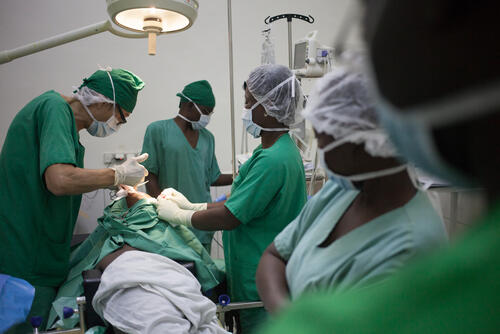
Olga* describes what happened in a trembling voice: "Yesterday afternoon I left home to go and look for a bit of yucca [plant] in a field near the airport. On my way there, two men armed with machetes intercepted me and told me to sit down. One covered my eyes and the other began to undress me.”
That is how her story begins. It could be that of almost any of the thousands of people who suffer sexual assault in Bangui, the capital of the Central African Republic (CAR). Last year, Médecins Sans Frontières (MSF) assisted 4,000 victims of sexual violence across the country. Our team at Bangui community hospital have treated more than 800 people in the first half of this year alone.
In CAR, as in many other countries, sexual violence is a taboo subject. In many cases of sexual assault, the victims are forbidden from talking about it due to the shame it will bring on their family. Some of the local languages don’t even have a specific word for rape.
"I thought about committing suicide several times. I felt ashamed when I walked down the street and I thought everyone was looking at me. I can’t sleep at night,” said Olga, 41, when explaining her situation to an MSF psychologist working in Bangui, through a project known as Tongolo, meaning ‘star’ in the Sango language.

Sexual violence in the Central African Republic
A cloak of silence
The long conflict in the country and the presence of armed men on almost any corner provide fertile ground for sexual violence. "But here, many sexual assaults are committed between neighbours or within the family,” says Beatriz García, coordinator of the Tongolo project. “And in most cases the problem is resolved amicably in the community or between family members to avoid bringing shame upon the families, forgetting that this is a medical emergency that must be taken care of."
In order to give the community access to treatment, MSF has extended its Bangui community hospital project to the outskirts of the city, opening a new support service in the district of Bédé-Combattant.
"We are sure that this will allow victims to arrive in less than 72 hours, which is key to mitigating the possible consequences of the assault,” Beatriz explains. Olga showed up at the new MSF service 24 hours after she had been assaulted and was prescribed prophylaxis to protect her from sexually transmitted infections, such as HIV.
I’d been carrying a weight on my shoulders for six years. I hadn’t told anyone what had happened to meMartine*, a widow and mother of three, receiving weekly psychological consultations with MSF in Bangui
A feeling of relief
Martine* is a 53-year-old widow with three children. She seems relaxed as she leaves a psychological consultation at the centre in Bédé-Combattant. “I feel relieved. I’d been carrying a weight on my shoulders for six years. I hadn’t told anyone what had happened to me, but then some people told me that I had no reason to feel afraid or ashamed. And here I am,” she says.
"During the fighting in 2013, I took refuge in the forest. There, two armed men took me by force and raped me. I then had intense pains in my groin, I felt dirty and I was terrified of meeting other armed men,” she explains, without losing her composure. Martine will now have a free weekly consultation through the MSF mental health service.
There remains a gap in assistance services for victims of sexual violence in Bangui. Beyond the medical services offered by MSF, there is no legal or socioeconomic support available to victims to help them overcome the consequences and challenges of the aggressions they have suffered.
It is essential to make this problem visible in order to attract the attention of donors, authorities and humanitarian agencies. The unmet needs of victims of sexual violence remain huge.
Thanks in part to a number of awareness campaigns, people are beginning to realise the scale of the problem, with many victims, like Martine, turning to MSF’s services a long time, even years, after the incident. The project is open to the entire population but places special emphasis on treating children and men, because their cases are even less visible and tend to be more complex.
“In CAR, there are many men who have suffered sexual assault but who are too scared to speak up. Hardly any of them come to our treatment centres. They are reluctant to ask for help. There is huge pressure in the community, with very violent stigmatisation,” the project coordinator, Beatriz, explains.
*Patients’ names changed