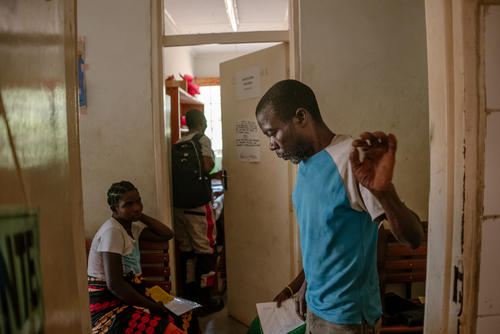A couple who contracted multidrug-resistant tuberculosis (MDR-TB) after being displaced by armed conflict has been cured at a clinic run by Médecins Sans Frontières (MSF) in Shan state, Myanmar.
It is the first time since 2015 that the clinic has successfully treated patients with the disease. The couple spent nearly two years away from their children and home during their treatment. Their story illustrates the difficulties patients in Myanmar’s conflict-affected communities face, and the scarcity of specialised treatment for patients in rural areas.
Myanmar’s Shan state has long been dogged by conflict between the armed forces (Tatmadaw) and non-state ethnic armed groups, as well as fighting between ethnic armed groups. Renewed fighting since mid-August 2019 has killed civilians and resulted in short-term displacement of approximately 8,000 people.
In September, MSF’s team in northern Shan was able to carry out a distribution of non-food items to hundreds of families in a new displacement camp, but many areas remain inaccessible to humanitarian organisations. For patients needing specialised medical care, displacement disrupts treatment, which can have devastating consequences on their health.
In 2017, Aik Jong and Aye Htwe were displaced from their home in Namhsan Township and detained in a crowded monastery for five days. The couple had been receiving antiretroviral medication from MSF since 2013 but weren’t allowed to take it during their period of detention.

A difficult but necessary separation
After their release, Aik Jong and Aye Htwe sought refuge elsewhere, and Aye Htwe noticed she was losing weight. The couple travelled to MSF’s clinic in Lashio, where both tested positive for MDR-TB. Due to a lack of locally available specialised treatment, they were unable to return home.
Treatment for MDR-TB is essential and lifesaving. But it is gruelling and many patients drop out. Curing patients is relatively rare.
The treatment lasts almost two years and has considerable side effects, which include nausea, vomiting, dizziness, hearing damage and loss of renal function. Patients have to take a daily cocktail of oral medication, and for the first six months, undergo painful injections six days a week.
Those living in more remote areas do not have treatment options close by, and may be forced to leave their homes, their jobs and their families in search of treatment.Mitchell Sangma, MSF medical coordinator
To minimise the risk of spreading the infection, MSF patients with MDR-TB are encouraged to live apart from others, with limited visits from family and friends during their treatment. While Aik Jong and Aye Htwe stayed in the MSF MDR-TB house in Lashio, where MSF also paid their living expenses, their three children stayed with relatives.
“At first the treatment was really hard but the medical staff supported us,” says Aye Htwe. “We didn’t need a lot of motivation. We knew the treatment would be hard, but we were determined – we had to do it for our kids.”
Although Aik Jong and Aye Htwe are cured, they are still struggling to reunite their family and to return to their village where they once worked as farmers.
“I’m happy to be cured of MDR-TB. I just feel like a huge burden has been lifted,” says Aik Jong.
Now he has other worries. “I don’t know when we’ll see our children again. It’s too expensive for us to make the journey to see them right now,” he says.

The need for treatment closer to home
The social and emotional upheaval Aik Jong and Aye Htwe experienced might have been reduced if treatment had been available closer to home. Myanmar’s Ministry of Health and Sports has, in principle, committed to decentralising treatment for MDR-TB to the district level, providing treatment along with primary healthcare. This has not yet been implemented.
“A lack of resources and diagnostic equipment continue to keep nearby care out of reach for many,” says Mitchell Sangma, MSF medical coordinator.
“This means that those living in more remote areas do not have treatment options close by, and may be forced to leave their homes, their jobs and their families in search of treatment.”
Given the lack of decentralised MDR-TB care, MSF has been providing treatment in Kachin, Shan, and Yangon, and has cured 228 MDR-TB patients in Myanmar.