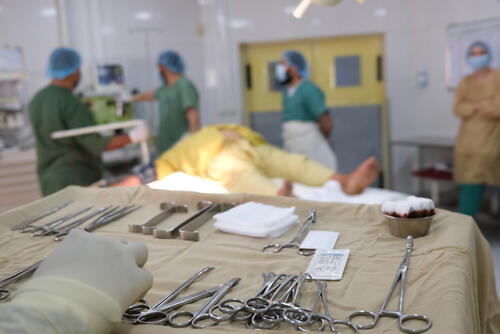
The healthcare system in Afghanistan is ill-adapted to the challenges faced by the Afghan people, according to a report released today by Médecins Sans Frontières (MSF).
The report, The Continued Struggle to Access Medical Care in Afghanistan, brings together medical data, interviews and questionnaires from patients, their caretakers and staff in MSF’s projects in Helmand, Herat, Kandahar and Khost provinces. It clearly shows a healthcare system that is failing the population, and echoes the findings of previous MSF reports released in 2014 and 2020.
Over the years, MSF has continued to expose the discrepancy between the promises of the donor-promoted model of public healthcare delivery and the reality on the ground. “Poorly functioning health facilities, unaffordable costs, and patients who undertake long and dangerous journeys. These all reduce people’s ability to access timely medical care,” says Filipe Ribiero, MSF Afghanistan country representative.
Last year, international donors cut funding for services in Afghanistan increasing pressure on an already fragile public health system and on health partners. The emphasis needs to be on Afghans receiving quality treatment closer to home, in line with their needs and financial circumstances.
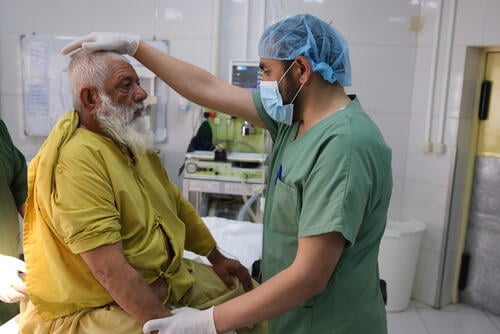
Patients described weighing up a range of factors before seeking medical care. Over 80 per cent of those surveyed said they had experienced financial difficulties as a result of spending on healthcare. And the socioeconomic effects of the COVID-19 pandemic have only made things worse.
“We live in the desert with no access to healthcare. And there are economic issues,” says a male caretaker in Boost hospital, Helmand province. “Some people can’t find the money to get help even if they have a patient at home; they wait for God to do something.”
When people find the money needed either for transport and/or the cost of medical care, and successfully reach the clinic or hospital, the challenge is not over though. Among all surveyed patients who visited a public health facility in the last year, 45 per cent said they were not satisfied with the services provided.
Many Afghans go to private clinics or hospitals, where they face costs they can barely afford and whose quality is far from guaranteed; some favour local solutions such as traditional remedies; and others travel long distances to reach free medical facilities supported or run by organisations like MSF.
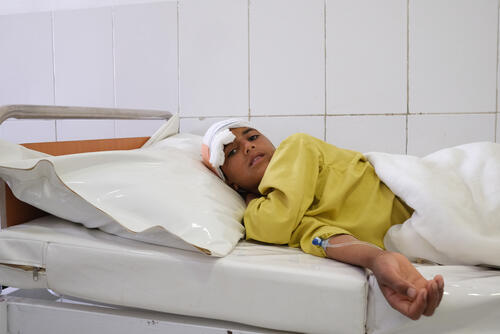
But beyond financial costs, travelling to heath facilities is fraught with danger due to active fighting, the presence of explosive devices and the threat of robbery on the roads. These obstacles lead to people delaying or taking more circuitous routes, meaning health conditions can deteriorate by the time they arrive for treatment.
When there was heavy fighting around Lashkar Gah city in early May, one mother described how she was left with little choice but to brave the violence to seek healthcare for her son who had had fever and diarrhoea for over a week: “We thought he might die, so we had to take him to hospital. We left in the morning when the sun was rising. We came a very difficult way and crossed a river. Our motorcycle stopped working so we left it. It was a war, there were bullets in the air. There were so many obstacles.” A journey that should have taken 30 minutes took five hours.
“We are under no illusions about our ability to respond to the overwhelming needs in the country, but we do our best,” says Ribeiro. “Donors and policymakers need to take an honest look at the shortcomings of the current model of healthcare delivery in Afghanistan and work to make quality care available, accessible and affordable to everyone”.
MSF has worked in Afghanistan since 1980 and today runs five projects in five provinces: Helmand, Herat, Kandahar, Khost and Kunduz. In 2020, MSF teams provided 112,453 emergency room consultations, assisted 37,898 deliveries and undertook 5,669 major surgical interventions. MSF provides medical care free of charge. It relies solely on private funding for its work in Afghanistan and does not accept money from any government.