Despite decades of international aid and investment, people in Afghanistan still struggle to access basic and emergency medical care due to insecurity, distance, cost and the fact that many health facilities lack the staff and equipment they need.
The effects of active fighting and indiscriminate violence permeate every aspect of daily life, and this includes seeking medical care. MSF teams fill significant gaps in healthcare in the areas where we work, however people’s needs for healthcare remain high.
Care in one of the most dangerous places in the world to give birth
Afghanistan has one of the world’s highest rates of maternal mortality; an estimated 4,300 women die yearly due to complications during pregnancy or childbirth.
Many births take place at home, without assistance, either because of a shortage of female medical staff to look after women in labour, or – outside of big cities – most women don't have adequate access to obstetric care or can't afford it.
We work in one hospital in Helmand province in collaboration with the Ministry of Public Health. Our services range from maternal and paediatric care to vaccinations and treatment for malnutrition.
We also run a maternity hospital in rural Khost province, in eastern Afghanistan, where our work is strongly focused on complicated deliveries.
We place an emphasis on training local female staff through our projects in Afghanistan. Almost all the midwives are Afghan women, some of whom have become highly experienced in managing complicated deliveries since we opened our maternity hospital in Khost in 2012.

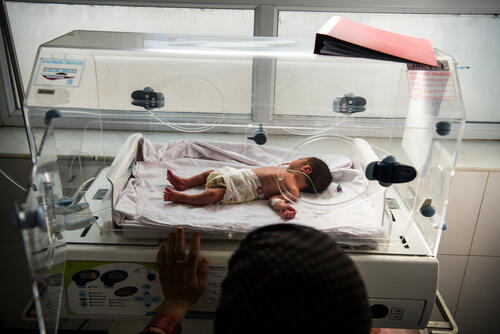
Khost, Afghanistan's biggest maternity hospital and MSF's busiest
The inpatient department at our hospital in Khost includes a 60-bed maternity unit and a 28-bed newborn unit. We also run two operating theatres and offer comprehensive emergency obstetric care, vaccinations for newborn babies, family planning, health promotion and a women’s health clinic.
MSF is one of the largest employers of women in Khost: we employ around 430 people, as cleaners, nurses, midwives, nannies and doctors; the majority are women.
In the peripheral districts of the province, we support eight health centres to increase their capacities, allowing them to assist simple deliveries, making it easier for mothers to give birth close to their homes.
Dasht-e-Barchi
We also had a team at the maternity wing of Dasht-e-Barchi hospital, in Kabul’s west, which provided the only 24-hour maternal care for emergency and complicated deliveries in a neighbourhood of more than one million people.
On 12 May 2020, the maternity wing was attacked by an unknown armed group, seemingly targeting mothers in the wards. During the four-hour attack, 16 mothers were killed, as were two young boys and an MSF midwife. In June 2020, we announced that we had made the difficult decision to withdraw from Dasht-e-Barchi.
Drug-resistant tuberculosis
The burden of tuberculosis (TB) is increasing in Afghanistan. The World Health Organization estimates that 61,000 people are infected annually, causing around 12,000 deaths every year.<a href="http://www.emro.who.int/afg/afghanistan-news/tuberculosis-burden-increases-in-afghanistan-with-over-60-000-new-cases-every-year.html">World Health Ogranization: Tuberculosis burden increases in Afghanistan with over 60 000 new cases every year, 28 March 2017</a>
We diagnose and treat drug-resistant tuberculosis (DR-TB) in Kandahar province, in partnership with the Ministry of Public Health, and run a laboratory and facilities to host patients during their treatment in Kandahar city.
In December 2019, we introduced a nine-month oral regimen allowing DR-TB patients to change from injectable drugs to pills and reduce their number of consultations at the hospital. The shorter, all-oral treatment produces fewer side effects and improves the patients’ quality of life.
We also provide support to Mirwais regional hospital, and organise training for other facilities in Kandahar to improve the detection of TB, including drug-sensitive cases.

Treatment for TB in Kandahar
Trauma centre in Kunduz
On 3 October 2015, our trauma centre in Kunduz was destroyed in airstrike attacks by the US military. Forty-two people were killed, including 14 of our staff. The hospital had opened in 2011 to give much-needed quality medical and surgical care to victims of violent and non-violent trauma.
A wound care clinic opened elsewhere in the city in 2017, and construction on a new Kunduz Trauma Centre started in 2018. The new centre – with 30 beds and an operating theatre – opened in August 2021.
Teams at the trauma centre see people injured during the fighting, and many people are injured in road traffic accidents, suffering head trauma injuries. We do not have the capacity to provide neurosurgery and other facilities in the area that would normally have capacity are currently not providing that service; this is a stark illustration of the gaps in healthcare that have long existed, and are as acute as ever now.
High health needs in Herat
Since December 2019, MSF has been supporting the Herat Regional Hospital’s 40-bed Inpatient Therapeutic Feeding Centre (ITFC), for severely malnourished children. The majority of patients and caretakers travel more than 15 kilometres to come for care, with some travelling over 300 kilometres.
We also run a clinic for internally displaced and local people, offering general consultations – including for non-communicable diseases – screening and treatment of malnutrition, ante- and post-natal consultations, and childhood vaccinations.
MSF has been assisting the COVID-19 pandemic response by triaging cases in Herat Regional Hospital since April 2020, and running a COVID-19 treatment centre in Gazer Gah. This centre helps to increase the region’s bed capacity for patients in need of oxygen and has so far been operational three times, opening in response to different waves of the pandemic.



