Miriam Alía, an MSF vaccination expert, has just returned from Equateur province in the Democratic Republic of Congo (DRC). Miriam worked as a medical referent in the area of Itipo, the epicentre of the recent outbreak. She explains how MSF took part in the ring vaccination against the disease and tells of her personal experience working with Congolese health workers.
For three weeks I was part of the MSF medical team responding to the Ebola epidemic in Itipo, a remote area south of the city of Mbandaka in DRC, where a number of people had tested positive for Ebola. While caring for patients in the treatment centres we had set up in collaboration with the Ministry of Health, we implemented the other ‘pillars’ of an Ebola response. For instance, we were finding people who had been in touch with Ebola patients – ‘patient contacts’ – and informing communities about the disease and how to avoid getting infected.
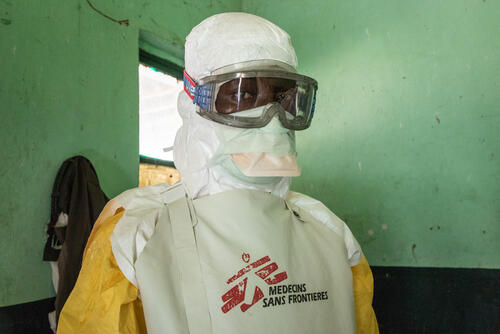
A key component of the response is to make sure that the health system continues to function properly during the outbreak. That means health workers are protected and know how to identify suspected cases. If this is in place, we have a good chance to slow down and then stop the spread of the disease, and to avoid deaths linked to other medical conditions such as malaria. Often health staff can be afraid of treating patients due to the risk of infection from Ebola.
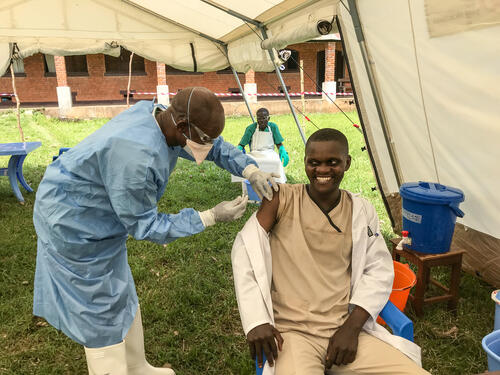
This year in DRC we had an additional tool to use against Ebola: an investigational vaccine. In Itipo, MSF, in partnership with the World Health Organization and the Congolese Ministry of Health, was in charge of vaccinating those most at risk of contracting the virus. This included not only the contacts of confirmed Ebola patients and the contacts of those contacts, but also the people on the frontline of the fight against Ebola, i.e. healthcare workers, traditional healers, local religious leaders and motorbike taxi drivers. Sadly, the infection of healthcare workers is something that we see in many outbreaks of Ebola, as they are obviously most at risk of catching the disease when sick people come to them for help. It was great to be able to offer them the vaccine, and in turn some protection.
A key component of the response is to make sure that the health system continues to function properly during the outbreak. That means health workers are protected and know how to identify suspected cases.
This vaccine against Ebola had already been used in clinical trials in West Africa during the 2014-2016 outbreak. But this was in Sierra Leone, and in Conakry, the large Guinean capital city. In Itipo this year, we faced another kind of challenge: the area we were covering was made up of eight health zones, including 46 health centres and health posts, many of them located in remote villages. To reach them and vaccinate their health staff, we had to use motorbikes, pirogues (canoes) and sometimes go on foot for several kilometres through the forest.
Most of the health staff we vaccinated were nurses. Some of them were working completely alone in remote health posts. Others worked in groups of three or four in larger health centres. We didn’t have to convince them to be vaccinated. They were quite afraid of the disease and knew very well that the head nurse from Itipo had just died of Ebola, along with 20 other people in the area.

While we are confident that the vaccine works and had seen very promising data from other trials, we had to be sure to explain to the staff that they needed to continue caring for suspected Ebola patients with all the necessary precautions. They needed to use the protective material that we provided them with, and be aware that it takes five to 10 days after vaccination for the immune system to be activated and provide protection against the virus.
We also trained them about how to put in place a proper triage system and detect suspected Ebola patients at the clinic door. We explained that if they then detected a suspected case, they were to contact us and a properly trained ambulance team would come and collect the patient safely.
The dedication of these healthcare workers, who care for their communities with very little resources, is what impressed me the most during my time in Itipo. They show an amazing level of commitment to their patients.
I will notably remember George, a nurse from Itipo. His wife had been diagnosed with a confirmed case of Ebola and transferred to a treatment centre in Bikoro, another village where MSF was helping the Ministry of Health to run an Ebola treatment centre. But he chose to stay in his village and provide medical care to the community. He also volunteered to disinfect the houses of patients suspected of being infected with Ebola. During their 21-day follow-up as contacts of a confirmed Ebola case, George’s son fell sick, which obviously worried him a lot, but fortunately the boy tested negative. A couple of days after the child tested negative, his mother was discharged after beating the disease. All ended well for this wonderful man. Later, he joined our team as a nurse at the Ebola transit centre we were running in Itipo.