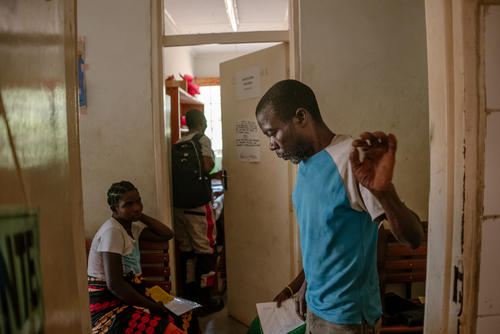When Thongsei Lupho, 44, first started feeling unwell, he suspected he had contracted tuberculosis (TB). He visited Médecins Sans Frontières’ (MSF) clinic in Moreh, on the India-Myanmar border, where was diagnosed with HIV.
Lupho had used drugs in the past to gain social acceptance in an area where tribal tensions had fostered a lack of trust amongst people. Having put his drug use behind him once he married, his diagnosis came as a shock.

At first, he was afraid of discrimination and felt unable to mingle with others in public. He also worried about his children, some of whom were also diagnosed with HIV. His eldest daughter feels ashamed of her diagnosis and hides it from her friends and classmates.
Intravenous drug use is not uncommon in Manipur and, according to the Manipur State Aids Society, it has contributed significantly to the spread of HIV and hepatitis C in India’s northeastern states.
Tuberculosis is likewise highly prevalent but in Manipur, which has experienced years of low-intensity conflict, state infrastructure has been unable to cope with the high number of HIV-positive and TB patients, particularly people with drug-resistant TB (DR-TB). This can have dire outcomes: in cases of co-infection, each disease speeds up the progress of the other, making the patient more vulnerable and their treatment more difficult.

MSF started providing specialised care for HIV and TB in Manipur in 2005 and 2007, respectively. At our three clinics in Chakpikarong, Churachandpur and Moreh, we provide screening, diagnosis and treatment for HIV, TB, hepatitis C and co-infections of the three diseases.
We are the only international NGO in Manipur treating the three diseases and have a patient-focused model of care at the heart of our operations in order to improve outcomes and minimise the spread of the diseases.
“One of the simple ways we’ve tried to reduce the spread of drug-resistant strains of tuberculosis is to bring care to the patient instead of making them come to us,” says Edoardo Nicolotti, MSF Project Coordinator. “When someone is newly diagnosed, we visit them at home to carry out an infection prevention and control assessment.”
“If they live with family, we offer to build a simple house for them near the family house,” says Nicolotti. “This greatly minimises the risk of transmission to others but keeps the patient close enough to maintain normal family interaction.”
MSF has built nine such houses during 2018 and 2019. We also send a nurse to the patient’s house every day to carry out tests and ensure they are adhering to their treatment, which involves a challenging cocktail of drugs to be taken over roughly two years.
Since DR-TB medication causes significant side effects, making it difficult for patients to complete treatment, MSF also provides counselling to encourage better outcomes.

Along with treating partners of co-infected patients, we also treat mono-infected hepatitis C patients at an opioid substitution therapy centre in Churachandpur. At the same clinic, people who inject drugs can pick up clean needles and turn in their used ones, helping to reduce the risk of needle-sharing and further infection. We support the district hospital in Churachandpur by treating people living with HIV for hepatitis C.
Since January 2019, 120 new people were started on antiretroviral drugs to treat HIV; 36 HIV-hepatitis C co-infected patients are being treated for hepatitis C, and 133 patients were started on treatment for drug-sensitive or drug-resistant TB.
In 2018, MSF started using a new drug, bedaquiline, in the treatment of patients with drug-resistant forms of TB. Currently, three multidrug-resistant TB patients are on new, shorter treatment regimens using the newest drugs bedaquiline and delamanid, with the remaining patients on the two-year regimen.