101,500
101,5
21,800
21,8
19,700
19,7

9,500
9,5
4,200
4,2
4,000
4,

3,400
3,4
Much of the public infrastructure, including health facilities, has been destroyed by the warring parties. Import restrictions due to the imposition of a blockade by the Saudi-led coalition (SLC) in 2015, coupled with high inflation, has crippled Yemenis’ access to healthcare and other essential services. Furthermore, many of the country’s 50,000 health workers have not been paid since August 2016 and have consequently left the public health system, forced to look for other sources of income.
All these factors have led to the collapse of the health system, and outbreaks of diseases, such as cholera and diphtheria. Even where medical facilities are operational, most people are no longer able to afford the transport costs to go to them. This means they are unable to seek timely care, and easily curable health conditions are turning deadly when left untreated.
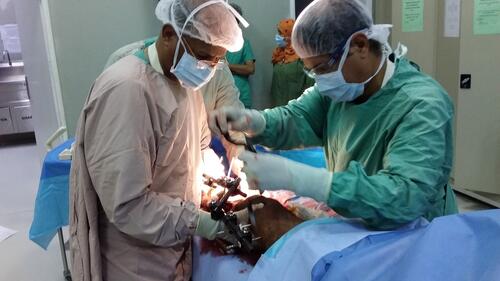
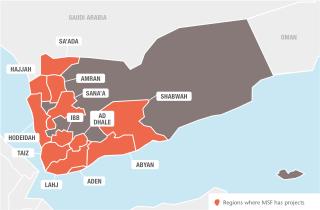
To respond to the growing humanitarian needs, MSF scaled up its activities in Yemen in 2017, working in 13 hospitals and health centres in 12 governorates, and supporting 20 public health facilities. MSF teams are back in the Haydan and Abs hospitals that were bombed by SLC in October 2015 and August 2016, respectively. MSF employs more than 1,790 national and international staff and supports over 1,000 health ministry employees, which makes Yemen one of its biggest missions in terms of human resources.
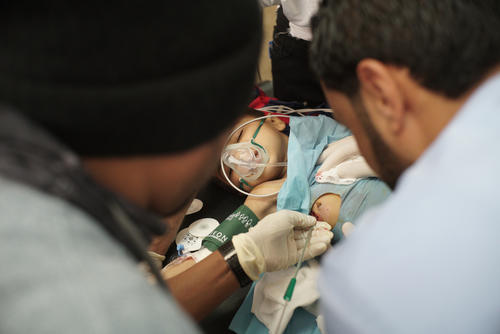
MSF teams performed 19,728 surgical interventions in the country during 2017. At the emergency surgical hospital MSF runs in Aden, the team saw an increase in the number of patients admitted for surgery, not only from the frontlines, but also from within the city, due to an upsurge in violence.
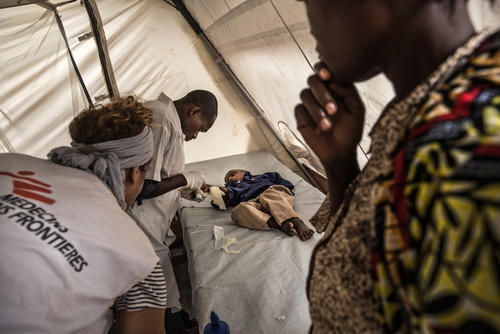
Many basic health conditions cannot be treated by the time patients make it to MSF clinics. For example, a growing number of women deliver their babies at home or arrive with complications. In Taiz, Yemen’s second largest city and the scene of intense fighting for over two years, MSF assisted more than 7,900 deliveries in 2017 at Al-Houban mother and child hospital. On both sides of the frontline in Taiz, indiscriminate violence continues to threaten civilian lives every day.
In addition, MSF donated medical supplies, including surgical kits and medicine, to more than 20 governmental hospitals and health facilities across the country.

Cholera, a crisis within a crisis
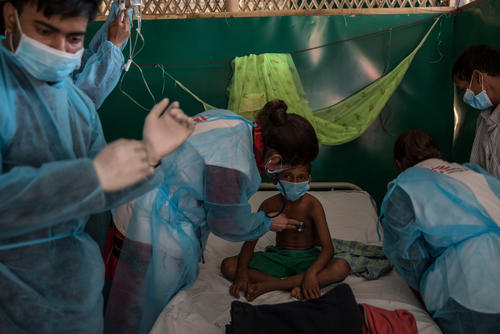
MSF admitted 101,475 to its cholera treatment centres (CTCs) over the year. The cholera outbreak of 2017 exemplifies the consequences of the conflict on the Yemeni people. If there had not been a war, they would not have faced the same challenges in accessing clean water, disposing of waste and obtaining medical care.
In April 2017, when the outbreak started, MSF immediately launched a response, opening 37 CTCs and oral rehydration points in nine of the 22 Yemeni governorates. The 15-bed treatment unit set up in Khamir hospital in Amran was soon full and had to be replaced with a larger one with 100 beds. In Hajjah, one of the most severely affected governorates, the Abs CTC alone admitted 15,769 patients, almost a sixth of the total admitted by MSF during the epidemic. In Ibb governorate, as well as setting up CTCs, MSF trained hospital staff to identify and treat the disease, and referred the most vulnerable patients to treatment centres. CTC teams also provided training on best practices to prevent the spread of the disease and organised outreach activities to monitor the quality of water, distribute decontamination kits and raise awareness.
In the third week of June, when the outbreak reached its peak, MSF admitted 11,139 patients. After this, the number of admissions started to decrease, and there were only a few hundred in October.
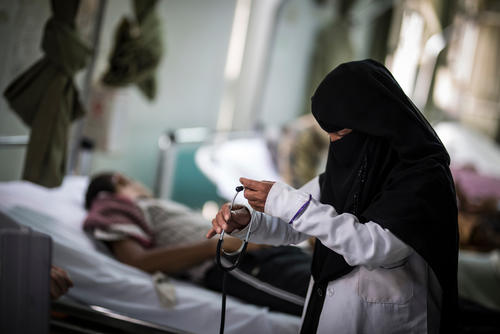
Diphtheria, the re-emergence of a neglected and forgotten disease
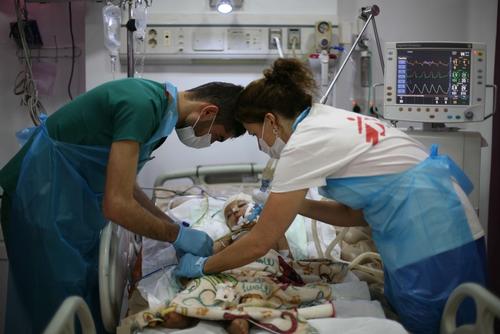
As the cholera epidemic subsided, teams began to see the first patients with diphtheria. Nearly 70 per cent of the suspected cases were identified in Ibb, with the rest scattered across 15 other governorates. This disease, which can be fatal in up to 40 per cent of cases if left untreated, was eliminated from most countries after systematic childhood vaccination campaigns. The last case in Yemen was recorded in 1992, and the last outbreak in 1982.
In response, MSF opened a diphtheria treatment unit in Nasser hospital in Ibb city and at Al Nasr Hospital in Ad Dhale, and supported two others in Yarim and Jiblah hospitals, the latter with intensive care capacity. An ambulance referral system was also set up to transport patients to the hospital. In addition, MSF supports the transport of samples to a laboratory and carries out community-based health promotion activities. In 2017, MSF treated more than 400 patients suffering from diphtheria.
Renal failure treatment
Since 2015, four of Yemen’s 32 kidney treatment centres have been forced to close. The 28 remaining centres are running out of essential supplies, so treatment is often interrupted.
Over the past two years, MSF has imported more than 800 tonnes of dialysis supplies and provided over 83,000 dialysis sessions for some 800 patients, as well as supporting six dialysis treatment centres. Three of these have now been handed over to another organisation. More than 4,400 renal failure patients remain in urgent need of care.
Challenges to MSF’s programmes in Yemen going forward
The respect for humanitarian principles and the safety of medical facilities and staff remain key concerns for MSF, as well as import limitations due to the blockade and its effects on the Yemeni healthcare system.
Authorities in Sana’a and Aden continue to impose new and often arbitrary requirements and restrictions on aid operations across the country. In November 2017, the SLC imposed a complete blockade on humanitarian staff and cargo at the ports and airports under its control, thereby hampering MSF’s capacity to assist vulnerable communities in need. In 2017, the MSF office in Djibouti arranged more than 200 flights from Djibouti to Yemen, carrying more than 500 tonnes of cargo and 1,200 staff going to work in the country.