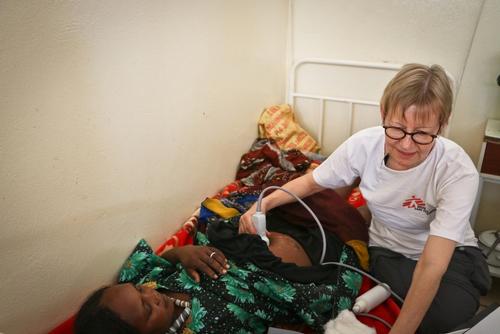
Heavily pregnant, Miriam rests on the bed as an MSF gynaecologist performs an ultrasound of her growing belly. She seems surprised when, unexpectedly, the outline of a baby appears on the monitor, and her expression quickly turns to relief as the translator confirms that Miriam’s unborn child is progressing well.
Miriam is one of 44 patients with hepatitis E who have been admitted to Am Timan hospital in Chad since September. More than 320 other potential cases have been identified.
The first cases of hepatitis E were diagnosed at Am Timan hospital in late August. Like cholera, hepatitis E is transmitted from one person to another, mainly through contaminated drinking water, and rapidly spreads in places where hygiene and sanitary conditions are poor.
Miriam is a mother of nine, and her tenth child is due in February. It is estimated that one in 25 patients with hepatitis E is at risk of death, but for pregnant women in their third trimester, the risks of maternal and fetal mortality are higher. Among the nine patients who have died in the past few months, three were pregnant women with jaundice.
Brought to Am Timan after seeking treatment at an MSF mobile clinic in Ardo, Miriam is part of a nomadic community and this is the first time she has ever been in hospital. She explained, "I was not able to feel the heartbeat of the baby for over a week. I spent 25 days in my bed without moving. It was the first time I felt so sick." The team in Ardo immediately recognised the symptoms of hepatitis E, including jaundice, and decided Miriam needed further treatment at the hospital which was a three-hour drive away. Jaundice, also known as icterus, is the yellowing of the skin and the whites of the eyes. It’s one of the most obvious signs that a person may have hepatitis E.
Veronica Siebenkotten-Branca, an MSF gynaecologist in Am Timan, explains that hepatitis E has no cure and is particularly dangerous for pregnant women like Miriam. "Depending on how severe the hepatitis E infection is during pregnancy, it can potentially lead to serious consequences for maternal and fetal health. Abortion, post-partum haemorrhage, and premature or still birth are among the worst situations a mother can face."
MSF provides HIV and tuberculosis (TB) care in Am Timan hospital and is working in the paediatric and maternity departments. Within days of her admission to the hospital, Miriam’s health had improved. "Now I can finally feel my baby again. Before I was so afraid to come to a hospital, but now I feel much better and I hope I will able to go back to my community soon." As a nomad, Miriam and her family rarely spend longer than a few months in one place. In the dry season, the group moves to the far south of the country, and then travels north during the rainy season. The journey in between can last for over a month, with around 200 people on the move with their livestock, stopping to plant grains along the way.
Ngomdimadje, a 25-year-old teacher, was the first patient to survive hepatitis E in Am Timan. He lives with his cousins in a rented house in the central Salamat district. Around four months ago, after he returned from teaching young elementary students in Harazè, near the border with the Central African Republic, he started to experience severe body pain. He said that at that time he felt close to death, and was suffering from loss of appetite, severe vomiting, headaches and abdominal pains. He was barely able to move or walk. Critically ill, Ngomdimadje managed to travel to Am Timan hospital where he was diagnosed with hepatitis E.

He was admitted to hospital and his health started to deteriorate. The MSF medical team treated and closely monitored him for over two weeks. He has now made a full recovery. "Today, I call myself a survivor because, as long as I am breathing, I survived this potentially deadly disease. Before me, the other two female patients didn't make it. Calling myself a survivor is truthful and it is hopeful."
Since the first cases of hepatitis E were identified, more than 600 MSF staff have been working to test for new cases, treat patients and improve water supplies and sanitation. Many staff are community health workers whose main role is to talk to people about the early signs and symptoms of hepatitis E and to share information about hygiene practices. Most people in Am Timan had not previously heard of hepatitis E, and as a result, staff are working to address fear and suspicion about the "sick people with yellow eyes". This work includes meeting with local chiefs, leaders and officials, to hear their concerns, identify needs and encourage them to talk to their community about the urgency of responding to hepatitis E. In the last four weeks, they have also distributed more than 11,000 hygiene kits containing bars of soap and buckets. In many cases, hepatitis E patients have been seen as a threat to the community, leading to both stigmatisation and shame for those who are diagnosed. But with support from community outreach workers, this is changing.
MSF has been working in Chad since 1981. Before the current hepatitis E outbreak, MSF had been running regular medical programmes in Am Timan and in Moissala. Earlier this year, MSF launched an emergency nutrition response in Bokoro where, in partnership with the Ministry of Health, MSF runs 15 mobile outpatient clinics and an intensive therapeutic feeding centre in Bokoro hospital to treat malnourished children. MSF also launched an emergency response in March 2015 in the Lake Chad region for people displaced due to violence by Boko Haram. Teams based in Baga Sola and Bol continue to provide assistance to the people around Lake Chad. In the capital, N’djamena, MSF supports Ministry of Health hospitals by training staff on the management of mass casualties in order to increase their capacity to respond to emergency situations.