Most West African and Sahelian countries face a significant number of childhood illnesses and diseases each year, mostly related to climate change or instability in the region. In the coming months, these countries will also contend with the usual peaks, when malaria and malnutrition are particularly risky. Health workers, paramedics and community agents are preparing once again to ensure that they do not severely affect the communities in the region.
Neonatal mortality remains the main morbidity for children under five, but others include pneumonia, diarrhoea (causing dehydration) and malaria. Malnutrition is also a contributing factor to almost half the deaths of under-fives, while sickle cell disease (an inherited condition of red blood cells) accounts for nearly one in ten deaths.
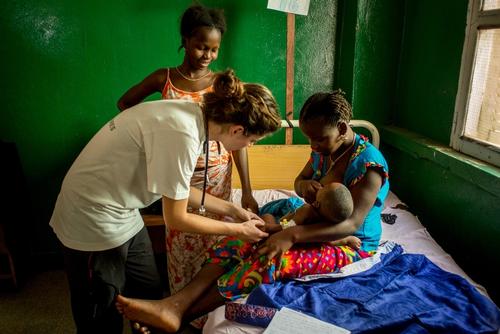
Children are one of the most vulnerable groups in humanitarian settings.
What challenges do MSF teams face in the field?
Dr Didier Mukeba Tshialala, MSF Medical Coordinator is very familiar with the needs and constraints in West Africa. He has worked with MSF in Niger for several months and has also been on several field assignments in the region.
“In Niger, we know there are several solutions that work: on the one hand, to improve access to drinking water for the populations; on the other hand, to implement chemoprophylaxis against seasonal malaria between August and November; in addition, to increase routine vaccination coverage in children of 0-11 months of age. By doing that, we can significantly improve the health status of children in Niger. However, that is not enough.”
Children are one of the most vulnerable groups in humanitarian settings. Conflicts, political insecurity, natural disasters, displacement, and challenging economic conditions all restrict access to healthcare and thus increase their vulnerability.
This is in line with Dr Nematoulaye Toure’s experience in her home country, Mali. Dr Nematoulaye is MSF Head of Neonatology and Paediatrics on the project in the district of Ansongo, in the region of Gao.
“The biggest challenge is getting access to patients. With a night-time curfew and a distance of several hundred kilometres to the nearest health centre, who would take the risk of leaving in search of medical attention? That is why it is necessary to adopt medical strategies to reach the greatest number of people, especially young children who are the most vulnerable. This is what we do, for instance, with the strategy for treating the nomadic population in Mali.”
In most of these contexts, limited resources in the field including insufficient paediatricians and paediatric nurses; poorly trained caregivers who lack knowledge about the specific needs of children; limited context-specific protocols and tools; and a shortage of medication, are creating many challenges that complicate interventions in the field.
MSF Paediatric Days: a platform for exchange
In December 2017, Dr Didier and Dr Nematoulaye attended the MSF Paediatric Days in Dakar, Senegal, one of the main academic paediatric centres in West Africa. Among the recommendations made by the participants during the conference, was the need for a stronger integration of families and community members in the paediatric programs. In addition, a more integrated approach to mother and child care, which MSF already practices in some projects implemented in West and Central Africa.
As Dr Nematoulaye testifies: “In Ansongo, we have invited traditional birth attendants to accompany women to the health centre in order to keep them calm and reassure them. An increasing number of patients have come and since the start of the project, the number of women giving birth at home has drastically decreased. Benefiting from medical care allows them to avoid many complications, and can save the life of a child and his mother when complications endanger them.”
The MSF Paediatric Days aims at addressing an urgent need to improve the quality of paediatric care in humanitarian settings. The second edition took place in December 2017, in Dakar. This very same year, the international medical organisation had around 50 projects (20 of them specialised in paediatric and maternal health care and malnutrition treatment) in 11 countries of the West African and Sahelian region.