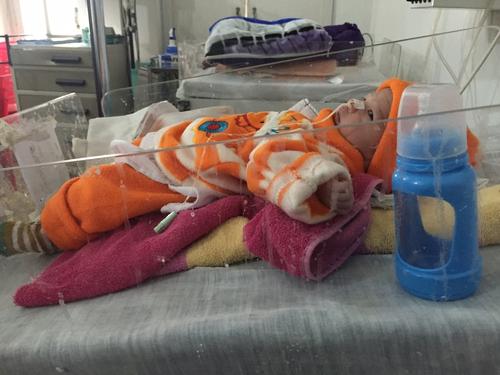
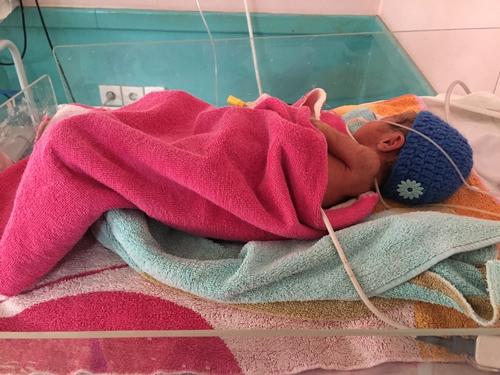
Although born and trained in Pakistan, Dr Anokhi Ali Khan had never worked there until she joined Médecins Sans Frontières (MSF). A paediatrician, Dr Khan has been treating newborns and strengthening staff skills as part of the MSF team in Peshawar women’s hospital in northeastern Pakistan. The hospital celebrated its fifth anniversary in May 2016. As Dr Khan explains, the experience has been eye-opening.
I arrived at the end of February 2016. I actually studied medicine here. I’m Pakistani-Swiss, and live in London. Yet I never thought MSF would send me to Pakistan. But more than interesting, it’s been quite eye-opening. Of course I was hoping to see a new place and have a new experience at the same time as offering my expertise. On the other hand, I know the culture, the language, so I can understand it is an advantage to have me here.
I’m from Karachi, the south of the country, which is a very different world, even though it is still Pakistan. If anyone had said while I was living in Pakistan “Let’s go to Peshawar”, I would have said “Why would you want me to go there?” But when you drive up from Islamabad, up in to the mountains, it is absolutely breathtaking. Peshawar also reminds me of the interior of Sindh where I used to go every second weekend for a picnic, and people would be wonderfully open. In Karachi, it is a metropolis and people are busy, like in New York, London or Zurich. But in Peshawar people are incredibly hospitable, and all very hardworking.
I studied pediatrics in Switzerland and then took a Masters in Public Health, followed by my PhD in Epidemiology in London. Then I went back into clinics in order to give me a bit more clinical exposure. I had been wanting to join MSF my entire life. I wanted to do paediatrics at a global scale, not just sitting in one place. I wanted to complete my training, do everything in chronological order, to dedicate my life to medical humanitarian work.
The Peshawar women’s hospital is not what I generally assumed MSF does, because I knew we have really good hospitals in Pakistan. But very soon, I started to understand what our target population is and how we are trying to reach them in the surrounding areas – for example in FATA, the Federally Administered Tribal Areas. It is absolutely brilliant that we can offer healthcare, especially when you have patients who come from regions where they have poor access. The neonates wouldn’t get that level of care in other hospitals – one reason being the government hospitals are overwhelmed with patients beyond capacity.
Some families, for whatever reason, feel pressure to take their child home as soon as possible, so if we assess a need to keep a baby for a longer period, we take the time explaining to the parents the reasons why, including the significance of the illness. This often well received by parents and family members.
Most of the babies here have infections. What we see in the newborn unit are obviously the sickest cases; the mothers we receive have had high-risk pregnancies or complicated deliveries. The most common condition in their babies is sepsis. Neonatal sepsis is a severe infection and is one of the top three killers of newborns worldwide.
In the first 72 hours, if the child gets a bacterial infection, it has very likely been transmitted from the mother. However, these children don’t necessarily present symptoms in the first day. So, we assess them for risk of infection under our guidelines and if the risk is there we tend to treat immediately with antibiotics. This is done keeping in mind the fact that once the baby has returned home, he or she could deteriorate very quickly, and it might not be easy for the mother to seek further care.
It has been a good first placement. My predecessor had done a very good job, and I wasn’t being ‘thrown in the deep end’. One of the roles of international staff like me is to supervise standards of care. During the most recent emergency we had, the maternity nurse came running in with a pre-term baby (an unexpected arrival at our gates) requiring CPR; we started CPR and everybody knew what to do. It was lovely how everyone worked together so well.