After more than two months of the war, Israel’s unrelenting, indiscriminate strikes on Gaza, Palestine, have turned the north of the Strip into a pile of rubble and are now pounding the Middle Area and the south with increasing brutality. The suffering of Palestinians trapped in Gaza can no longer be put into words.
With nearly the entire 2.2 million people of Gaza now cornered in the south of the Strip, the Israeli forces' strikes on what was supposed to be a safe zone prove that nowhere is safe.
Nearly 19,000 people have been killed and over 50,000 have been injured over the past 10 weeks in Gaza according to the Ministry of Health, and the ongoing offensive continues to create hundreds, if not thousands, of new casualties each day.
Doctors are stepping over bodies of dead children to treat other children who will die anyway.Chris Hook, MSF medical team leader in Gaza
Challenges of treating war-wounded in Gaza
In Nasser hospital in Khan Younis, in the south of Gaza, where Médecins Sans Frontières (MSF) works, the dead and wounded have been arriving en masse almost every day since the end of the short-lived truce on 1 December.
The severity of their injuries and the sheer number of patients are pushing Gaza’s healthcare system to a breaking point even in this part of the Strip, after its collapse in the north, where according to the WHO only one hospital is still partly functioning.
“The emergency department at Nasser hospital is completely full and new patients are being treated on the floor,” says Chris Hook, MSF medical team leader in Gaza.
“Doctors are stepping over bodies of dead children to treat other children who will die anyway,” he says.
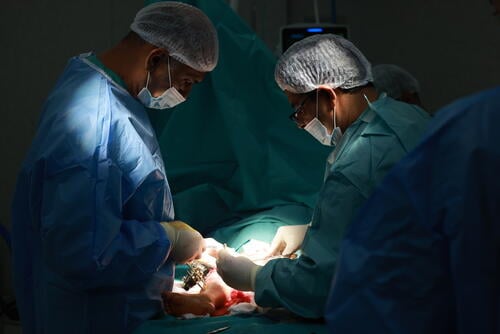
“More and more temporary structures are being erected, tents are used as wards and temporary clinics. Every spare building is being filled with beds for patients. More hospital beds are desperately needed,” says Hook.
Treating the war-wounded is complicated as blasts from explosive weapons and collapsing buildings create multiple, simultaneous injuries on many parts of the body. In Gaza, Israel’s complete siege makes it impossible to access essential drugs, including pain management drugs, which are critical in surgical interventions, and the medical tools needed to repair shattered and burned bodies.
“The lucky few that survive have life-changing injuries. Many injured people suffer from extreme burns, major fractures that won’t heal properly and may go on to require amputations,” says Hook.
“Many of these patients, even if they can get back to something resembling normal life, will have severe chronic pain that will require substantial pain management as well.
“It would be a huge burden even on the most functional healthcare system, let alone for a system under intense pressure, like in Gaza.”

In Al Aqsa hospital, in Gaza’s Middle Area, our teams have been providing emergency surgery and outpatient care. From 1 December to 11 December, approximately one in three patients (640 over 2,058) have been announced dead on arrival.
On 6 December, the number of people killed arriving at Al-Aqsa hospital surpassed the number of injured. The hospital staff strive to maintain effective hygiene protocols and lower the risk of infection for patients while facing a lack of essential supplies and equipment. This is a remarkably difficult task, yet a critical one, as a soaring number of infections can quickly turn into an additional medical challenge for both the patients and the overwhelmed health workers.
What happens in the south of Gaza today seems to echo the approach followed by the Israeli forces in the north of the Strip. A scorched-earth policy that leaves no safe space for people, constant attacks and repeated evacuation orders given by the Israeli forces to entire neighbourhoods, and the total siege imposed on the Strip have made it extremely hard for people to access healthcare, and for medical staff to provide it.
Since 1 December, we've had to suspend our support to three health clinics in the south and reduce our presence in Nasser hospital. An end to the continuing displacement of people is imperative to allow the sick and the wounded to receive the care they urgently need.
The general conditions for most of these people are appalling: they live in temporary structures made of a few pieces of wood banged together and covered in plastic sheeting.Chris Hook, MSF medical team leader in Gaza
Infections peak as the healthcare system reaches breaking point
While the risk of violent attacks for civilians in Gaza persists, infections resulting from poorly treated wounds are rising fast, putting lives at risk.
“The risks of infection are incredibly high because of the conditions that people have to live in and the fact that there just isn’t the ability to provide the long-term in-hospital care that these patients truly need,” says Hook.
In the European hospital, an MSF medical team recently started treating patients who were injured at the beginning of the war and whose wounds have now become infected due to the lack of healthcare.
There are only a few general healthcare facilities, including Al-Shaboura clinic, which is supported by MSF, currently open in the south. This means there is limited treatment available for infectious diseases like respiratory infections, diarrhoea, chicken pox, lice and scabies, which spread uncontrollably in overcrowded shelters, adding to the risks for displaced Palestinians.

Appalling living conditions and widespread hunger
“As you go through the streets south of Khan Younis and near Rafah, you see the temporary shelters expanding further and further as more and more people arrive,” says Hook.
“The general conditions for most of these people are appalling: they live in temporary structures made of a few pieces of wood banged together and covered in plastic sheeting. They struggle to find enough water to meet their hygiene needs.”
The flimsy shelters are now constantly struggling, battered by the strong winds and heavy rain. With more people arriving in the south, food is becoming harder to find and the little food that is available is too expensive for people to buy,” he says.
During a seven-day truce in November, Nasser hospital had a brief respite from receiving patients with violent injuries and was instead overwhelmed with diabetic and other chronic patients who were not able to access the medical care they needed during the fighting.
This changed again when hostilities resumed on 1 December. This time with even greater intensity. We don’t know what has become of those chronic patients once our facilities were overwhelmed by mass arrivals of the war-wounded, nor how they will be able to survive.
On 17 December, the maternity ward of Nasser hospital came under fire. One patient was killed, while others were wounded in this attack. Attacks on healthcare must stop now.






