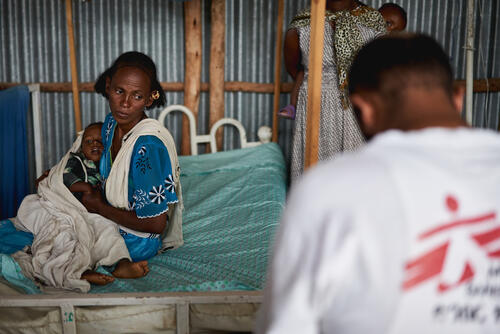
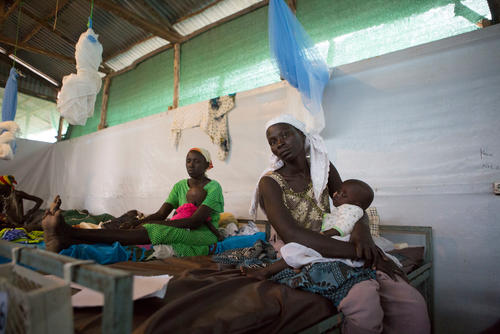
Ephraim is in one of the small counselling rooms of the MSF mental health centre in Hitsats refugee camp, in northern Ethiopia. Being able to tell his story in detail, while remaining emotionally stable is an important step in his therapeutic process.
“I was studying in ninth grade and I knew that I had to do military service soon. For some people it never ends and while you are in the military they pay you almost nothing,” he says. “For me it was clear that I did not have a future, not a future where I could freely choose what to do and be, and where I could provide for my family. So I decided to leave, like many other Eritreans.”
Now, 17 years old Ephraim was only a child of 14 when he first left Eritrea.
Reasons to flee
Each month, approximately 5,000 people flee Eritrea and many of them are teenagers just like Ephraim. The mandatory indefinite military service imposed on all Eritreans by an oppressive regime that deprives them of basic human rights is a major push factor for those who flee the country.
For those who stay, the ‘choice’ is not without cost: arbitrary detention, violence and intimidation are known to be used against those who do not conform to the system .
Ephraim has had his fair share of abuse and detention, both in Eritrea and while on the search for a better life. At one point in his journey, he was caught in Sudan while attempting to reach Libya. With very little food and water, the 13-day long trip across the desert almost killed him. He was beaten and jailed for several weeks before being sent back to Eritrea where he was imprisoned again.
“The prison in Eritrea was like a hole in the ground, with no windows and no lights. There were more than 80 people in the room with me. We didn’t have enough space to lie down so we spent every night sitting and taking turns to sleep.”
His mother managed to have him released and Ephraim tried to leave the country again.
“The soldiers caught me at the border, beat me up badly and sent me back to prison”, Ephraim says. “The injuries from the beating were getting worse. I started coughing and I couldn’t sleep because the floor was too hard and painful. I did not receive any medical help until things became pretty bad. At that point I was sent to the hospital. I was treated and sent back to the prison.”
Finally, on his third attempt, Ephraim managed to reach the refugee camps in northern Ethiopia.

Consequences on mental health
Despite the extreme challenges, Ephraim’s story is not unique. Many other Eritreans have gone through similar ordeals. While experiences like these can surely cause physical problems, the mental health consequences are far more complex to identify and treat, and their impact can be devastating.
In an effort to offer Eritrean refugees comprehensive health care, in 2015 MSF started a mental health project for the people in Hitsats and Shimelba refugee camps. With around 2,300 new monthly arrivals, refugee camps in northern Ethiopia are one of the first destinations for Eritreans leaving their country. Robel Araya, MSF Mental Health Supervisor in Hitsats camp, is very familiar with the situation faced by Eritrean refugees.
“Most of the people that we see in the camps have been through traumatising experiences. Leaving Eritrea is dangerous and some of them have made several attempts before succeeding”, Robel says. “Many develop depression, anxiety and post-traumatic stress disorder linked to torture, violence and abuse. These conditions have a very negative effect on their lives. Our mental health services can help them get back on their feet.”
The prison in Eritrea was like a hole in the ground, with no windows and no lights. There were more than 80 people in the room with me. We didn’t have enough space to lie down so we spent every night sitting and taking turns to sleep.
MSF offers counselling, inpatient and outpatient psychiatric care and a wide range of therapeutic activities, including therapeutic discussions and psycho-education, where patients can discuss what they are going through and receive detailed information about their conditions and how to overcome them. Realising that other people are experiencing similar problems helps them feel less isolated.
As is the case for the majority of humanitarian settings, children are one of the most vulnerable groups.
“Around 40 per cent of the camp population is aged under 18. Half of them are travelling alone or have been separated from their families”, Robel says. “Their situation is very delicate. They tend to suffer from separation anxiety and in some cases, they had difficult or confusing early sexual experiences. Here we have activities specifically designed for them, like sport, drawing and theatre sessions, as well as specialised counselling.”
The population in the camps is very transient. It is estimated that around 80 per cent of Eritrean refugees will continue onwards through Sudan and towards Libya along the Central Mediterranean route within 12 months of their arrival in the Ethiopian refugee camps.
The harsh living conditions in the camps, the lack of future perspectives, the desire to reunite with family members in other countries and the young average age seem to greatly contribute to these secondary movements.
“Our outreach activities in the community need to be constant because the population is always changing”, Robel says. “The few who stay for the long term do so because they do not have the money to move further. We also see people who tried to leave but were caught in Sudan or Libya, where they have seen and experienced horrible things, and were sent back to Ethiopia even more traumatised than before.”
Challenges in providing care
One of the main challenges is convincing people to seek support. The fear of being labelled as ‘weak’ or ‘crazy’ by the community prevents many from coming forward.
“At first we encountered a lot of difficulties talking about mental health with refugees. So we decided to hire Community Mental Health Workers (CMHW’s) from the refugee community to provide door-to-door culturally appropriate awareness raising, education and de-stigmatisation of mental health” Robel says.
Every day, the CMHWs go from shelter to shelter and explain in detail how mental health issues manifest themselves, that treatment is available and why it is important to seek help. These sessions usually involve a whole family at one time, and in their native language.
“Now we have a team of 26 very motivated CMHWs. It helps that many of them are our former patients and have experienced first-hand the benefits of counselling and treatment”, Robel explains. “Being Eritrean, they know how to properly address the topic with the rest of the camp’s population. Their commitment comes from wanting to help their community.”
SimonThe name was changed at the request of the interviewee to protect his identity. is one of MSF’s CMHWs in Hitsats camp. Like the other members of the team, he is an Eritrean refugee and a former patient.
“When I first arrived in the camp, I was not doing well. I was constantly reliving all the things that I experienced when first trying to cross the border, and while in jail, like the shooting, the torture and the abuse”, he says. “The counselling really helped me get my life back together and I realised that this is something I could help other people with.”
“Working as a social worker in the MSF mental health programme here in Hitsats camp is the only thing that gives me stability and motivation. Having a purpose has helped me not to think too much about further movements and the fact that I miss my family, my friends and my home”, Simon says. “A lot of people here suffer from trauma and mental health problems. When I see that they get better because of the support I provide through my work, I feel like staying here is worth it. Even if I didn’t manage to become a nurse like I was dreaming when in Eritrea, I am still able to help people and this makes me very happy.”

Hitsats and Shimelba refugee camps host around 10,000 and 6,000 people, respectively. MSF provides around 2,800 individual counselling sessions and 3,600 psychiatric consultations per year in the camps. In addition to the mental health programme, MSF offers primary and secondary healthcare services, including a 24/7 inpatient care in Hitsats refugee camp in partnership with the Ethiopian Administration for Refugee & Returnee Affairs (ARRA), and ambulance referral services for emergency patients to the nearby Shire hospital. Reproductive health awareness and HIV prevention are also provided at community level.