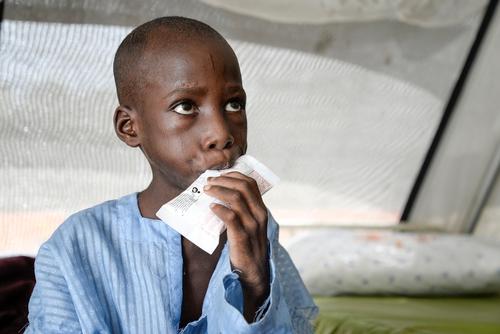
- Helle Poulsen-Dobbyns has just returned from Maiduguri – the capital of Borno State in northeastern Nigeria – where she was programme coordinator for Médecins Sans Frontières (MSF).
- She explains how malnourished children were flooding into MSF medical facilities in a region affected by the conflict between Boko Haram and the Nigerian army.
What is the situation in Maiduguri?
Our teams were confronted with huge numbers of acutely malnourished children and an increasing number of malaria cases. We didn’t expect this in the capital, where there is no conflict and aid organisations do have access to the population.
In some locations, malnutrition rates were as high as those recorded in the conflict zones. We had lots of both manifestations of severe acute malnutrition: severe marasmus, or wasting, and kids with Kwashiorkor (swellings of fluid, known as oedema, occurring on the child’s ankles, feet and belly ), but so bad that their skin developed boil-like eruptions, as if they had suffered burns. When we conducted food distribution in a camp, it was the first food these 8,000 people had received in four months.
What were the main difficulties?
Our triage was overwhelmed by the number of children under five years of age; they are the most vulnerable. But we also experienced the deaths of too many older children. They were victims of the effect of severe malaria on bodies already weakened by malnutrition, and were not able to fight off disease. That’s why I kept telling the team “it’s all about food”.
To have a targeted impact, we established criteria for who should receive the food. For example, for children discharged from the inpatient therapeutic feeding centre (ITFC), we give their mothers a family ration of one month’s food supply so that that their children wouldn’t succumb to severe acute malnutrition again. We also do a targeted food distribution to families with six or more children and with at least one child under five. This is not replacing the food distribution that would be needed for the internally displaced people living in camps or in the community. To complicate things, 90 per cent of the displaced people are hosted by communities in Maiduguri in poor conditions, with inadequate sanitation and hygiene. It’s making it harder to reach them and such conditions are like an incubator, spreading disease.
How is MSF responding to the emergency?
To deal with the influx of patients, we first increased our capacity to manage them by recruiting new staff, who are trained by our existing staff while receiving and treating a huge number of new emergency cases.
Then we worked on the management of our medical facilities. For example, in our Maimusari clinic, we have nurses triaging within the patient queues, to ensure prompt identification, which would then allow us to give the necessary care to the most severe cases: the children were so sick we would otherwise have risked them dying while waiting to be seen.
We maintain a comprehensive intervention in the camps in Maiduguri and outside through a four-day distribution campaign of food and non-food items like mosquito nets, jerry cans, mats, blankets and soap. We ran a mobile clinic simultaneously, doing medical screening as well as treating systematically, and giving preventive treatment like measles vaccination and seasonal malaria prophylaxis.
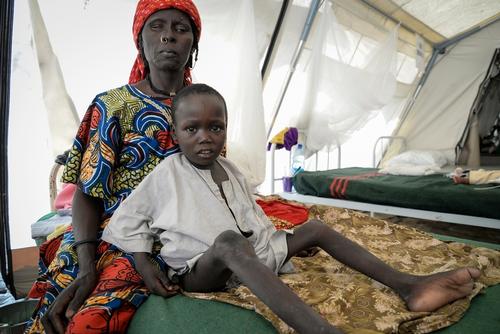
What are your main concerns for the future?
The rainy season has been short, with little rains, so it created the optimum conditions for mosquitos to develop in small water pools. When the hot season comes, the whole population will still be weakened by malnutrition as well as exposed to the massive risk of malaria, exacerbated by the crowded conditions.
People have missed the rain and therefore the planting season. Their villages have been destroyed, livestock stolen, fields and crops looted and torched. They will need as much, if not more, support in the Maiduguri camps and community.
There are some people returning and some businesses and shop merchants bring a sense of normalcy, but this crisis is still unfolding. And, there must be a comprehensive and collaborative approach, including food distribution by aid agencies and authorities.
MSF has three projects in Maiduguri. In Gwange, MSF runs a 102-bed ITFC where we hospitalise children with severe acute malnutrition and complications. In Maimusari, MSF runs an inpatient department (IPD) and outpatient department (OPD) and provides care to malnourished children in their community with an ambulatory therapeutic feeding centre (ATFC). We also provide safe delivery care. Our emergency obstetrics team cares for mothers and their newborns, whose lives are most at risk around the time of birth. In Bolori, we provide general health services and nutrition care in an OPD and ATFC, as well as emergency obstetric services.