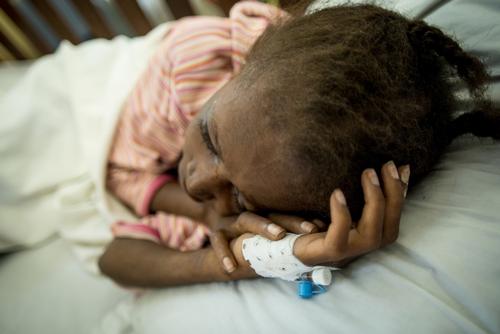
Leaders from West and Central Africa urged to mobilize national and international political commitment for an ambitious catch up plan to intensify the HIV response in the region
Dakar – As high level officials convene today in Abidjan to discuss increased access to HIV care for children, Médecins Sans Frontières (MSF) welcomes this initiative confirming what its medical teams see on the ground, but warns that the dramatically low coverage of pediatric antiretroviral (ARV) in West and Central Africa is but a tragic example of a much wider problem of a lack of action on the HIV/AIDS front in regions left behind. The organization urges leaders to adopt and implement a catch up plan to increase access to ARVs for all in countries with low access to treatment.
In a report released last month “Out of focus: How millions of people in West and Central Africa are being left out of the global HIV response”, MSF highlighted the particularly low coverage of pediatric ARVs in West and Central Africa. Close to half of all children infected with HIV live in this region which accounts for only 18% of all people living with HIV in the world. Barely one in ten of those children in need there is on life-saving treatment.
“Considering that the prevention of mother-to-child infection is the strongest success story in HIV care, no child today should be born with HIV in the first place. The fact that such a disproportionate number of HIV infections in infants happen in West and Central Africa is a clear sign of the failures of the HIV response in the region. Antiretroviral treatment coverage needs to be urgently increased for all, so as to protect not only the children but also their mothers, fathers, kin and communities”, says Dr Eric Goemaere, MSF’s HIV/TB referent.
A pregnant or breastfeeding HIV+ woman on successful ARV treatment has less than 2% risk of transmitting the virus to her infant. In West and Central Africa, the high number of infections in infants is due to low access to treatment for their mothers, with just 42% of HIV-positive pregnant women receiving ARVs compared to 88% in the Eastern and Southern Africa regions.
Country examples:
Lack of testing of pregnant women to avoid their newborn being infected:
In Guinea, the Democratic Republic of Congo and the Central African Republic (CAR), only 11 to 16% of pregnant women are screened for HIV, meaning that undiagnosed HIV positive women remain unknowingly at risk of transmitting the virus to their infants.
In CAR, only half of the 119 sites offering services preventing mother-to-child transmission were functional in 2015 and over a third of these only in the capital.
Lack of early infant diagnostic (EID):
- In CAR, an early infant diagnostic test cost 57 USD. In a country where 62% of the population live with less than $1.25 a day, this fee is unaffordable for most patients. UNICEF covers the costs for the tests but puts a cap of 500 tests to be performed nationwide each year, leaving over two thirds of the 1700 children infected each year undiagnosed and therefore very unlikely to survive.
- In Guinea, only four sites in the country offer early infant diagnostic tests. Due to the low availability, only 7% of infants born from HIV positive mothers were screened in 2014. In the DRC, only 13% of exposed children are tested for HIV overall.
- Last August in Carnot (CAR), 56 newborns exposed to HIV were tested, but their test results never came back from the laboratory in the capital.
- Because of the difficulties to getting results for infants, MSF teams in CAR and DRC have turned to sending their samples to laboratory outside the country to get results.
Only 10% of infants of HIV-positive mothers in West and Central Africa are tested for HIV within two months of their birth, compared to 50% in high HIV prevalence countries of Eastern and Southern Africa. Early infant diagnosis testing is unavailable in most health facilities. Getting timely results of the limited number of tests performed is crucial to ensuring the survival of HIV infected babies; however, this has proven very difficult, either because there are not enough tests available, or because patients have to pay for them, or because inadequate transport and communication systems mean that the result takes up to six months to be received by the health care provider – with valuable time being lost to start treatment. Besides these diagnostic barriers, access to and retention on treatment is hampered by the non-availability of pediatric formulations, frequent stock outs of essential commodities, payment requirement from patients, and lack of counselling and patient support.
MSF calls on African leaders to strongly ask the UN member states gathering in the high level meeting on HIV in New York next month to urgently address the current treatment gap in West and Central Africa. The world’s commitment to accelerate the HIV response must be secured, including for those now left behind.
“The upcoming UN high level meeting on HIV/AIDS is a unique, and perhaps the last, opportunity to close the treatment gap, not only for children but also for all people living with HIV. Governments of countries left behind the HIV/AIDS response, particularly in West and Central Africa, should seize this chance to ask loud and clear an increased commitment from the international community to intensify the HIV response for people facing a deadly treatment gap”, says Dr Mit Philips, MSF’s health policy advisor.
Médecins Sans Frontières (MSF) has been working on HIV/AIDS since the late 1990’s. It currently supports treatment for over 200,000 patients in 19 countries, primarily in Africa. This includes HIV programs and activities in West and Central Africa: DRC, Guinea, CAR, Chad, Niger and Mali as well as other countries with low ART coverage such as South Sudan, Yemen and Myanmar.
West and Central Africa is composed of 25 countries: Benin, Burkina Faso, Burundi, Cameroon, Cape Verde, Central African Republic, Chad, Congo, Cote d’Ivoire, Democratic Republic of the Congo, Equatorial Guinea, Gabon, Gambia, Ghana, Guinea, Guinea-Bissau, Liberia, Mali, Mauritania, Niger, Nigeria, São Tomé and Príncipe, Senegal, Sierra Leone, Togo