Early Thursday morning, an MSF mobile clinic team leaves Wardher town with two Landcruisers in the direction of Ton-Habalan, a remote village a two-hour off-road drive away on red sandy roads. Three mobile clinic teams, made up of a nurse activity manager, an outreach supervisor, a nutrition assistant, a midwife, clinical officers, a pharmacist and drivers, provide primary healthcare in 17 remote locations in Doolo zone, a vast and sparsely populated arid area in the eastern most part of Ethiopia’s Somali region, bordering Somalia.
The vegetation along the route is dry, the water scarcity palpable. It’s the end of March, the hottest and driest time of year, when temperatures quickly rise to over 40 degrees Celsius. From time to time, the convoy passes camels and goats. Over the radio, the driver of the first car warns the others to drive cautiously, to not scare or hit the precious livestock. “Geel, geel, geel,” the driver warns for camels, “adhi, adhi, adhi,” for goats; only once does he say “gaariga” for an approaching car.

Scarce water means a balancing act for life
Pastoralist life in Somali region means moving from place to place, searching for water and pasture to feed livestock. With hardly any access to reliable water, every aspect of life depends on the main seasonal rains, usually expected in April. When they arrive, the rains collect in ponds called ‘berkits’, which provide water for people and their animals. The rains also generate pastures that feed the livestock, which in return provide milk and meat, the staple food in the region. Camels and goats are central to Somali culture and survival in extreme and harsh climatic conditions.
The MSF convoy occasionally passes a child or grown-up with a yellow plastic canister, on their way to fetch water. A young boy stops the cars and asks for water to drink. He looks dehydrated and he still has around 25 kilometres to walk to the closest not-yet-dried-up berkit to fetch water for him and his family.

Two hours later the team sets up their mobile clinic under a wide tree in the village of Ton-Habalan. The tree’s grey-green leaves – a rare sight in the arid environment – provide shade to the team and their patients in the rising and increasingly stifling heat. The weekly mobile clinic is the only health service in the area providing primary healthcare, antenatal and maternity care, child malnutrition screening, and monthly distributions of therapeutic food supplements to the families of malnourished children.
The village is home to maybe 420 households, with many more pastoralist families living scattered in the surrounding bush and visiting the village regularly to trade basics such as sugar, tea, water, tools and simple cooking items for animals, milk and meat. Many of the conversations this morning circle around empty berkits and the anxiously awaited rains, and what could happen if they fail again.
Heat and lack of water makes for difficult conditions
Thirty-eight-year-old Muhabba walked for two hours with her small son to the clinic. The previous week the boy was too sick and weak with fever and a throat infection to walk. The fever abated so he could make the long walk this time.
“The previous droughts eradicated much of our livestock,” Muhabba says, while she waits for her son’s consultation. “In the bush, we were all affected. Only a few animals survived. I am lucky I could raise some of my herd again. I now have 18 goats. It is all I have. We need the rains to survive. We are hoping for God to bring us good rains this year so that our animals and we stay alive.”
During the devastating drought in the Somali region in 2017, 75 per cent of livestock were lost. Since then, few livestock herds have recovered to their previous size.
MSF clinical officer Abdi Abdullahi Abshir checks on a little boy with tonsillitis. “Some of our patients walk as far as three hours to reach us,” he says. “Most health complaints these days are related to the hot and dry climate, the difficult living conditions in the bush and scarce and dirty water. Today the team saw mostly upper respiratory infections. We also treated many women with urinary tract infections.”
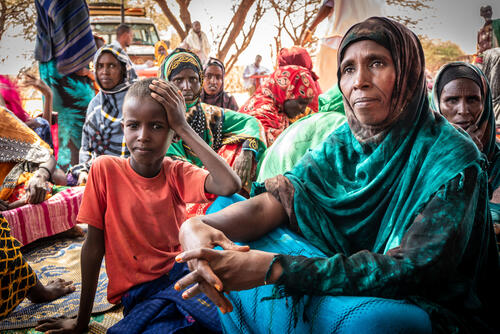
Providing desperately-needed healthcare in an isolated area
It turns out to be one of the busiest days since MSF started providing healthcare in Ton-Habalan in 2018. Communities increasingly know about the services and every week more patients come. The team has seen 208 patients by 2pm, when it is time to pack up for the day and return to the MSF base in Wardher town.
On the way back, the convoy picks up a former patient. “The young man has insulin dependent diabetes and was treated by MSF when we were working in Wardher hospital last year,” says MSF nurse activity manager Maren. “Now we give him a ride whenever we pass him on his walk from his village of Wal-Wal to Warhder. The remaining days of the week, he has to walk 12 kilometres to the hospital to get his daily dose of insulin, which needs to be cooled in a fridge. It is impossible for him to keep insulin at home as his village has no electricity.”
In this isolated region, even under normal circumstances, it is near impossible to get timely emergency care. The existing healthcare system does not cater to pastoralists, who are continuously on the move. Distances to health care are overwhelming and can be life-threatening.
Only a few ambulances serve a population of more than 300,000 in Doolo Zone, who are dispersed over a vast area without any paved roads, most of the time they are broken down or used for other purposes by the authorities. It forces people to find alternative means of transport, which often involves having to pool funds to fuel private vehicles – which are not even available in most locations – or walking for hours on foot, sometimes, but rarely, on camels.

MSF provides flexible mobile primary healthcare services in 17 mobile clinics, like the one in Ton-Habalan village. The mobile set up permits the teams to move locations quickly, following the pastoral communities to places where no health posts exist. Since the beginning of 2019, the number of patients has consistently increased. A good indication that we reach the right sites and communities.
By the end of March, MSF teams had treated over 4,500 patients, mostly for upper respiratory tract infections, skin infections and urinary tract infections. The number of pregnant women coming for antenatal care has doubled to more than 400 consultations in March. MSF’s ambulance referred an average of five emergency patients per fortnight to the hospital in Wardher town. Many emergency referrals are pregnant women with complications or with obstructed labour.

Failing rainy seasons over the past years have caused prolonged and persistent droughts. Affected pastoralist families began traveling long distances in search of water, food and grazing grounds. Unstable and unreliable food and water sources, unhygienic living conditions in cramped sites for displaced people near villages and towns, in combination with the poor coverage of health services not only leads to tensions, but also results in disease outbreaks, malnutrition, and the loss of lives and livestock.
If the rains fail again this year, the fragile balance could quickly turn into an emergency, endangering the health and lives of the most vulnerable in Doolo zone: nomadic pastoralists and displaced communities.
MSF has worked in Ethiopia’s Somali region of Ethiopia since the 1980s, supporting various government health facilities.
In Doolo zone, MSF had worked in Wardher hospital and health centres in Danod and Lehel-Yucub since 2007 until handing over activities in these facilities to local partners in 2018. Since then, activities focus on comprehensive primary healthcare through mobile clinics, community engagement, surveillance and health promotion activities to an extensive area and to remote populations, in addition to emergency preparedness and disease outbreak response management. MSF runs 17 mobile clinics and monitors 17 remote surveillance locations for early detection of disease outbreaks, and a timely response to emergencies.











