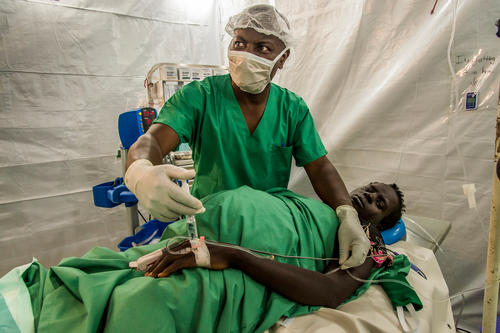
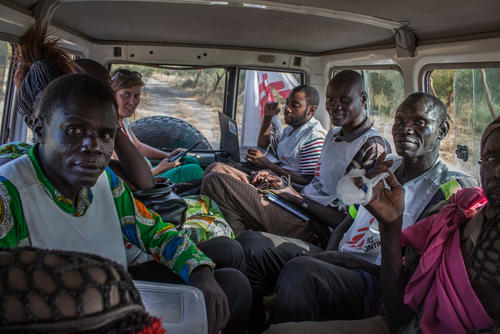Treating patients in Old Fangak, one of South Sudan’s remote areas.
War has forced roughly a third of the population of South Sudan to flee their homes. While many hoped that South Sudan would enjoy peace after it became independent from Sudan in 2011, another conflict broke out between factions of the newly formed country in 2013.
In Old Fangak - one of 16 areas in South Sudan where MSF provides medical care - MSF runs a hospital and outreach activities for a population living along the Phow and White Nile rivers, where the land becomes a giant swamp during the rainy season from May to October each year. The forbidding geography makes it a refuge for people fleeing fighting.

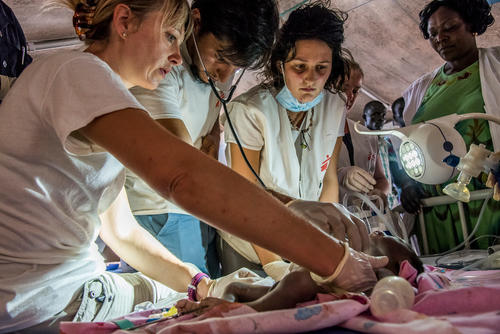
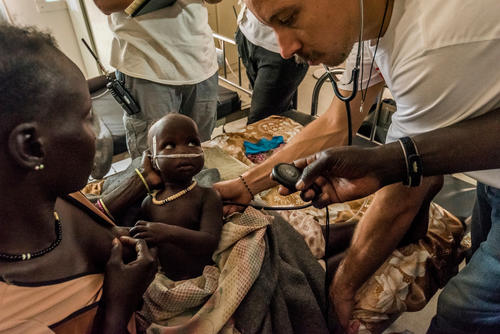

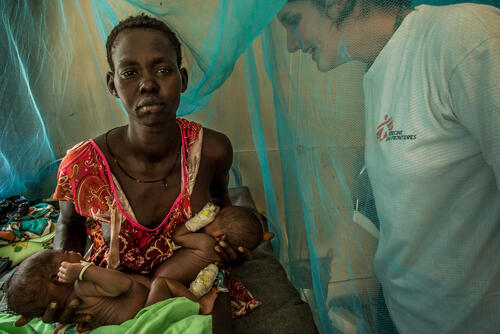
A lot of people's lives have been completely disrupted.Michael Parker, project coordinator in Old Fangak
People in this area of South Sudan subsist on raising cattle, fishing, crops such as maize and small-scale trading and commerce. The conflict has reduced the grazing areas for cattle and disrupted the few existing schools and clinics that people had access to. "A lot of people's lives have been completely disrupted," says Michael Parker, who served as project coordinator in Old Fangak and later as deputy head of mission. Many rely on emergency air drops of food from humanitarian agencies.

Access to health care is very limited, and MSF's hospital in Old Fangak is often the only place people in the region can receive treatment for serious conditions. "Patients often come from remote villages and walk for several hours on foot, under the rain, the sun and in the mud to reach the hospital, while some are carried on a traditional stretcher," says Aamir Jamal, MSF's project coordinator in Old Fangak.
The long journey makes it especially difficult for patients with emergency needs, including women with complications during childbirth. "The normal practice in this area is for women to deliver at home with a traditional birth attendant, and this might mean they don't receive proper antenatal care and that complications are not anticipated," says Dr. Adi Nadimpalli, MSF medical coordinator for South Sudan. "We work a lot in the community to encourage women to receive prenatal care and deliver in the hospital, because it is safer for the mother and the baby."
MSF has expanded the hospital into a 41-bed facility and added surgical capacity in December 2017, performing 82 surgical interventions in the first month of operations. The operating theatre along with the rest of the hospital have been rehabilitated to meet the challenges of providing health care under difficult environmental conditions. In July 2018, MSF plans to stop the surgery program in Old Fangak while maintaining the operating theatre to respond to mass casualty events if needed.
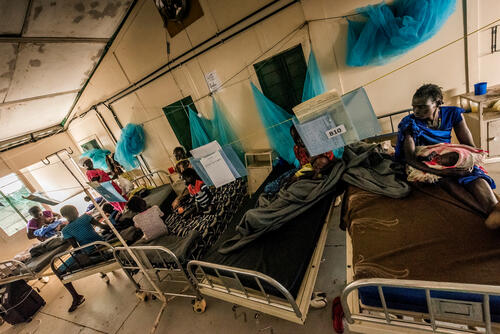
Every year, the rainy season creates huge logistical challenges. Supplies must be brought in by barge, over days and weeks. MSF staff members must be flown in by plane - when the landing strip is dry - or by helicopter. In recent years, the entire hospital compound has flooded on numerous occasions, which led MSF to build raised platforms for the hospital wards and the staff compound. "The hospital tents are set on 80-centimetre-high [2.5-foot] platforms, and concrete pathways have been built to access the various wards and facilities inside the hospital," Jamal says. "Around the area, the local community made a dike to protect the village from the flooding of the river."

Bringing Care to the Swamps of South Sudan
People in remote villages are not always able to reach the hospital on their own, or are unaware that treatment is available for their health conditions. Traveling by speedboat, MSF teams conduct mobile clinics in about 10 communities up and down the Phow and White Nile rivers. "Outreach is critical," says Parker. "You go out into the communities, you get a sense of what's going on, and you pick up people - particularly pregnant women with complications - and you take them to the hospital." Teams also often administer routine vaccinations for children (called EPI, or extended program of immunisation) and ask about potential cases of infectious diseases, such as measles or acute watery diarrhoea. "It's important to engage with communities in these hard-to-reach areas," Dr. Nadimpalli says. "We also have a sort of radio communication with some of the villages, and we ask them to call us when there is a problem, so we can decide if we need to send a boat to pick up some of the patients."
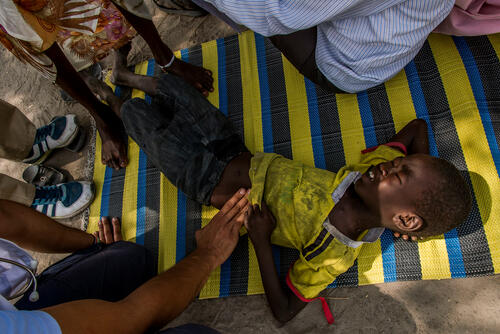


As the rains continue, certain diseases are more likely to occur, including malaria and cholera. The environment also increases the risk of other infections, such as in open wounds exposed to floodwaters. Despite the many challenges that patients and medical workers face in this environment, the hospital remains the best hope for many people with serious conditions. "The fact that people continually come to the hospital, despite the rain, the long distances and the lack of certain specialised services, shows us why we need to be here," Jamal says.
Photography by Frédéric Noy. Video by Jason Rizzo. See more from Frédéric Noy at instagram.com/fredericnoy.