September 2018 update on activities in Cox's Bazar district, Bangladesh, providing care for Rohingya refugees who have fled Myanmar.
- Over 13,000 people have been registered by the United Nations refugee agency, UNHCR, as new arrivals so far in 2018.
- Cyclone season will begin in October. Most buildings in the camps, including medical facilities, are extremely vulnerable to cyclone damage. And cyclones also bring heavy rains that could cause further flooding and landslides.
- There are concerns about whether there are enough inpatient beds to meet the needs of the Rohingya and Bangladeshi population in the area, and referrals may become more difficult if movement restrictions on Rohingya patients increase.
Operational summary
NUMBER OF HEALTH FACILITIES: 4 inpatient health facilities (hospitals), 5 primary health centres, 8 health posts and 1 outbreak response centre (details below).
NUMBER OF STAFF: More than 2,000 MSF staff and over 1,000 volunteers continue to respond to the health and water and sanitation needs of the Rohingya refugees and host communities.
NUMBER OF PATIENTS: Between August 2017 and the end of September 2018, our teams have carried out 843,800 outpatient consultations and 15,434 admissions.
MAIN MORBIDITIES: Respiratory infections, diarrheal diseases and skin diseases.
WATER AND SANITATION: Activities include drilling boreholes, setting up water distribution systems, desludging old latrines, bucket chlorination and distributing domestic water filters.
OUTREACH: Outreach teams focus on health promotion in both refugee and host communities, investigating possible outbreaks, conducting vaccination campaigns and maintaining links with community and other organisations.

Recent developments
Over 13,000 people have been registered by the United Nations refugee agency, UNHCR, as new arrivals so far in 2018. This includes people who have been forced or asked to leave their homes within the host community and move to refugee camps.
Those arriving from Myanmar tell MSF teams of continuing violence, harassment, detention and coerced registration as “non-citizens”.
Border controls on both sides of the border have reportedly been intensified making it more difficult for refugees to reach Bangladesh.
The island
Bangladesh plans to start relocating Rohingya refugees to a remote island in the Bay of Bengal called Bhasan Char. It is intended eventually to house 100,000 people, beginning with 50 to 60 families who may be relocated as early as October.
This small island only emerged from the sea in 2006 and there are serious concerns that it could be vulnerable to extreme weather. There are also concerns that Rohingya refugees will not be able to leave the island even for medical treatment.
Insecurity, violence and protection
Refugees have reported concerns about violent attacks in the camps, including abductions and kidnappings. MSF teams hear stories from patients, and Rohingya volunteers report fearing for their safety. In response, many camp authorities have now introduced curfews and law enforcement patrols have been increased, particularly at night.
MSF is concerned that the limitations on movement as a result of curfews may prevent patients from accessing emergency healthcare during the night.
Possible reduction in activities of other organisations
MSF is concerned that other organisations working in the camps may begin to reduce their activities because they have not received funding. While some consolidation of activities is necessary to avoid overlap, any significant reduction in activities in the near future risks leaving serious gaps and potentially overwhelming MSF’s capacity to provide medical care.
Cyclone season preparations
Cyclone season will begin in October. Bangladesh experiences regular cyclones. Emergency measures such as evacuation plans and cyclone shelters, however, are not available to refugees.
MSF and other organisation are preparing to respond but most buildings in the camps, including medical facilities, are impermanent structures made of bamboo and plastic sheeting, so any cyclone activity is likely to cause serious damage. Cyclones also bring heavy rains that could cause further flooding and landslides.
Uncertainty about the future
Uncertainty about the future remains a major concern for refugees and continues to affect their health. Any return of the refugees to Myanmar must be voluntary, safe and dignified.
MSF continues to calls on governments able to influence Myanmar, to press for violence and discrimination against Rohingya to stop, for refugees to be able to return to their place of origin, and for restrictions on freedom of movement for Rohingya remaining in Myanmar, and for access for humanitarian organisations, to be lifted.
In the meantime, Rohingya in Bangladesh should be granted refugee status or other legal status and have access to services.
Still no longer-term solutions in the camps
There is a need for longer-term planning to secure a safer and sustainable living environment for the Rohingya refugees. This includes continued international support. Camp-level planning must bring infrastructure up to minimum standards.
The extent and the urgency of the humanitarian crisis and the real risks need to be widely appreciated.

Current health concerns
There are concerns about whether there are currently enough inpatient beds to meet the needs of the Rohingya and Bangladeshi population in the area.
MSF is one of the main providers of hospitalisation for paediatric, neonatal and adult patients. Non-communicable diseases (NCDs) also remain a serious unmet need.
Surgical capacity is an area of concern as surgical facilities within the camps are limited and these may also be reduced over time.
Both international and national organisations need more support, including funding, to scale up secondary healthcare and surgical care.
MSF has so far also been able to refer patients from both the host and Rohingya communities to facilities in Cox’s Bazar. This may become more difficult if movement restrictions on Rohingya patients increase.
Routine vaccinations
MSF is working with the government of Bangladesh to expand routine immunisation (vaccinations) for Rohingya refugees.
Currently vaccinations are available for children up to one year old. We hope that this will eventually be expanded to all children under five years to address the historically low vaccination coverage among the Rohingya, as a result of limited access to healthcare in Myanmar, and to prevent communicable diseases.
Mental health
Only a small proportion of the population currently has access to specialised mental health services, such as those provided at MSF facilities.
The traumatic experiences that forced them to flee Myanmar, their hazardous journeys, the daily stresses of camp life and uncertainty about their future all negatively affect Rohingya refugees’ mental health. They experience flashbacks, generalised anxiety, panic attacks, recurring nightmares and insomnia, as well as illnesses such as post-traumatic stress disorder and major depression.
MSF is also seeing chronic mental health difficulties and psychiatric needs within both the host and refugee communities.
Sexual and gender-based violence (SGBV)
Progress has been made in putting in place sexual and gender-based violence (SGBV) prevention, mitigation and response mechanisms, but coverage and service delivery remains patchy.
MSF teams continue to provide support and treatment to victims of sexual violence at our health facilities. Since August 2017, MSF has treated more than 600 patients, who have reported experiencing sexual violence both in Myanmar and in the camps.
MSF’s services include psychosocial care, treatment for sexually-transmitted infections (STIs) and menstrual regulation (Bangladeshi medical term for termination of unplanned pregnancies). Post-exposure prophylaxis is also provided where possible.

Water and sanitation
Given the scale of the water and sanitation needs, MSF’s water and sanitation response has shifted to focus on larger projects to distribute clean, treated water, and the management of waste from latrines. Maintenance of existing facilities, chlorination points and distribution of aquafilters also continues.
While the distribution of aquafilters to patients leaving the hospital and identified vulnerable households continue, other activities will gradually be phased out as MSF focuses on the development of water distribution systems. Several systems are already in operation.
One of the systems under construction is a solar-powered water network to bring clean, chlorinated water to 81,000 refugees. This system will allow for “in-line chlorination”, meaning the water is treated as soon as it is pumped out of the borehole. The chlorine in the water ensures that the water is safe while it is stored in the large water-tanks (between 75,000 and 90,000 litres each). Once the water is collected from taps near people’s shelters, the chlorine will also keep the water safe as it is stored in the household.
MSF health facilities and services
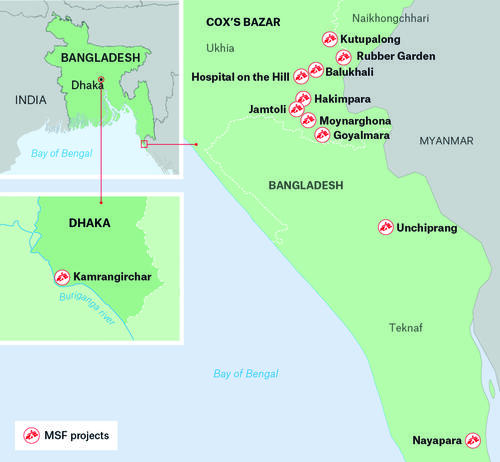
MSF teams are providing a wide range of health services for Rohingya refugees living in formal and informal camps, as well as for the local host population around our facilities.
Inpatient facilities (hospital-level facilities)
MSF operates four hospital-level inpatient facilities in the Cox’s Bazar district: Kutupalong IPD, Balukhali IPD, the Hospital on the Hill (Kutupalong-Balukhali mega-camp), and Goyalmara Mother and Child Hospital between Moynarghona and Unchiprang camps.
Goyalmara Mother and Child Hospital and Kutupalong IPD are located just outside of the camps and serve both camp and host populations. Indeed, 40 per cent of patients at Goyalmara are from the host community.
The four hospital-level facilities offer a range of services including:
- Emergency, outpatient departments and inpatient departments, and isolation beds/wards,
- Sexual and reproductive health services, including maternity, neonatal and paediatric facilities,
- Mental health services,
- Sexual and gender violence services, and
- Laboratory services.
Rubber Garden outbreak response centre is now an emergency facility that can be activated in case of an outbreak of a communicable disease like cholera or diphtheria. It has a capacity of 100 beds. It is one of the few dedicated facilities that would be available in the case of an outbreak, as finding space to implement isolation and treatment activities in the Kutupalong-Balukhali mega-camp is extremely challenging.
Primary health centres
MSF operates five primary health centres in the camps south of the Kutupalong-Balukhali mega-camp (in Hakimpara, Jamtoli, Moynarghona, Unchiprang and Nayapara camps).
These primary health centres are outpatient facilities that provide primary healthcare, as well as 24-hour emergency and ambulance referral, mental health and sexual and gender-based violence services. Each primary health centre sees 200 to 300 patients a day.
The medical teams at Hakimpara, Jamtoli and Moynarghona primary health centres are currently revising their protocols in order to constantly improve the quality of care. Unchiprang primary health centre was damaged by strong winds earlier in the year but has now been repaired. At Nayapara primary health centre, construction has begun on a maternity facility.
MSF teams are also working with local communities and health facilities to improve outbreak readiness and infection prevention and control. Nayapara primary health centre will start a mobile clinic programme from October, to bring healthcare closer to where people live.
Health posts and mobile clinic
MSF runs eight health posts or outpatient departments in Kutupalong-Balukhali camp. All provide basic primary healthcare, including vaccinations, and sexual and reproductive health and mental health services. Some also provide follow-up for patients with non-communicable diseases such as hypertension, diabetes, chronic obstructive pulmonary disease, asthma and epilepsy.
The mobile clinic that was providing screening, consultations and referrals at Sabrang entry point, where many refugees arrived last year, is on standby as very few people are now arriving at this point. An MSF social worker continues to monitor the situation and the mobile clinic can be reactivated quickly if needed.
Supporting government health facilities
In Cox’s Bazar town, MSF is starting construction at Sadar Hospital, one of the main hospitals in the town. MSF is building a brand new waste management area for the hospital as part of a project to support the hospital to improved infection prevention and control. The hospital serves both host and Rohingya populations.
MSF is supporting mental health services at Ukhiya Upazila Health Complex in Ukhiya town, near the largest of the refugee camps.
In August, MSF also donated and installed an x-ray machine at the Teknaf Upazila Health Complex and provided staff training.






