In November 2017 a series of security incidents forced Médecins Sans Frontières (MSF) to evacuate our team from Bangassou, Central African Republic (CAR), and suspend activities in the area for five months.
In April 2018, our team returned to the city.
Assistant Medical Coordinator Dr Ernest Lualuali Ibongu has been working in Bangassou since April 2017, where he experienced the temporary suspension of activities and their resumption. Here, he describes the situation.
What was the situation in Bangassou when you first arrived?
Before I arrived, Bangassou was described to me as a “little paradise”, a haven of social cohesion in Central African Republic relatively unaffected by the intercommunal conflict that tore the country apart from 2013 to 2014. But just three days after my arrival in 2017, I found myself in an ambulance in the midst of fighting, transporting 27 war-wounded patients to the MSF hospital. It was as if the city I had heard about had disappeared.
Back then we still had a large team in the region. We were expanding the hospital, training medical staff in three rural health centres, implementing an ambitious programme in the villages where we wanted to improve access to drinking water to prevent cases of diarrhoea, and implementing prophylactic measures against malaria. These diseases don’t kill as violently as guns, but they are much more deadly. But when the insecurity got worse we had to reduce our teams.
It was an intense period. Before tensions escalated in Bangassou, the number of patients admitted for violent trauma in a month could be counted on one hand. But during April 2017, we treated 141 war-wounded patients, and they just kept coming: 30 per month, sometimes more. On top of that, people don’t stop getting sick during conflict.
But many people who needed care were so afraid of encountering armed men on their way to the hospital, that they didn’t dare attempt the journey unless they were so ill that their lives depended on it. I will never forget a case we had in August or September: a four-year-old child with a complicated case of malaria who was brought to the hospital from more than 200 kilometres away. We still don’t understand how he survived the journey.

Why was MSF forced to suspend activities in Bangassou?
Many of the challenges we faced in Bangassou come with the territory when providing humanitarian aid as close as possible to those who need it most. But we were forced to leave when we were no longer able to work under the conditions of neutrality and impartiality that are supposed to protect us in war zones. If we can’t treat people solely based on their medical needs, we fail in our mission.
For instance, I remember the case of a 12 year-old child who had been shot and wounded. The staff did everything they could to save him, and he survived. But a few months later, this same child suffered a bowel obstruction. He was living in a camp for displaced people less than a kilometre from our facility. But we were told: “If you take him to the hospital, we will kill you”. I had to resuscitate him for 48 hours in the camp, stabilise him, and transfer him more than 700 kilometres away to Bangui, where he underwent surgery.
The increase in incidents like this pushed us to wonder if our presence remained legitimate, considering armed men were forbidding us from providing care to part of the population. The armed robbery of our base in November 2017 was the last straw, and that’s when we decided to leave.
Many people who needed care were so afraid of encountering armed men on their way to the hospital, that they didn’t dare attempt the journey unless they were so ill that their lives depended on it.Dr Ernest Lualuali Ibongu, Assistant Medical Coordinator

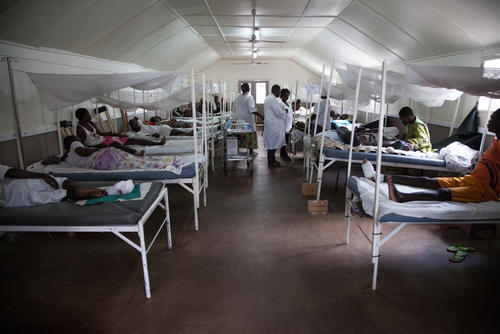
Bangassou hospital - increase of health needs in times of war
What made MSF return to Bangassou in April 2018?
The tensions in Bangassou have eased a bit recently, which encouraged us to progressively resume our operations. We returned under one condition: that all parties accept and adhere to humanitarian principles and allow access to our services for all those in need, regardless of who they are. We conducted lengthy discussions and consultations with the local people to ensure that our return—desperately needed, considering the extent of the unmet medical needs—could be carried out under acceptable safety conditions for our teams. It’s the involvement of all the communities that convinced us we could indeed come back.
We are resuming activities gradually, focusing first on paediatric and surgical emergencies. In the paediatrics department of Bangassou hospital we handle at least 60 blood transfusions per month. Here, a transfusion generally means severe malaria, which, if left untreated, can result in death. Bangassou hospital is currently the only health structure available for the region’s 200,000 inhabitants. We simply can’t let these people down. But we remain vigilant, because CAR remains one of the most dangerous contexts in the world.
How would you describe the situation in the city today?
Things have improved significantly in Bangassou. People are starting to cut the grass again and we can see the horizon. Children are playing in the streets; there are even patients who come from the displacement camp to the hospital for a consultation, which would have been unthinkable just a few months ago. But that doesn’t mean the armed fighters who operated out of Bangassou have disappeared. They have simply retreated to the periphery, and the population is still affected.
Despite all of this, I still have hope. The communities here are not as divided as they might seem. In Bangassou, Muslims and Christians have always lived together. In fact, there are a lot of mixed couples. I believe it was external events that changed the city’s internal dynamics. We could feel it during the months when we suspended our activities, when the people of Bangassou committed to working together to allow everyone to access care. Keeping this in mind helps me move forward.