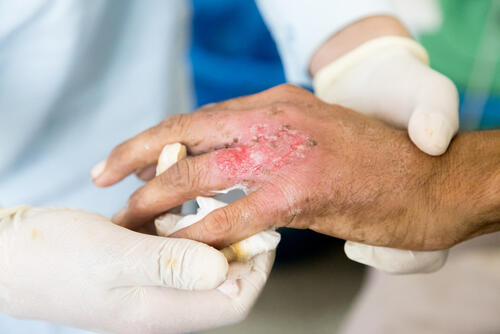
Amy Le Compte is a midwife from Gisborne in New Zealand. She has just returned from a six-month assignment in MSF Women's Hospital in Peshawar, in the north of Pakistan where, along with daily maternity work, she supported the launch of a new community outreach program to enable access to quality maternity care for poor and marginalised populations.
“Peshawar is a huge city with a total population of around 3 to 4 million inhabitants. There are several health facilities but MSF Women's Hospital focuses on the most marginalised or poorest populations. To further facilitate access to our hospital for these groups of people in particular, we have an outreach program that has recently been expanded to access a much wider area of people in need. The region that we’re working in is close to the Federally Administered Tribal Areas (FATA), where the health facilities are very poor due to ongoing conflict over the past years. Within Peshawar city and the surrounding district there are lots of internally displaced people and many refugees from Afghanistan, and most of them don’t have access to maternity care because they can’t afford it, because it’s unsafe to travel or because they simply don’t know the service exists.
So we have been going into the Basic Health Units (BHUs) around Peshawar to inform them about what we are doing, who we are, that our medical services are free. We also cover the cost of transport to facilitate the referral of women by the Basic Health Units to our maternity service.
For the last three months, for the same programme, I (with the support of the MSF team) have also started providing training to the Basic Health Units staff on High Risk Obstetrics and Maternity Care, because decentralisation of good-quality care to the communities is essential for mother and child health. BHU staff travel to our hospital once a month, for three days worth of training that is provided by senior national staff members and overseen by the international medical staff. The training includes lectures in two of the local languages plus English, case presentations, scenario sessions and time spent learning in the wards. We also do educational sessions on the importance of safe and appropriate antenatal care for the health of the baby and the mother.
We had around 100 deliveries a week
It’s been a very intense assignment for me and an extremely interesting experience in mixing roles, between training personnel, managing staff in our hospital, and providing medical care myself. And it was also very rewarding. The Pakistani staff are doing a fantastic job. They are all well trained with good medical skills. Life is not always easy for them in this country and they have strong characters. Discussing the cases has sometimes been quite challenging. As a young midwife I may have needed more time to be fully accepted than if I had been say an older or male doctor. But this is just one of the many cultural differences that you have to learn to work around in many countries.
We make up about 150 employees from the director to the cleaner, including nine international staff. We have four full-time female gynaecologists, and five medical officers. With around a 100 deliveries per week we were often close to over-capacity. We have an operating theatre with Pakistani anaesthetists and obstetricians, so we can take care of women in need of a caesarean to secure a safe delivery.
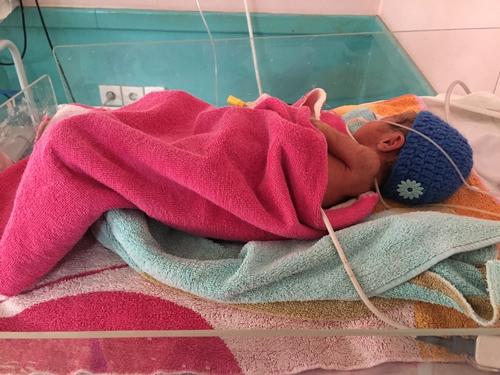
We were facing many challenges in regards to the frequent use of several dangerous drugs that mothers-to-be can get without medical prescription in Peshawar. This causes a lot of mishandling of cases during pregnancy, lots of premature babies, obstructed labours and many multiple births. Once (and this was my worst experience), we had quadruplets that we simply couldn’t save. They were less than 30 weeks old, and the labour had been started with a drug called oxytocin -- because of irregular antenatal care we don’t always know the age of the foetus -- but they were too small to survive. Instead of four births that day, the family was going to go through four painful and possibly avoidable deaths.
Lots of multiple and premature deliveries
In these countries, because of the social and sanitary situation, deaths and disabilities are more common and somehow more accepted than in more wealthy countries. Child mortality is higher and women have many more children.
Fortunately these cases are balanced out with a number of wonderful stories. One day, a woman arrived from Hangu, in the FATA area after a four hour-long drive. She had been referred by the MSF hospital there for "twins". She had already had four children, and when she arrived with her husband and her mother-in-law she was extremely tired, dehydrated and in early pre-term labour. After two weeks, thanks to our ultrasound machine, some specialised medication and the skill of our staff, we were able to plan a safe vaginal delivery and she gave birth to not two but three small but healthy babies from 1.5 to 1.7 kg, two boys and a girl. They stayed in our neonatal unit for another three weeks before finally being able to go home“.