14,300
14,3
690
69
280
28

330
33
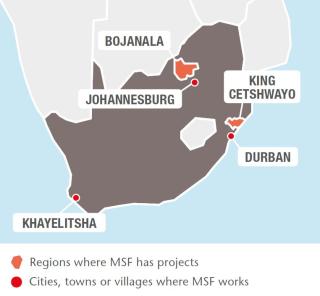
King Cetshwayo district, KwaZulu-Natal
The MSF HIV and TB project in King Cetshwayo district uses innovative community-based strategies to reduce the incidence of the diseases, as well as sickness and mortality.
Since 2012, as part of its outreach testing services, MSF has annually performed an average of 4,500 HIV tests in over 30 high schools. This has not only increased HIV testing coverage in the district, but also demonstrated the feasibility of delivering sexual and reproductive health services on school grounds.
A process to decentralise drug-resistant TB (DR-TB) care is underway in the district, so patients can receive treatment closer to their homes. MSF initiated 126 patients on a new treatment for DR-TB, including a new drug, bedaquiline, in a hospital in the district.
In Durban, the province’s largest city, MSF launched a clinical trial called TB Practecal in partnership with the TB and HIV Investigative Network. The trial is aimed at finding a shorter, more effective treatment regimen for DR-TB that does not require patients to undergo painful daily injections, and has fewer debilitating side effects.
Khayelitsha, Western Cape
The Khayelitsha project near Cape Town continues to develop innovative interventions in HIV and DR-TB care, with the aim of influencing local, national, regional and international policies on treatment for these diseases.
The project successfully increased access to new drugs for DR-TB patients, and currently has some of the largest groups of patients on the new drugs, or combinations of them. This was a major factor in the project being chosen as a site for the multi-location endTB trial, which seeks to revolutionise treatment for the toughest strains of TB.
A focus on alcohol disorders as the most common reason that DR-TB patients interrupt treatment was the project’s major patient support intervention in 2017. The effectiveness of oral self-testing as a tool for increasing the number of people who are aware of their HIV status was investigated.
The project also piloted postnatal support clubs for mothers and their babies in primary healthcare facilities in partnership with Mothers2Mothers, aiming to provide integrated care and prevention of mother-to-child HIV transmission. No transmission was recorded 18 months after the women gave birth.
Rustenburg, North West
In 2017, MSF continued its support to the provincial health department, expanding access to medical and psychosocial care for victims of sexual violence in Bojanala district. The project is located in South Africa’s platinum mining belt, where one in four women between the ages of 18 and 49 have been raped in their lifetime.
A total of 332 victims of sexual violence were treated in three MSF-supported primary healthcare facilities called ‘Kgomotso care centres’, where an essential package of medical care, forensic examination and psychosocial services is available to victims.
To increase the numbers of patients accessing services and referred to the centres in 2017, MSF positioned social workers in a community-based organisation and a local police station. MSF nurses also supported the provision of sexual and reproductive health services, including choice of termination of pregnancy in two primary healthcare facilities. Between September and December, a total of 428 clients had first trimester terminations in MSF-supported facilities.
MSF continued to advocate increased access to comprehensive services at healthcare facilities for victims of sexual violence nationwide. A report, Untreated Violence: Critical gaps in medical and clinical forensic care for survivors of sexual violence in South Africa, publicised the findings of MSF’s telephone survey of facilities designated across the country to provide care for victims of sexual violence. The survey found that 73 per cent of participating facilities do not provide or do not have the capacity to offer all necessary services.
Fix the Patent Laws (FTPL)
Launched in 2011 with MSF as a founding member, the FTPL campaign is a coalition of 36 patient groups and organisations, which advocates reform of South Africa’s intellectual property laws to address obstacles to access to affordable medicines.
In August 2017, the Department of Trade and Industry published a new draft of the Intellectual Property Policy for public comment, which was welcomed by the FTPL coalition as it recognised the need for a balance between public health and intellectual property protection.
The FTPL coalition continues to exert pressure on the government to expedite the pace of legislative reform. A final policy and reform bills are expected to be debated by parliament in 2018.
Stop Stockouts Project (SSP)
The SSP is a consortium of organisations – including MSF – who are dedicated to assisting the thousands of people living in South Africa whose livelihoods and lives are threatened by chronic shortages of essential medication.
SSP crowd-sources stockout reports from health service users, healthcare workers and volunteers, and maps reported cases. SSP pushes for the rapid resolution of stockouts and shortages through engagement with suppliers, government and other stakeholders.
At the International AIDS Society conference in 2017, SSP presented an economic analysis of the cost impact that stockouts of HIV and TB medicines have on affected individuals and the health system. Stockouts can be impoverishing for at least 40 per cent of health service users, and efforts made by healthcare workers to source medicines in the event of stockouts place a substantial financial burden on the health system.
243
243
10.2 M
10.2M
1999
1999
Patient Story
“For 29 years I endured physical and mental abuse at the hands of my husband. I stayed with him because in our culture, we respect the wishes of our parents, and my mother felt it would humiliate her if I left him. In 2014 and 2015 I lost my mother, sister and brother, and my life fell apart – I could no longer face my home but had nowhere else to go.
On the streets of Boitekong I had met a healthcare worker called Rosina from MSF, who told me about the services for victims of partner violence at the Kgomotso care centre at Boitekong community health centre. I borrowed 20 rand (US$1.70), and took a taxi to the centre, where I was counselled and then transported to a shelter for vulnerable women and children.
I feel strong now, and ready to leave the shelter. If an abused woman hears my story, I want her to know that I used to hide my problems, but if you don’t seek help it can kill you from inside. Getting to a clinic and talking to a counsellor saved my life.”