In the middle of the African continent, Central African Republic (CAR) is only slightly smaller than France, but has limited roads connecting regional centres with the capital, Bangui. Hundreds of thousands of people in CAR have been displaced due to violence, and security remains a concern following intense conflict in 2013-2014. Dr Belen Caminoa, an MSF paediatrics advisor, recently criss-crossed the republic by plane to assess three hospitals run by MSF, where providing and accessing care comes with many challenges. She explains how a visit from a medical advisor helps review skills and protocols with hard-working teams and shares the story of a critically ill newborn admitted to the newborn unit in Paoua, in the northwest of the country.
Assessing activities and guiding medical care
For a medical advisor like Dr Belen Caminoa, a field visit typically responds to a request from the operations team in headquarters. It will entail assessing how activities are progressing, following up on any training that has been conducted, providing additional training where needed, discussing queries from teams regarding protocols or guidelines, and reviewing first-hand any critical cases that are in care during the visit. Depending on the country, there is quite a bit of travel involved.
“I have been following CAR since the end of 2015,” says Dr Caminoa. “Specifically, I’m looking after three projects with neonatal and paediatric activities. I spent four days in each: Carnot, in the west near Cameroon; Paoua in the northwest towards Chad; and Bria in the east, close to the border with Congo and Sudan. I flew back to the capital Bangui in between each time.”
“I start each visit by attending the morning handover. This is routine for me. It’s the opportunity to introduce myself and explain why I am visiting. Then I go through the different departments: from emergency and intensive care, then on to the rest of the wards, including the neonatal unit. If MSF’s work includes outpatient activities, I have a look at those. I also make sure I see all the workings of the hospital – for example, the maternity ward, the pharmacy, the kitchen (if there is one) – to understand how everything is working together.”
The health system in CAR has numerous gaps, including qualified staff, and child and newborn mortality remain high. MSF services are busy with high numbers of patients, so ongoing training to improve and maintain the quality of care is vital.
“I especially wanted to get feedback from our staff and to see how they had benefited from working with the new ‘Flying Paediatrician’,” explains Dr Caminoa. “This is an international staff position we’ve created for these projects in CAR. The paediatrician rotates through the three projects back-to-back, for two months in each, focusing on a different aspect of care each time. This time she had worked closely on neonatal care so I was expecting to see the results of that, especially in terms of good organisation of care and correct use of protocols.”
Giving birth at home remains common in CAR, so staff care for babies who have fallen sick since being born at home, as well as babies born in the hospital maternities.
“With our neonatal guidelines, they can treat sick and small or pre-term babies as long as they are not too complex,” says Dr Caminoa. “They can give oxygen and monitor oxygen saturation; provide IV infusions, and stabilise a critical patient if necessary; deal with sepsis (severe infection), skin infection and meningitis. Skills like these address many of the threats to newborn survival. The work ambience is good and the staff are working really hard.”
After treating measles patients hands-on in 2013, this second visit to CAR demanded a different approach.
“As a paediatrician you’re always focused on individual cases, case by case,” explains Dr Caminoa. “But as an advisor, your aim is to have an overview of the situation, to understand the context and the challenges of the project, including the wider issues like logistics and human resources, which are also linked to the care that a patient can receive. By guiding the medical care taking all these things into account, I can support the team in the field to achieve what they want to achieve, and also help them adapt to any limitations.”
Essential care for newborns
For newborns, prematurity and low birth weight, infection and lack of oxygen at birth can be deadly. With a high proportion of women giving birth at home, newborns in CAR often miss out on the essential care that can avoid, or start to address, any complications. In the rural areas of Bria, Carnot and Paoua, MSF teams can treat sick and small or pre-term babies as long as they are not too complex. Serious cases, however, require urgent airlift to the capital, Bangui.
“In Paoua we had a critically ill newborn who had been admitted with a severe infection, what we call sepsis,” Dr Caminoa recalls. “I had just arrived and gone straight to the neonatal unit. Just a few minutes after, I reached his bedside the baby had a cardiac arrest. Only after we resuscitated him did the staff have time to explain his history. He had been brought in five days after being born, and had seemed to improve, but it was now obvious that he had started to deteriorate again. His infection had developed into necrotising enterocolitis, an acute and life-threatening inflammation of the abdomen, so he needed surgery. The team and I agreed that we needed to transfer him to Bangui via the next flight, if he managed to survive.”
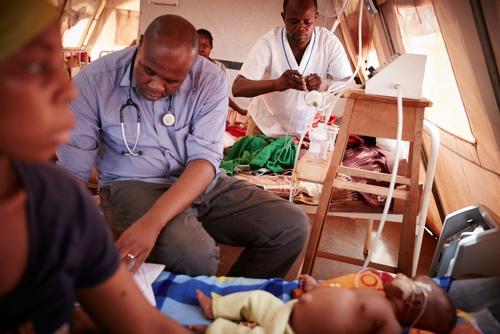
Although MSF no longer handles surgery in Paoua hospital, it looks after transfers to Bangui for all complicated surgical and trauma cases, including adults and children. In Bangui, responsibility is divided between MSF (for adults) and the Italian non-governmental agency, Emergency (for children). The two surgical facilities are located side by side.
“We explained to the mother that the transfer itself was risky, but that if her baby boy wasn’t transferred he could die,” Dr Camiona continues. “We had to wait from Thursday to Monday, keeping him stable with antibiotics, fluids and oxygen. By Monday, it turned out we had three patients to evacuate: an adult and child, each with an open fracture, and our really critical newborn.”
“We transferred him in his mother’s arms throughout the flight, while I monitored his breathing and the intravenous, or IV, infusion. In principle, he needed oxygen but we don’t have oxygen in the plane. We half-jokingly asked the pilots to fly lower to increase the amount of oxygen. Next thing, we could see the ground more clearly than we normally would! Every 15 minutes they’d turn their heads to check, ‘Is he still OK?’ We had coordinated with the team in Bangui and an ambulance was already waiting on the airstrip. As soon as we arrived, the baby was put on oxygen to help stabilise him. Once admitted to hospital, he stabilised to the extent that they could plan surgery the next day. So that was satisfying for everyone who had been involved, that we were able to care for him and get him to surgery safely when he had been so gravely ill.”
In 2015, MSF ran 17 projects across Central African Republic, involving more than 2,400 national and over 240 international staff. As one of a number of NGOs providing the majority of health services in the country, our medical activities include paediatrics, vaccination, sexual violence care, trauma surgery, and HIV management.






