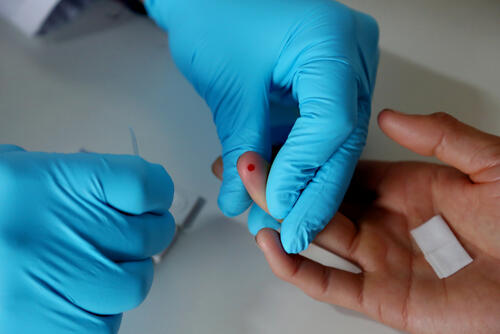
Confronting a deadly pandemic
Over 39 million people were living with the human immunodeficiency virus (HIV) at the end of 2022, the majority of them in sub-Saharan Africa. While there is no cure for HIV, a combination of drugs, known as antiretrovirals (ARVs), enable people to live longer, healthier lives if taken regularly. The cost of first-line drugs is now cheaper than ever, but efforts are still needed to ensure everyone who is living with HIV receives treatment.
Globally, 29.8 million people living with HIV were receiving ARVs in 2022. This equates to a global ARV coverage rate of 76 per cent. However, only 57 per cent of children were receiving ARV treatment at the end of 2022. (All figures UNAIDS)

31,500
31,5
6,570
6,57
Quick facts about HIV/AIDS


Worldwide, around 14 per cent of people currently infected with the virus don't know their HIV status. In West and Central Africa, one in five people living with HIV didn't know their HIV-positive status at the end of 2022. Once someone is diagnosed with the disease, viral load monitoring - measuring the levels of HIV virus in the blood - is essential to measure whether treatment is working. While annual viral load tests are standard in wealthy countries, access in developing countries still lags far behind.


There is no cure for HIV, although life-long treatment using combinations of drugs known as antiretrovirals (ARVs) helps manage the virus and enables people to live longer, healthier lives if taken regularly. While 22 million more people are on treatment today than in 2010, deadly treatment gaps still exist, especially among children. In the Middle East and North Africa; in the latter, only half of people living with HIV receive ARVs, while the number in Eastern Europe and Central Asia is 51 per cent.


While most people living with HIV can stay healthy on first-line antiretrovirals - which cost around US$63 per person per year – some people develop resistance to this regimen and have to switch to second-line regimens. But the price of doing so is high - literally. Second- and third-line regimens are over four times the price of first-line regimens.


In conflict settings and when people are displaced, ensuring the continuity of care for people with HIV - including long-term supply of drugs - can be difficult. Logistical and security issues are barriers for both our teams and patients in ensuring that people living with HIV can access the care and treatment they need to stay healthy. In Yemen, providing uninterrupted treatment during years of war has proved logistically challenging - and dangerous to our staff and patients.

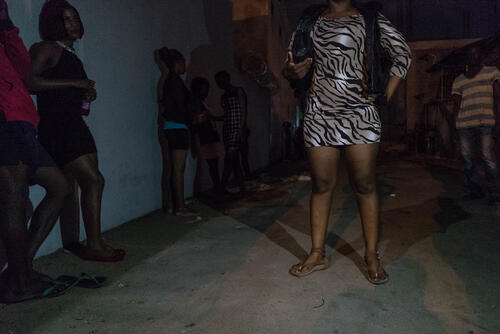
So called ‘key populations’, or groups of people, include people who are disproportionately affected by HIV, including sex workers, people who inject drugs, men who have sex with men, and prisoners. Despite their higher risk of acquiring HIV, these key groups are often excluded from accessing HIV treatment and prevention as well as comprehensive health services. Stigma, discrimination, social exclusion, violence and criminalisation are part of their daily struggles. In Mozambique, MSF provides packages of HIV and sexual and reproductive healthcare services for sex workers and men who have sex with men in key sites.

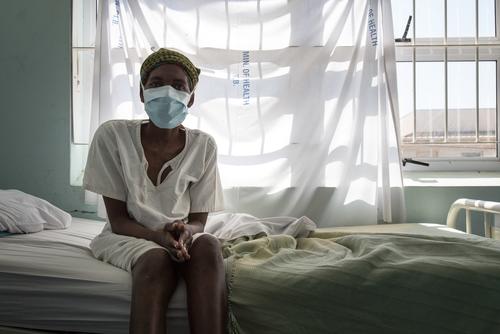
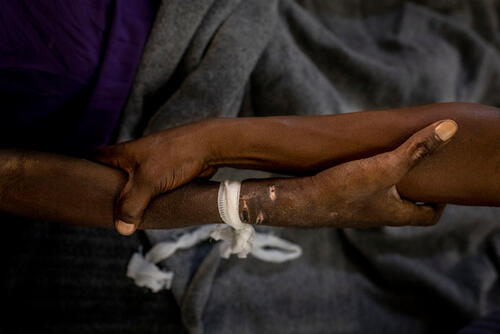
HIV lowers the body's immune response, and without effective treatment, leaves people living with the disease much more vulnerable to deadly opportunistic infections like tuberculosis (TB). TB is the single biggest killer of people living with HIV, accounting for the death of 214,000 people living with HIV in 2020.

Pharmaceutical corporations are failing children with HIV

HIV and TB treatment at risk as countries gradually lose Global Fund support

Diagnosing, treating and researching HIV-kala azar co-infection in Ethiopia
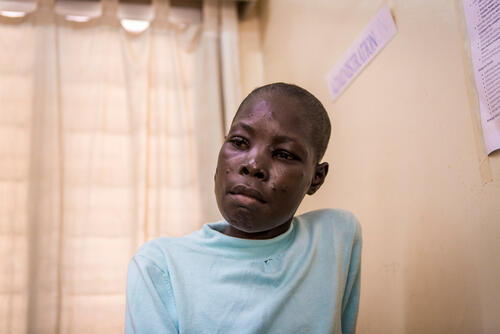
Stopping Senseless Deaths: Overcoming access barriers to affordable, lifesaving diagnostics and treatments for HIV and opportunistic infections

Pfizer and GSK’s HIV/AIDS division, ViiV, prevents children with HIV from getting needed medicine
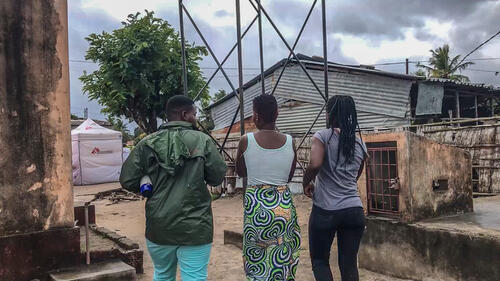
Towards Peer-Led HIV and SRH Services for Sex Workers and Men Having Sex with Men

Meeting the specific needs of key populations living with HIV

AIDS 2018

MSF at AIDS 2018
Research & Publications
Burden sharing or burden shifting? How the HIV/TB response is being derailed

Treatment scale-down ahead?
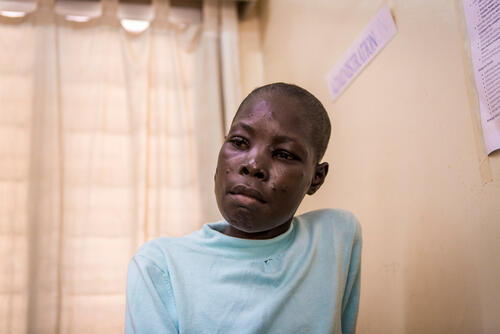
Stopping Senseless Deaths: Overcoming access barriers to affordable, lifesaving diagnostics and treatments for HIV and opportunistic infections
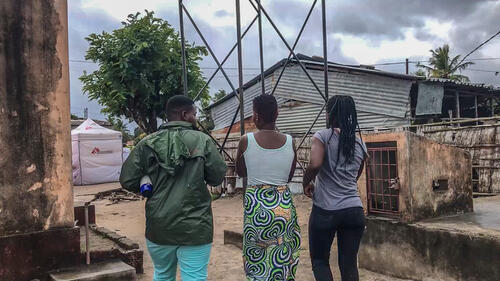
Towards Peer-Led HIV and SRH Services for Sex Workers and Men Having Sex with Men
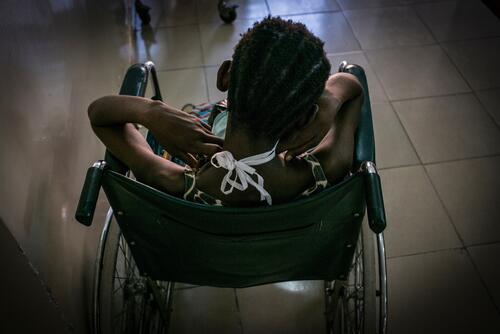
Left behind by the HIV response - Kinshasa
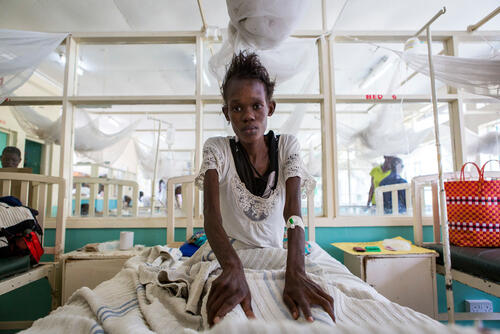
MSF at IAS 2017
MSF publishes study on the accuracy of HIV rapid diagnostic tests
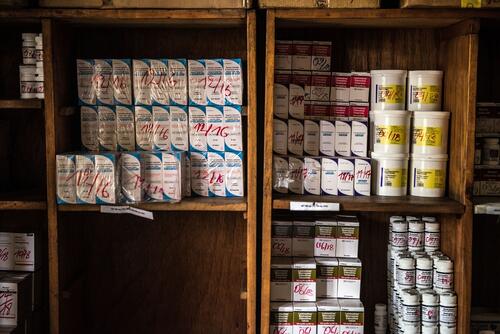
Untangling the Web of Antiretroviral Price Reductions 18th Edition
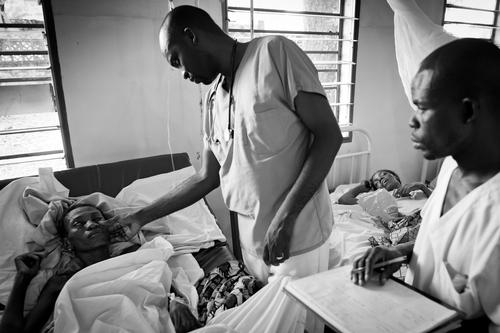
Fight against HIV doomed to fail without urgent focus on West and Central Africa
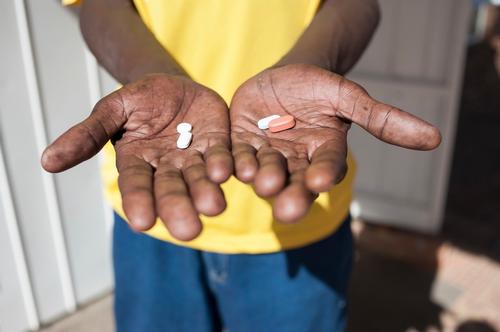
HIV: Antiretroviral drugs fail to consistently reach patients in countries most affected by HIV/AIDS
MSF HIV/AIDS Research
fieldresearch.msf.orgWe produce important research based on our field experience. So far, we have published articles in over 100 peer-reviewed journals. These articles have often changed clinical practice and have been used for humanitarian advocacy. Read all our HIV/AIDS-related articles on our dedicated Field Research website.