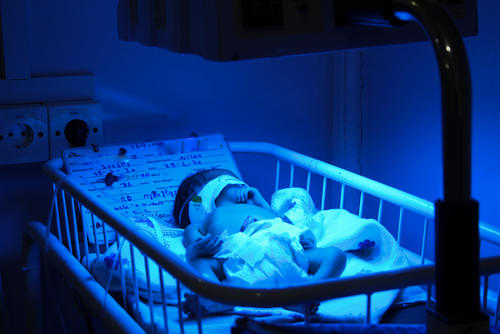
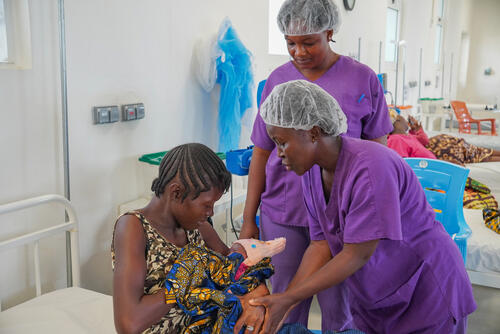
After Gulnaz started having labour pains in the 31st week of her pregnancy, she knew she would have to make the two-hour journey to Timergara district headquarters hospital, in northwestern Pakistan, where Médecins Sans Frontières (MSF) provides care for mothers and newborn babies.
Gulnaz explained that, with medical facilities in her area closed as part of the lockdown to control the spread of COVID-19, the hospital was her only option. MSF’s mother and child healthcare unit in Timergara is the largest maternal health facility in a 100-kilometre radius, and the team assists with more than 1,200 deliveries every month.
Babies don’t stop during COVID-19
MSF’s Timergara project was faced with a significant challenge when, out of a team of 500, more than 200 staff members had to either isolate or quarantine at different times between April and June because of COVID-19 – they were either confirmed or suspected cases. In addition, many other staff could not come to work as the areas where they live were under lockdown and they did not have any means of transport to reach the hospital.

This could have affected the level of patient care, and at one point the team also feared having to suspend activities. But they worked tirelessly to keep the services running. The remaining team members worked double-shifts for three or four weeks, cancelled holidays, hired daily workers for medical and non-medical positions, and arranged for extra administrative and logistical staff to come from the MSF coordination office in Islamabad. They also received additional medical staff support from the Ministry of Health.
“About 70 per cent of the mothers we see in our facility come when they are already in active labour,” says Said Raziq, MSF’s medical referent for the project. “It was impossible for us to send them to another hospital when none were providing free care for hundreds of kilometres.”
However, our women’s hospital in Peshawar, in the country’s northwest, did not have the advantage of external medical staffing support from the ministry of health. After a team member tested positive there for COVID-19 in early April, the hospital lost nearly half of its staff due to quarantine measures and had to suspend activities.
They stopped accepting new patients, transferred current patients to a public hospital located nearby, and informed village-level health units and communities of the changes. The measures were implemented to try and stop further spread of the virus.
“I was really afraid of going to any hospital for my delivery,” says Mehvish, who delivered her baby girl at the women’s hospital in Peshawar. “I thought I would catch COVID-19. My friend’s father died of it ... I did not go to my doctor even for my antenatal check-ups.”
“When I finally came to the MSF women’s hospital, on the recommendation of my relatives, I was relieved to see the prevention measures being taken to stop the virus from spreading,” says Mehvish. “I am not worried about COVID-19 anymore.”
Stepping back is never easy
It was a difficult decision for MSF to suspend activities in Peshawar, even for a short period, as people we treat there, including Afghan refugees, have very few options for good quality, free maternal and newborn healthcare.
As the team feared that some pregnant women might still arrive at the women’s hospital in active labour with no time for them to travel to the public hospital, they prepared a room for emergency deliveries with medical staff available 24/7.
“We made structural improvements to the facility to create more space, implemented infection prevention and control measures, and trained staff on how to protect themselves and their patient while local transmission rates remained high,” said Marion Restrepo, the MSF medical advisor at Peshawar women’s hospital.
After six weeks, the hospital resumed its services. The new layout of the hospital had increased spacing between beds; there was a COVID-19 screening area at the entrance; and infection prevention and control measures, including personal protective equipment such as masks, were available for the medical staff, patients and caretakers. The hospital also now has an isolation delivery room for mothers with COVID-19 symptoms.
One of the biggest challenges is to maintain adequate staffing levels when there is already local transmission and if one member of staff is exposed, their entire team must be placed in quarantine to stop the transmission.Carmenza Galvez, MSF medical coordinator
In Balochistan, MSF works in Chaman, Quetta/Kuchlak, and in Dera Maura Jamali in the east of the province. We run three maternity wards in the province, along with two newborn units, two paediatric wards and an emergency room for trauma patients. These inpatient activities are complemented by outpatient activities including antenatal care, family planning, vaccinations, health promotion, mental health, nutrition and laboratory services.
Although COVID-19 forced the temporary suspension of outpatient maternal and child care services, our teams established safe pathways in the mother and child healthcare centres to allow their birthing units to stay open, isolation facilities where COVID-19-symptomatic women can give birth. We also safeguarded safe delivery options remained available to mothers. Together with the referral ambulances, MSF has ensured this constant level of care remains available.
“One of the biggest challenges is to maintain adequate staffing levels when there is already local transmission and if one member of staff is exposed, their entire team must be placed in quarantine to stop the transmission,” says Carmenza Galvez, MSF medical coordinator. “To prevent this scenario, strict infection prevention and control procedures are in place. These are reinforced by continuous education of staff about the disease, and its transmission and prevention.”
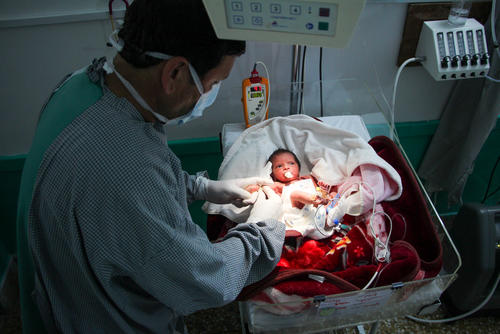
Hepatitis C and cutaneous leishmaniasis
To reduce the risk of COVID-19 transmission, the team in the MSF hepatitis C clinic in Karachi only sees patients two days a week. The people that come to the clinic are new patients or those who need in-person follow-up consultations. During the pandemic, we have provided most of our patients with three months’ worth of medication to cover their treatment, so they can avoid frequent clinic visits.
MSF operates five cutaneous leishmaniasis treatment centres in Peshawar, Bannu and Quetta. The treatment centres are located in government-owned facilities; MSF had to suspend these services after the Ministry of Health closed all outpatient services in March and April. Now that outpatient services are slowly reopening across the country, we are gradually resuming cutaneous leishmaniasis services after implementing new infection prevention and control measures.
Our priority is to continue essential lifesaving activities across the country. Pakistan fears another increase in COVID-19 patients, but MSF teams are better prepared this time. The infection prevention and control measures have been implemented taking into account the worst-case scenario, where anyone can be a COVID-19 virus carrier. Although the fear of contracting the virus remains, we are committed to providing services for patients in a safe environment.