Getting to Naga
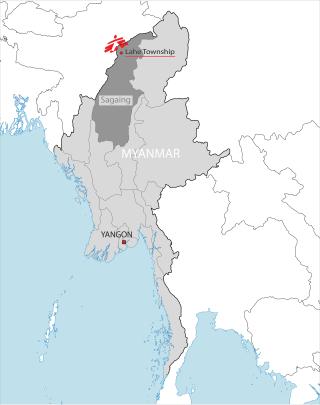
Situated in the mountainous far north-west of Myanmar's Sagaing region, Naga Self-Administered Zone is one of the most remote parts of the country, and home to the Naga people, a community living on both sides of the India-Myanmar border.
The Naga people are comprised of many tribes and retain a strong sense of cultural identity. Many in Naga, particularly in the more rural communities, sustain themselves and their families through subsistence agriculture and hunting.
In the rainy season, journeys between the two towns can take far longer than four hours and may even prove impossible if there are landslides or floods.
Rural communities

Mountainous terrain and remote villages make it difficult for people in rural communities to access basic healthcare services, even more so during the rainy season, when some of the villages can be cut off for several months.
MSF has been working in the Naga Self-Administered Zone since 2016; providing primary healthcare, hospital referrals and health education for 15 different villages in Lahe Township and supporting the Ministry of Health and Sports' (MoHS) hospital in Lahe town. We also assist in tuberculosis testing and in organising vaccination campaigns in the communities.
Our teams visit each of the 15 villages around once or twice each month. The mobile clinic team always includes a doctor and a pharmacist.
The teams rely mostly on motorcycles to traverse challenging terrain, with some of the journeys lasting up to eight hours.

Mobile clinics in Naga, Myanmar
8,400
8,4
Given the challenges many people face in reaching healthcare facilities, MSF's mobile teams can be a lifeline in emergencies and for those with serious illnesses.
The most common reasons for patients seeking medical treatment are respiratory tract infections, musculoskeletal pain and diarrhoea.
Low vaccination coverage is also an issue in the remote communities in Naga, leaving people vulnerable to preventable diseases. MSF has therefore supported MoHS in carrying out several vaccination campaigns in the past years.
Staying warm in the mountains
Naga is approximately 1,800 metres above sea level. During the winter months, temperatures can drop below zero, becoming particularly cold at night.
Most people live in wooden houses with thatched roofs, indoor fireplaces provide warmth and a place to dry meat and cook. Fires tend to burn constantly, keeping the houses warm, but making coughs and upper respiratory infections common.
Kyun
Kyun lives in Hay Khun village and has made her living through subsistence agriculture. She has had an eye condition for 10 years, and now receives treatment from the MSF mobile clinic team.
It’s so much easier to see the MSF doctors when they come here. It was different when I was young – when someone was sick, there just wasn’t anywhere to go.Kyun

“I’ve always lived here [in Hay Khun village - several hours' off-road driving from Lahe],” Kyun says. “I’ve made my living growing rice and corn in the mountains, but I don’t work anymore – now my husband and my daughter, Kyakin, grow food for us to eat. She also has three children.”
“I believe I am around 70 years old, but I’m not sure. There have been a lot of changes in Naga since our ancestors’ time – now we wear a lot more clothes! The traditional style is to wear a lot less. The nearest big towns for us are Lahe and Khamti, but it takes a long time to travel to either town, and you need a motorbike.
“I first went to see the MSF doctors because of my eye – it feels itchy and hot, and it’s been this way for ten years now. I only started seeing the doctors recently, and they’re working on my treatment.”
Kyakin
Kyakin is Kyun's daughter. She also visits the mobile clinic, along with her children.
I went to the MSF clinic for the first time yesterday for a pregnancy test. I already have three children – I delivered all of them at home by myself.Kyakin


“The most important thing for me is that they are educated, I would be sad if they had the same life I have – having to farm every day for food is exhausting,” Kyakin says. “It’s especially difficult to work without cows, to pull the ploughs, because we need to do everything manually.”
Kamor

“If it weren’t for MSF, I wouldn’t be alive today,” Kamor says. “Before I had medicine, I was so sick that I couldn’t move from my bed. But now I feel healthy and fit again. Before being treated, my whole body hurt and especially my chest.”
“I’m not sure of my exact age, but I think I’m over 80. I’ve seen a lot of changes in my life. I remember the different tribes fighting when I was young, and the establishment of Lahe township.
“Before the Christians and Buddhists and then the doctors came, we used to rely on a shaman when we were sick – sometimes they would tell us to sacrifice an animal. I’ve always been a farmer, but I don’t work anymore, so now my family support me with food and I stay home and cook.”
The work of MSF staff
Many of MSF's staff working in Naga are from the region itself, and some describe working for an organisation like MSF as a way to support the community.
All photos © MSF/Scott Hamilton, © MSF/Khine Nwe Zin














